
Kratom is mainstream and its risks are growing. CDC data show 2025 poison center reports hit a record, up 1,200% in 10 years. (Credit: Andrii__Ivaniuk on Shutterstock)
Is Kratom Safe? New Data on 9,000 Poisonings Suggests Lawmakers Need to Take a Harder Look
In A Nutshell
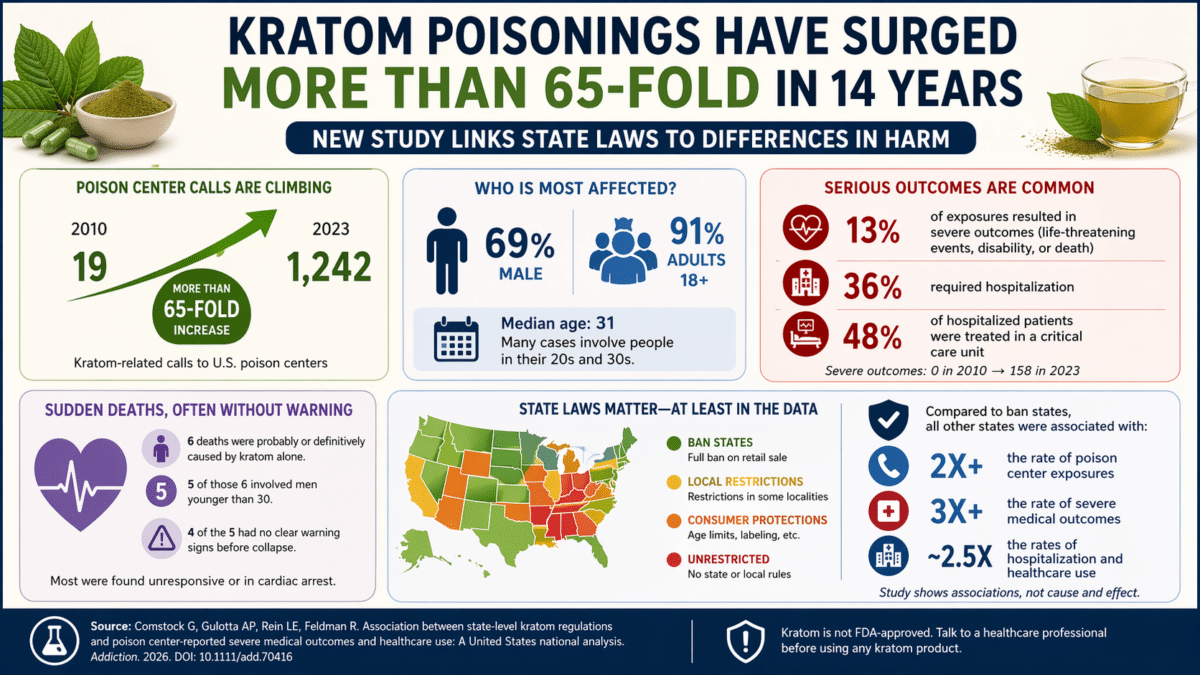
- Kratom-related poison center calls surged more than 65-fold between 2010 and 2023, with 13% of reported exposures resulting in life-threatening outcomes, permanent disability, or death.
- Adult men in their 20s and 30s account for the majority of cases, and five of six single-substance kratom deaths reviewed in detail involved men younger than 30.
- States with outright bans on kratom sales were associated with more than three times fewer severe medical outcomes than states with no restrictions or consumer protection laws only.
- Consumer protection measures such as age limits and labeling requirements showed no statistically significant improvement over having no kratom regulations at all.
Fourteen years ago, U.S. poison centers handled 19 kratom-related calls. Last year, they handled 1,242. That more than 65-fold climb tracks alongside a surge in Americans turning to the Southeast Asian plant as a self-treatment for pain, anxiety, and opioid withdrawal, often with little idea of what a serious exposure can actually look like.
Kratom is sold in gas stations, smoke shops, and online stores across most of the country, typically as a powder, capsule, or tea. At low doses it works like a stimulant. At higher doses it mimics opioids. Federal law doesn’t regulate it, leaving rules, or the absence of them, entirely up to individual states. Advocates call it a useful harm-reduction tool. The poison center data tells a more complicated story.
Researchers at the Medical College of Wisconsin spent 13 years tracking those calls nationally, and their findings, published in the journal Addiction, suggest that the type of kratom regulation a state adopts is closely linked to differences in how harmful those outcomes turn out to be.
A Kratom Poisoning Surge That Shows No Sign of Slowing
From 2010 to 2023, poison centers across all 50 states and Washington, D.C. logged 8,919 kratom-related exposures. Adult men dominated the data, with 69% of exposures occurring in males and 91% in adults 18 or older. Many cases involved people in their 20s and 30s, with a median age of 31. Severe medical outcomes, defined as life-threatening events, permanent disability, or death, climbed from zero cases in 2010 to 158 in 2023. Overall, 13 out of every 100 kratom exposures reported to a poison center resulted in one of those severe outcomes. More than a third of all cases required hospitalization, and nearly half of those patients ended up in a critical care unit.
