
(© Casimiro - stock.adobe.com)
In A Nutshell
- Syphilis cases in the U.S. have surged more than 80% since 2018
- Researchers at Tulane University found that adults diagnosed with syphilis faced significantly higher risks of heart attack, stroke, and dangerous aortic swelling or tearing
- The findings suggest doctors treating syphilis patients should consider routine heart health screening, while cardiologists evaluating unexplained blood vessel disease may want to consider testing for syphilis
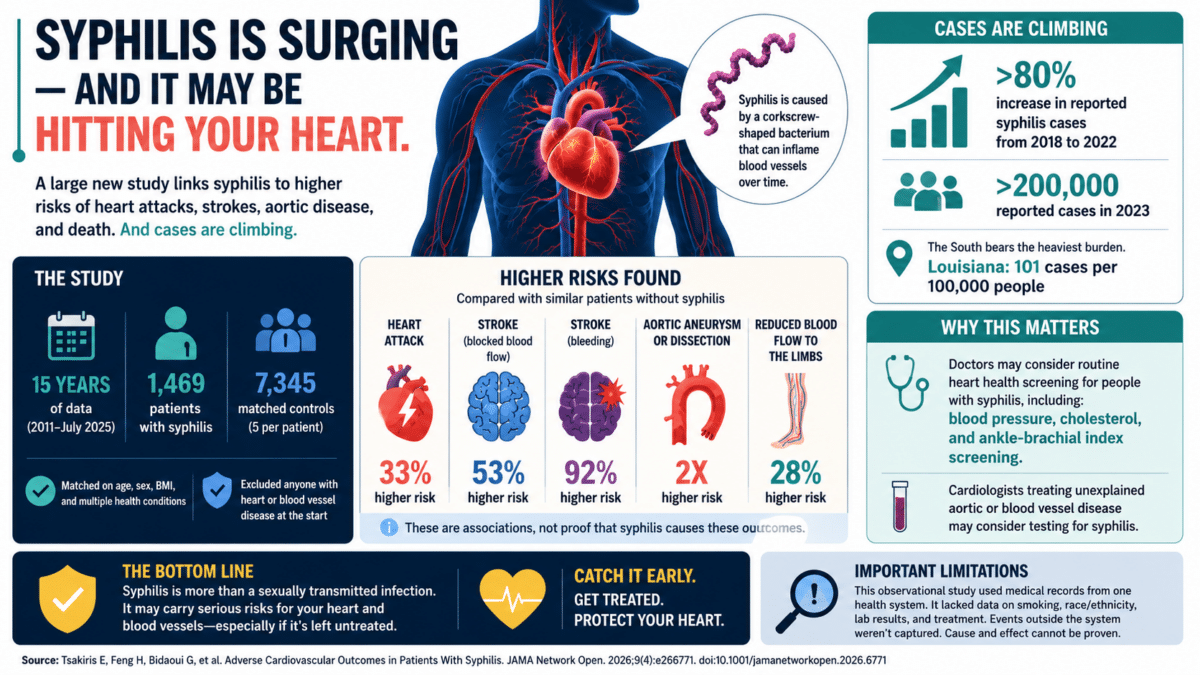
A sexually transmitted infection most people associate with another century is roaring back across the United States, and a large new study suggests it may be doing far more damage than anyone realized. Researchers in New Orleans found that patients diagnosed with syphilis faced sharply higher risks of heart attacks, strokes, and dangerous swelling or tearing of the aorta, the body’s largest blood vessel, compared to similar patients without the infection.
The most alarming signal: the risk of death was nearly six times higher among syphilis patients overall, though the study could not fully account for all factors that may have contributed to that gap. The worst outcomes, across the board, were concentrated in those with late-stage disease.
Reported syphilis cases in the U.S. jumped by more than 80% between 2018 and 2022, topping 200,000 cases in 2023 alone. Southern states bear the heaviest burden, with Louisiana ranking among the highest at 101 cases per 100,000 people. Despite this surge, no modern American study had, to the authors’ knowledge, used matched comparison groups to investigate whether syphilis independently raises the risk of heart and blood vessel disease. Until now.
