
Credit: Sarkadi Roland on Shutterstock
The inexpensive setup could help save countless lives during radiation emergencies
In A Nutshell
- Researchers tested a cheap setup that uses a smartphone and color-changing film to quickly flag very high radiation exposure.
- It worked best for serious exposures (about 5 Gy or higher), which is the range where people may need urgent medical care.
- It did not reliably measure lower doses, so a “low reading” should never be treated as an all-clear.
- The big win is speed: it could help responders sort people faster when hospitals and labs are overwhelmed.
When a nuclear accident or terrorist attack affects thousands of people, medical teams face an impossible question: who was exposed to life-threatening radiation doses and who can safely go home? Researchers at Hiroshima University think they’ve found a solution to this crisis response hurdle using technology most people already carry in their pockets.
Scientists Hassna Bantan and Hiroshi Yasuda tested whether everyday phones like Samsung Galaxies and iPhones could help flag likely high radiation exposure by photographing specialized film through a portable scanner. It’s not a lifesaver by itself, but it could help responders focus care where it’s most urgently needed. In a radiological emergency, this kind of rapid sorting matters because exposure to 3-4 Gy of radiation can kill within 60 days without treatment, and knowing who needs urgent care versus who received lower doses can save lives when hospitals are overwhelmed.
Current emergency dosimetry requires expensive laboratory equipment and trained technicians, creating bottlenecks when hundreds or thousands need rapid assessment. Bantan and Yasuda’s system costs under $70 for the portable scanner, and each film piece costs roughly $2. That’s affordable enough for governments to pre-distribute to nuclear facility workers, first responders, and residents near power plants. Scanners could be stored in emergency shelters the way they stock flashlights and first-aid kits.
How Color-Changing Film Detects Radiation
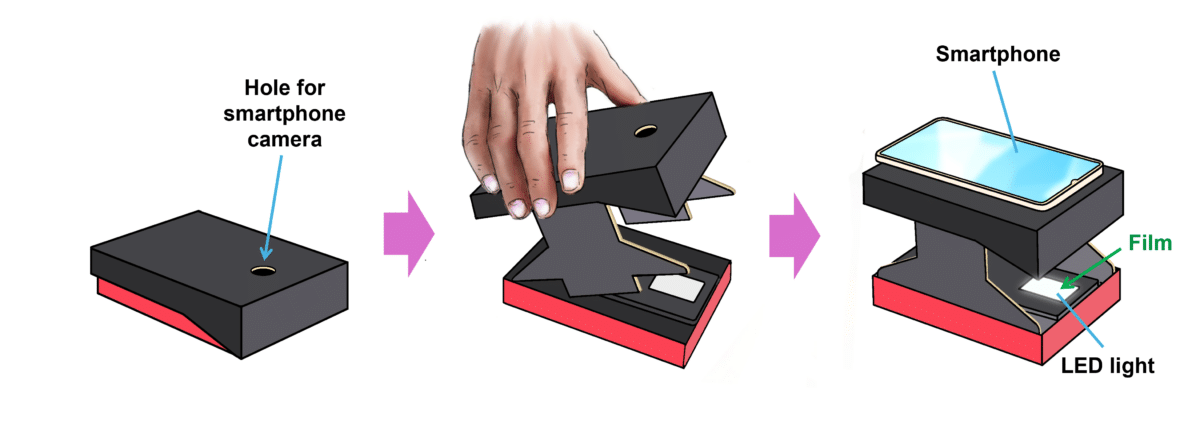
Gafchromic EBT4 film contains a radiation-sensitive material that turns progressively darker blue when exposed to ionizing radiation. The film develops color immediately without any chemical processing. Someone exposed to radiation during an emergency could pull out their pre-distributed film piece, scan it using a portable LED light box called a PictoScanner (originally designed for digitizing old photo negatives), and photograph it with their smartphone camera.
Bantan and Yasuda cut the specialized film into small rectangular pieces measuring approximately 24mm by 36mm: slightly larger than a postage stamp. They exposed these pieces to X-rays at three different dose levels: 2.5 Gray (Gy), 5.0 Gy, and 10 Gy. Whole-body exposure to less than 1 Gy can cause blood cell production problems, while 3-4 Gy means a 50% chance of death within two months without medical intervention.
The researchers scanned each piece using four different smartphones: two Samsung models (Galaxy A23 5G and Galaxy Note8) and two iPhones (Xs Max and 13 Pro Max). The PictoScanner held the film above an LED light table, allowing the smartphone camera positioned about 8 centimeters above to capture transmitted light through the color-changed film. This setup eliminated problems with surface reflections and ambient lighting.