Those numbers raise serious questions about how safe kratom is often perceived to be. It can cause liver damage, dangerous heart rhythms, and seizures. It also interacts with the enzymes the body uses to process other drugs, which may help explain the higher severe outcome rate seen in cases where kratom was combined with other substances, 13%, compared to 8.7% when kratom was the only drug involved.
Young Men Dying Suddenly, Often Without Clear Warning
Among all single-substance kratom exposures in the study, 27 deaths were reported. Researchers also examined a subset of those cases in detail, identifying six deaths judged as probably or definitively caused by kratom alone. Five of those six involved men younger than 30.
Most were found unresponsive or in cardiac arrest, with a documented history of kratom use and no clear warning signs reported beforehand. Four of the five showed no symptoms in the hours leading up to collapse. One man suffered a seizure during intercourse before going into cardiac arrest. A woman in her 50s became unresponsive after ingesting kratom, inhaled fluid into her lungs, developed a severe infection, and died three days later.
Based on this small but detailed set of cases, the pattern is sobering: a substance sold openly, often marketed as natural and safe, associated with sudden cardiac events in otherwise young, adult men. The authors noted that the six reviewed narratives represent only the cases where kratom was judged the probable or definitive cause, and that the full single-substance death toll in the dataset was 27.
How State Kratom Laws Are Linked to Who Ends Up in the Hospital
As lawmakers across the country debate how to handle kratom, a central question has been whether consumer protection measures, things like age restrictions and labeling requirements, are enough to reduce harm without resorting to an outright ban. Based on this study’s associations, the answer appears to be no.
Researchers sorted states into four categories: completely unrestricted, local restrictions only, consumer protection laws, or full bans on retail sale. States with bans reported lower rates across every outcome measured. Compared to ban states, all others combined were associated with more than twice the rate of poison center exposures, more than three times the rate of severe medical outcomes, and roughly 2.5 times the rates of hospitalization and overall healthcare use. Consumer protection laws, often promoted by kratom advocacy groups as the responsible middle ground, were linked to outcomes statistically indistinguishable from states with no rules at all in this dataset.
Kratom is widely available at retail in states without bans regardless of what consumer protections are technically on the books, the researchers noted. Bans may reduce harm partly by removing kratom from store shelves and limiting the advertising that drives awareness and access, though the study cannot establish that directly.
This is observational research, and the authors were careful to frame their findings as associations rather than proof of cause and effect. Under-reporting in ban states, where users may hesitate to call poison control out of fear of legal consequences, could also be affecting the comparison. Those are real limitations. But the association held across every outcome and every year of the 14-year dataset.
What makes the stakes particularly sharp is that the legislative tide is moving away from bans. Since 2023, several states have moved toward or passed consumer protection frameworks, including Florida, Maryland, Nebraska, and South Carolina. For adult men in their 20s and 30s who use kratom regularly, the question of what replaces a ban, and whether it offers any meaningful protection, is one the data has not yet answered reassuringly.
Disclaimer: This article is based on an observational study and does not establish that kratom directly causes the outcomes described. Findings reflect associations reported in peer-reviewed research and should not be interpreted as medical advice. Anyone with questions about kratom use or its health effects should consult a qualified healthcare provider.
Paper Notes
Limitations
This was a retrospective observational study, meaning it can identify associations but cannot establish causation. Because polysubstance exposures were included, adverse outcomes may not be attributable solely to kratom. Kratom Consumer Protection Acts were assessed as a group, so individual components may have had effects masked by bundling with less effective measures. Classifying each state’s regulatory status was difficult due to varying statutory language and evolving local rules, and some degree of misclassification cannot be ruled out. The District of Columbia was particularly hard to categorize due to conflicting legal interpretations. Poison center data relies on passive reporting and caller-provided information that cannot be independently verified. Laboratory confirmation of kratom exposure in clinical practice is rare, so most cases rest on patient self-report. Records are encounter-based rather than patient-based, meaning individuals may contribute more than one exposure to the dataset. Under-reporting may be worse in ban states if users fear legal consequences for seeking help.
Funding and Disclosures
No funding was provided for this research. The authors declared no conflicts of interest.
Publication Details
The study was authored by Grant Comstock, Anthony P. Gulotta, Lisa E. Rein, and Ryan Feldman, all affiliated with the Medical College of Wisconsin. Gulotta is also affiliated with Walter Reed National Military Medical Center. The paper, titled “Association between state-level kratom regulations and poison center-reported severe medical outcomes and healthcare use: A United States national analysis,” was published in the journal Addiction in 2026. DOI: 10.1111/add.70416