Researchers at Tulane University School of Medicine set out to answer that question, and the results are sobering. Syphilis, caused by a corkscrew-shaped bacterium, appears to inflame blood vessels over time without obvious warning signs, potentially triggering a cascade of serious problems that go well beyond the infection itself. Published in JAMA Network Open, the study points to a practical shift in how doctors might approach syphilis patients: screening them for heart risk factors. It also raises the question of whether cardiologists treating unexplained blood vessel disease might consider testing for syphilis, though further research would be needed before that becomes standard practice.
How the Syphilis and Heart Disease Study Worked
The research team analyzed electronic health records from three hospitals within a single health care system in New Orleans, covering a 15-year period from January 2011 to July 2025. They identified 1,469 adults diagnosed with syphilis and matched each one with five control patients (7,345 in total) who had never been diagnosed with the infection. The matching was thorough: controls were selected to be similar in age, sex, body mass index, and a range of existing health conditions, including diabetes, high blood pressure, high cholesterol, heart disease, chronic lung disease, kidney disease, liver disease, autoimmune disease, and cancer. Anyone who already had heart or blood vessel disease before the study began was excluded, so the researchers were tracking only new events.
The two groups ended up looking nearly identical on paper. Average age was about 50 in both, roughly 54% were female, and rates of chronic conditions were nearly the same. One exception was body mass index: syphilis patients averaged about 24.9 compared to 28.1 in the control group. Researchers adjusted their statistical models to account for this difference.
Over a follow-up period of about six and a half years, patients with syphilis developed cardiovascular problems at notably higher rates. Heart attacks occurred in 6.9% of syphilis patients compared to 4.2% of controls. Strokes caused by blocked blood flow hit 10.3% of syphilis patients versus 5.7% of controls. Bleeding strokes were more than twice as common in the syphilis group. Conditions where the wall of the aorta balloons out or tears struck 3.3% of syphilis patients compared to just 1.3% of controls.
After adjusting for other health factors, the statistical picture held up. Syphilis patients had roughly double the risk of developing aortic swelling or tearing compared to matched controls. Their risk of a bleeding stroke was 92% higher. The more common stroke type, caused by a blocked blood vessel, was 53% more likely. Heart attack risk was 33% higher, and reduced blood flow to the limbs was 28% more likely. Because this was an observational study, these figures represent associations rather than proof that syphilis directly caused each outcome. Still, the size and consistency of the findings are hard to dismiss.
Not every heart condition showed a link. Heart failure, irregular heart rhythms, a leaky heart valve, and blood clots in veins did not differ meaningfully between the two groups. That pattern makes biological sense: syphilis is believed to damage the lining of blood vessels through long-term inflammation, so conditions rooted in blood vessel injury would logically be most affected, while problems involving the heart muscle or clot formation would not be as directly influenced.
Late-Stage Syphilis Carried the Greatest Danger
One of the study’s most telling contributions was breaking down risk by the stage of infection. Patients with early-stage syphilis showed no statistically significant increases in heart or blood vessel events; though that should not be taken to mean early-stage infection is harmless. It carries other well-known health risks and can progress to more dangerous stages if left untreated. But the cardiovascular picture changed dramatically for patients with late-stage disease.
Among the 195 patients with the most advanced form of syphilis, the risks were severe. Their likelihood of dying was nearly seven times higher than controls. Aortic swelling or tearing risk was more than five times higher. Stroke risk tripled. Heart attack risk was associated with a more than twofold increase. Even heart failure and irregular heart rhythms, which showed no connection in the broader analysis, were about twice as common in this subgroup.
Patients with a form of the disease where the infection lingers without obvious symptoms also showed elevated risks of death, aortic problems, and stroke, though the associations were somewhat less dramatic.
This staged pattern fits with what scientists understand about how syphilis operates. The bacterium targets tiny blood vessels that supply the walls of larger arteries, gradually causing inflammation and damage that worsens over time. Catching and treating the infection early, before this damage accumulates, appears to be the critical window.
Syphilis, HIV, and an Unanswered Question About Treatment
Because syphilis and HIV frequently occur together, the researchers conducted a separate analysis comparing 721 patients who had both infections against 719 patients with HIV alone. In this group, syphilis was not associated with a significantly increased risk of most heart and blood vessel outcomes. The one exception was death, which remained dramatically elevated (more than 11 times higher) among patients with both infections. Because this subgroup was relatively small, that estimate carries considerable uncertainty and should be interpreted with caution.