Why the Phone Method Works Only for High Doses
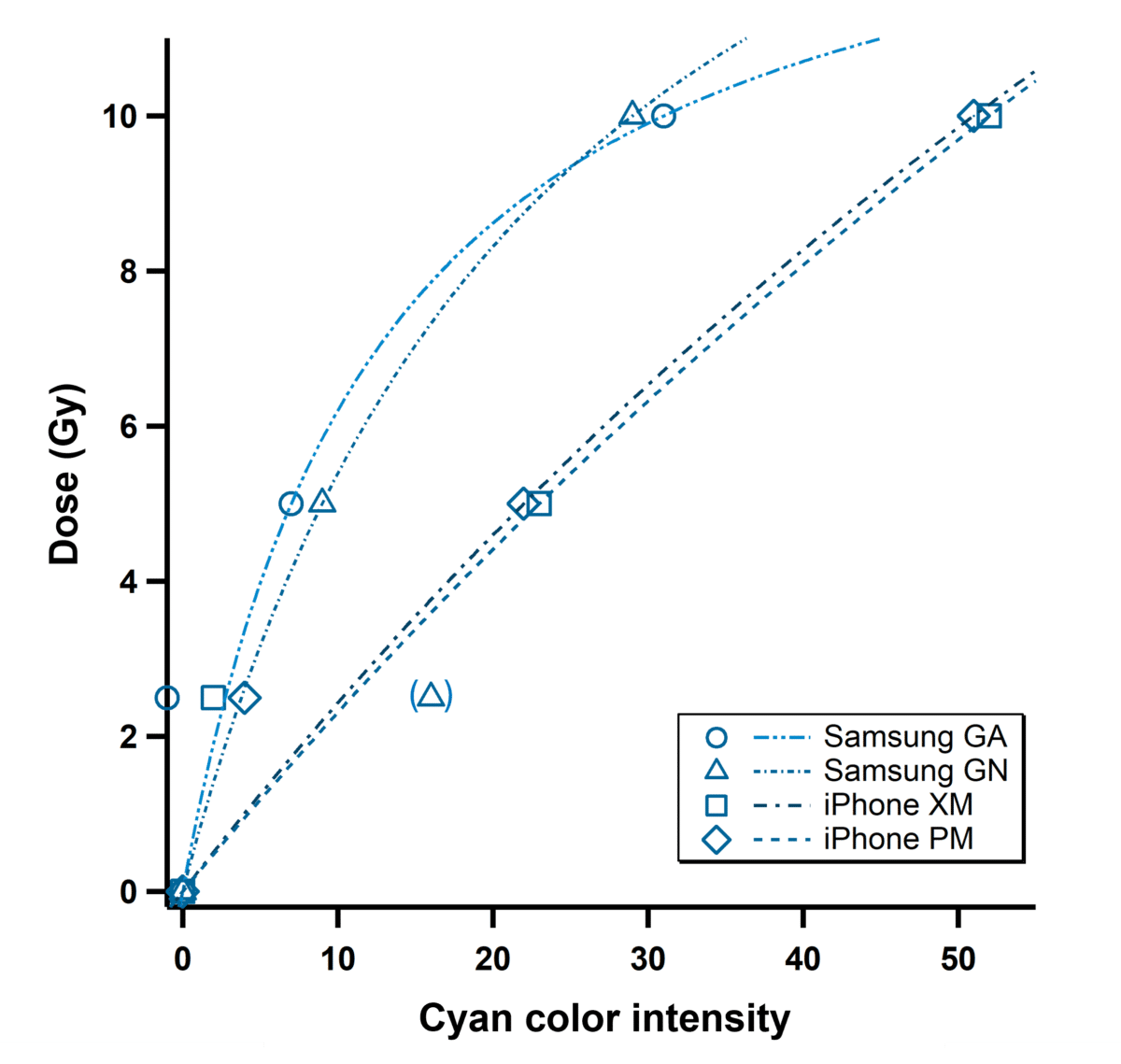
The phones performed remarkably well at 5 Gy and 10 Gy doses, considered the danger zone where people need immediate medical attention. However, at 2.5 Gy, all four smartphones stumbled badly. Samsung Galaxy Note8 overestimated the dose by 193%, while other phones underestimated doses by 60-100%. If the film doesn’t darken much, the phone can’t reliably tell the difference between “some exposure” and “more exposure.”
“According to the findings, this inexpensive portable dosimetry tool is expected to be effectively applied for on-site emergency dosimetry in relatively high-dose (≥5 Gy) situations,” the researchers wrote. That limitation matters because many harmful effects begin below 5 Gy. Recent studies suggest threshold doses as low as 0.5 Gy for lens opacities and circulatory problems.
In practice, the system works like a smoke alarm: not a full diagnosis, but a loud warning that tells you to seek help fast. Someone exposed to 1-4 Gy might not trigger enough color change for reliable phone detection, yet could still face serious health consequences including increased cancer risk and fertility problems.
Some cameras read the film more consistently than others. Samsung Galaxy A23 5G delivered the most reliable results, with less than 1% variation when scanning the same film multiple times. iPhone 13 Pro Max showed the most linear relationship between dose and color change. But each phone model needs its own settings because different cameras have different color sensitivities and processing.
