
Curated Lifestyle For Unsplash+
In A Nutshell
- Older adults with low sit-to-stand power were significantly more likely to die from any cause during the study’s follow-up period compared to those with normal power levels, with women facing roughly twice the risk and men facing about 57% higher risk.
- Women with low power scores were more than three times as likely to have reported a hip fracture in the previous year, while men with low scores were more likely to have a recent history of falls or fractures across all bone types.
- Low sit-to-stand power was linked to longer hospital stays for both men and women, and raised the risk of future hospitalization in women by 29%.
- A free smartphone app can help clinicians calculate a patient’s sit-to-stand power score and compare it against validated thresholds, requiring only a standard chair and a timer.
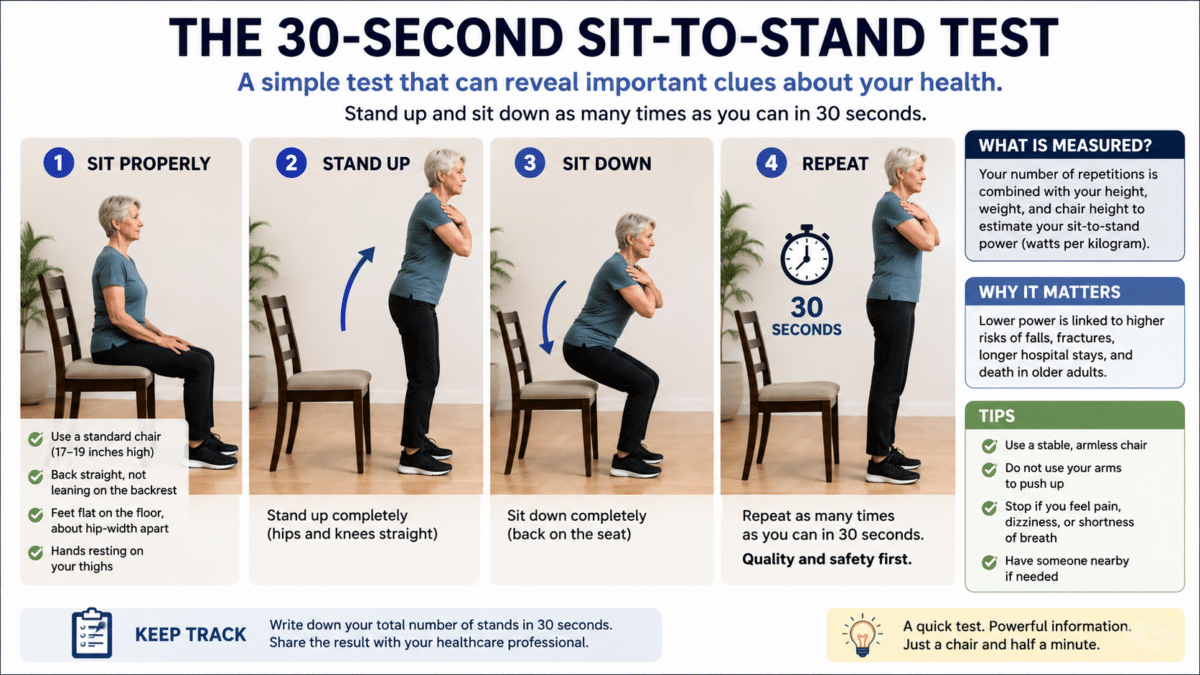
Getting up from a chair may be one of the most basic things a person can do, but how quickly and repeatedly someone can rise from a seat may offer clues about how long and how well they’ll live. New research finds that older adults who score poorly on a simple sit-to-stand test face higher risks of serious outcomes, including falls, broken bones, repeated hospitalizations, and death.
A large study following nearly 1,900 older adults found that those with low “sit-to-stand power” were significantly more likely to die from any cause during the follow-up period compared to those with normal levels. Women with low scores were roughly twice as likely to die, while men faced about a 57% higher risk. For a test requiring nothing more than a chair and a stopwatch, those are sobering numbers.
Published in the Journal of Sport and Health Science, the research comes from the Toledo Study for Healthy Aging, a long-running project based in Spain. Researchers tracked 1,876 adults aged 65 and older (about 56% of them women) measuring their physical power using a 30-second sit-to-stand test. Participants stood up and sat back down as many times as possible in half a minute. A formula then converted those repetitions, along with each person’s height, body weight, and chair height, into a power score measured in watts per kilogram of body weight.
What the Sit-to-Stand Chair Test Actually Measures
Muscle power is not the same as muscle strength. Strength is about peak force, how hard a muscle can push. Power adds speed to the equation: it’s the combination of force and how quickly that force is produced. Consider the difference between slowly pushing open a heavy door versus slamming it shut in one sharp motion. As people age, power tends to fade faster than strength does, and that decline speeds up after age 65.
Researchers used previously established cutoff scores to sort participants into two groups: those with low sit-to-stand power and those with normal levels. For men, the threshold was 2.53 watts per kilogram of body weight; for women, it was 2.01 watts per kilogram. More than half of the study participants, about 57%, fell below those thresholds.
That’s not a small fraction of the population. Low muscle power affects more than 45% of adults aged 65 and older, making it considerably more common than age-related muscle loss, which affects an estimated 10% to 16% of older adults.
Falls, Fractures, and a Clear Gender Divide
One of the more eye-opening findings was how differently low power was linked to broken bones in men versus women. For women, the danger was concentrated in hip fractures, one of the most serious and life-altering injuries an older person can sustain. Women with low sit-to-stand power were 3.25 times more likely to have reported a hip fracture in the previous year compared to women with normal power levels. Among women with low power, 4.5% had suffered a hip fracture in the past year, versus just 1% of those with normal power.