The researchers suggested that because HIV already raises cardiovascular risk on its own, separating out any additional effect from syphilis becomes difficult. Larger studies would be needed to clarify whether HIV meaningfully changes the cardiovascular toll of syphilis.
According to the authors, this is the first modern U.S. study of its kind to identify an independent link between syphilis and heart and blood vessel outcomes since the infamous Tuskegee Syphilis Study decades ago. It is also the first to examine syphilis as a risk factor for reduced blood flow to the limbs using matched controls. It’s a meaningful addition, since that condition is increasingly recognized as carrying the same long-term dangers as coronary artery disease.
What The Findings Mean for Patients and Doctors
Given the sustained resurgence of syphilis across the country, the researchers suggest that routine heart health screening (checks of blood pressure, cholesterol, and blood flow to the legs) should be considered as part of standard syphilis care. Patients with a history of syphilis, particularly late-stage or untreated infection, may benefit from more aggressive management of traditional heart risk factors. On the other side, doctors evaluating patients with unexplained blood vessel disease, particularly aortic problems, might consider testing for syphilis.
Major questions remain. Because the study relied on medical billing codes and could not access laboratory data or treatment records, it was impossible to distinguish patients with active infections from those who had been treated, and some diagnoses may have been miscoded. Other unmeasured factors, including smoking status and race, could also have influenced the results. Whether prompt antibiotic therapy can prevent long-term heart and blood vessel damage is still unknown.
Syphilis, an infection many assumed modern medicine had nearly vanquished, deserves renewed attention not just as a sexual health concern but as a potential threat to the entire cardiovascular system. With cases still climbing, the urgency to understand that connection is only growing.
Disclaimer: This article is based on a retrospective observational study and reports associations, not proven causes. Syphilis was linked to higher rates of cardiovascular events, but the study design cannot confirm that the infection directly caused those outcomes. Individual risk varies. Readers with questions about syphilis testing, treatment, or cardiovascular health should consult a qualified medical provider.
Paper Notes
Limitations
This study carries several limitations tied to its backward-looking design. Because it relied on medical billing codes to identify syphilis diagnoses and cardiovascular events, there is potential for error in both directions: some syphilis cases may have been miscoded by stage, and some control patients may have had undiagnosed or previously treated syphilis not captured in their records. A large proportion of syphilis patients were classified under an unspecified stage, reflecting gaps in documentation. Smoking status and race and ethnicity could not be accounted for, variables that may be unevenly distributed between groups and could influence outcomes. Laboratory test results and treatment records were unavailable, meaning researchers could not determine whether patients had active or treated infections, nor could they evaluate whether treatment prevented cardiovascular problems. Events occurring outside the health system were not captured. Cause and effect cannot be confirmed from this type of observational study. The mortality finding, while plausible, may be influenced by unmeasured differences between groups and should not be interpreted as death caused solely by syphilis.
Funding and Disclosures
Dr. Nassir F. Marrouche reported receiving grant support from Abbott Laboratories, Biosense Webster, and Siemens AG, and personal fees from Medtronic plc, Boston Scientific Corporation, and Preventice Inc, and holding equity in Cardiac Design Labs outside the submitted work. Dr. Amitabh C. Pandey reported serving on an advisory board for Novartis AG outside the submitted work. No other disclosures were reported.
Publication Details
The study, titled “Adverse Cardiovascular Outcomes in Patients With Syphilis,” was authored by Eli Tsakiris, Han Feng, Ghassan Bidaoui, Christian Massad, Janice Zha, Zhihao Wu, Yishi Jia, Yingshuo Liu, Hadi Younes, Yara Menassa, Michel Abou Khalil, Mayana Bsoul, Mohammad Montaser Atasi, Samer Zakhour, David Mushatt, Omar Kreidieh, Nassir F. Marrouche, and Amitabh C. Pandey. Affiliations include Tulane Research Innovation for Arrhythmia Discovery, the Section of Cardiology at the Heart and Vascular Institute, the Section of Infectious Diseases at Tulane University School of Medicine, and the Department of Medicine at the Southeast Louisiana Veterans Health Care System, all in New Orleans, Louisiana. The paper was published in JAMA Network Open on April 13, 2026 (Volume 9, Issue 4, e266771). DOI: 10.1001/jamanetworkopen.2026.6771. The study was approved by the Tulane Institutional Review Board and is distributed under the terms of the CC-BY License.