Getting Ready Before Disaster Strikes
The approach, detailed in Radiation Measurements, requires advance preparation. Local governments or facility operators would need to distribute small film pieces to people who might face radiation exposure risks: nuclear power plant workers, emergency responders, medical personnel, and potentially residents living near facilities. The researchers stored their film samples at 15°C in a dark refrigerator before testing, though once the film has been exposed to radiation, the developed color remains stable under normal indoor conditions.
Organizations would also need to stockpile portable scanners. The PictoScanner weighs less than 300 grams and runs on two AA batteries. Multiple people could share a single scanner at emergency shelters, medical triage points, or community centers, with each person photographing their own film piece.
For best accuracy, the phone needs to take an unfiltered photo (using a setting called RAW mode), and a free app like ImageJ.JS can read the film using saved settings for that phone model. Emergency conditions add another layer of uncertainty. For example, temperature swings, humidity, and variable lighting could all affect both the film and camera performance. The researchers ran their tests in controlled conditions at 20-23°C, but real disasters don’t offer that luxury.
Why This Matters for Emergency Response
Current emergency dosimetry can take hours or days to process samples from thousands of people, delaying critical treatment decisions. The ability to quickly flag whether someone’s exposure was in the danger zone gives medical responders a way to prioritize care. Anyone whose film shows 5 Gy or higher needs urgent medical attention. Those below detection limits can be monitored less intensively.
That triage function alone could prevent hospital overcrowding and direct limited medical resources to those who need them most. Previous attempts at portable film dosimetry used specialized equipment costing over $500 per device. Earlier Hiroshima University studies tested portable colorimeters that measured down to 1 Gy, but those devices still cost considerably more than a phone most people already own.
Bantan and Yasuda emphasize their method can’t replace professional dosimetry. Smartphone measurements serve as preliminary screening, with follow-up biological tests like chromosome analysis providing definitive dose assessment for treatment planning. Still, in the critical first hours after a radiological emergency, getting a quick read on who likely needs immediate care beats waiting for precise measurements.
The researchers are now working to test the system under realistic field conditions and investigating whether other radiochromic film types with different sensitivities could fill in the gaps, providing coverage across a broader dose range.
Disclaimer: This article is for general information only. In any suspected radiation exposure event, follow official emergency guidance and seek medical care when directed.
Paper Notes
Study Limitations
The system showed poor accuracy at 2.5 Gy, with dose estimation errors ranging from 60% underestimation to 193% overestimation depending on the smartphone model. This restricts reliable measurements to doses of 5 Gy and above, which exceeds the threshold for many radiation health effects. The study tested only four smartphone models under controlled laboratory conditions with consistent temperature (20-23°C) and lighting. Real-world emergency conditions involving variable ambient light, temperature extremes, user stress, and film handling variations were not evaluated. Different smartphone models require device-specific calibration settings, and the researchers did not assess how consistently cameras perform within the same model line or across software updates. Long-term stability of film images stored on smartphones remains unknown. The analysis focused on a narrow time window, and effects of post-exposure delays between irradiation and scanning were not thoroughly characterized. The portable scanner’s LED light source characteristics and potential variability across individual scanner units were not quantified. Software-based image processing, including in-phone compression and automatic white-balance corrections, was not evaluated in depth despite potentially affecting dose assessment accuracy.
Funding and Disclosures
This research received administrative support and article publishing charges from Hiroshima University. Hassna Bantan is affiliated with the Phoenix Leader Education Program (Hiroshima Initiative) for Renaissance from Radiation Disaster at Hiroshima University, in addition to her positions in the Department of Radiation Biophysics and Graduate School of Biomedical and Health Sciences. The authors declared no competing financial interests or personal relationships that could have influenced the reported work. Mr. Soheil Aghabaklooei from Graduate School of Biomedical and Health Sciences and Mr. Hideaki Fujita, Associate Professor at Hiroshima University, provided smartphones for the experiments.
Publication Details
Authors: Hassna Bantan and Hiroshi Yasuda | Affiliation: Department of Radiation Biophysics, Research Institute for Radiation Biology and Medicine (RIRBM), Hiroshima University, Kasumi 1-2-3, Minami-ku, Hiroshima, 734-8553, Japan | Journal: Radiation Measurements, Volume 191, 2026| Article Number: 107593 | DOI: 10.1016/j.radmeas.2025.107593 | Submission Timeline: Received August 23, 2025; Revised November 10, 2025; Accepted December 12, 2025; Available online December 13, 2025| License: Published by Elsevier Ltd. under CC BY-NC license (http://creativecommons.org/licenses/by-nc/4.0/) | Corresponding Author: Hiroshi Yasuda ([email protected]) | Special Issue: This article is part of a special issue entitled SSD21 published in Radiation Measurements.