For men, the pattern was different. Low power was linked to a recent history of falls in general and fractures across all parts of the body, rather than hip fractures specifically. Men with low power were 73% more likely to have reported a fall in the previous year and 86% more likely to have reported any type of fracture.
Researchers suggest these differences may reflect distinct physical and biological vulnerabilities between the sexes. After menopause, women lose bone density faster due to hormonal shifts, making the hip region especially fragile after a fall. In men, fractures appear to be more spread out across different parts of the body rather than concentrated in one area.
How Sit-to-Stand Power Predicts Hospital Stays and Survival
Beyond broken bones, the study tracked hospitalizations over a follow-up period averaging about 6.8 years, and deaths over a longer period averaging about 9.7 years. Lower sit-to-stand power was associated with more time in the hospital and a higher likelihood of dying during the follow-up window.
Both men and women with low power scores were hospitalized more often and stayed longer when admitted. Among men with low power, the average hospital stay was about 4 days per admission, compared to about 2.5 days for those with normal power. For women, the difference was 2.7 days versus 1.9 days.
When it came to the risk of being hospitalized in the first place, results split along gender lines again. Women with low sit-to-stand power were 29% more likely to be hospitalized during the follow-up period than women with normal power. For men, the difference existed but was not statistically significant after accounting for age, education, and other health conditions. The authors suggest sex differences in health-seeking behavior, care patterns, and physical reserve may help explain the gap, but the study was not designed to prove why it exists.
Why a Chair and a Stopwatch Belong in the Clinic
A 30-second sit-to-stand test doesn’t require expensive lab equipment, trained specialists, or a hospital setting. It needs a standard chair, a timer, and about half a minute of a patient’s time. Other methods of measuring muscle power in older adults, including stair-climbing tests, jump tests, and specialized gym equipment, require controlled conditions and physical abilities that many older adults simply don’t have. A sit-to-stand test sidesteps most of those barriers.
Researchers also addressed a methodological problem that has made it difficult to compare findings across different studies. Rather than identifying the lowest-performing portion of a given study’s participants, a group that can shift depending on who’s included, they used fixed, sex-specific cutoff scores. That approach makes it easier to apply results consistently across different patient populations and clinical settings. The authors also note that a free smartphone app, the Powerfrail App, can help clinicians estimate a patient’s relative muscle power score and compare it against validated sex-specific thresholds.
Getting out of a chair is something millions of older adults do dozens of times a day without a second thought. For clinicians looking for a fast, inexpensive, and meaningful way to identify who might be heading toward a fall, a hospital bed, or worse, timing how powerfully someone stands up could be one of the most useful tools not yet in routine use.
Disclaimer: This article is based on observational research and reports associations, not proven cause-and-effect relationships. Findings come from a study of older adults in Spain and may not apply equally to all populations. Consult a qualified healthcare provider before making any changes to exercise routines or medical care based on this information.
Paper Notes
Limitations
Muscle power was estimated using the 30-second sit-to-stand test rather than a laboratory gold standard, though the authors note the test has been validated across older adult populations and shows minimal bias compared to more technical methods. Falls and fractures were assessed by asking participants to recall events from the previous year, which introduces the possibility of memory errors and means the study cannot establish a direct cause-and-effect relationship between low power and those outcomes. Participants were drawn from an older Spanish population, which may limit how broadly the results apply to other countries or demographic groups. Future studies using prospective designs are needed to better clarify the direction and mechanisms behind the relationship between low sit-to-stand power, falls, and fractures.
Funding and Disclosures
Research was supported by the Centro de Investigación Biomédica en Red Fragilidad y Envejecimiento Saludable (CIBERFES) under grant numbers CB16/10/00477, CB16/10/00456, and CB16/10/00464. Additional funding came from the Plan Propio de Investigación of the University of Castilla-La Mancha, the Fondo Europeo de Desarrollo Regional (FEDER) funds from the European Union (grant number 2022-GRIN-34296), the Instituto de Salud Carlos III (grant numbers PI031558, PI07/90637, PI07/90306, RD 06/0013, and PI18/00972), the Government of Castilla-La Mancha (grant numbers 03031 and SBPLY/19/180501/000312), and Red EXERNET (RED2022-134800-T) from the Spanish Ministry of Innovation and Science. One author received a research grant from the University of Castilla-La Mancha under the Programa Investigo (grant number 2024-INVGO-12359). No competing interests were declared.
Publication Details
Authors: Mikel Garcia-Aguirre, Ivan Baltasar-Fernandez, Julian Alcazar, Ana Alfaro-Acha, Fabio A. Quiñonez-Bareiro, Ignacio Ara, Leocadio Rodriguez-Mañas, Francisco J. Garcia-Garcia, and Luis M. Alegre | Affiliations: GENUD Toledo Research Group, Faculty of Sport Sciences, University of Castilla-La Mancha; Centro de Investigación Biomédica en Red Fragilidad y Envejecimiento Saludable (CIBERFES), Instituto de Salud Carlos III; Instituto de Investigación Sanitaria de Castilla-La Mancha (IDISCAM); Geriatrics Department, Hospital Universitario de Toledo; Geriatrics Department, Getafe University Hospital; Faculty of Health Sciences, University of Castilla-La Mancha | Journal: Journal of Sport and Health Science | Paper Title: Low relative sit-to-stand power is associated with history of falls and fractures, prospective hospitalization, and all-cause mortality in older adults from the Toledo study for healthy aging | DOI: 10.1016/j.jshs.2025.101080 | Published: Available online August 13, 2025; Volume 15, article 101080 (2026 issue)







