
(© kai - stock.adobe.com)
Study Shows It’s Not About Your Weight, It’s About Where The Fat Lives
In a Nutshell
- A large study found that people who reduced and sustained lower levels of deep belly fat showed measurably slower brain shrinkage and better memory and thinking scores years later.
- Carrying the APOE gene variant, the strongest known genetic risk factor for Alzheimer’s disease, did not change the relationship between visceral fat and brain shrinkage, suggesting the effect operates independently of inherited Alzheimer’s risk.
- General weight loss, measured by BMI, did not show the same brain-protective pattern. It was specifically visceral fat, the kind packed around internal organs, that drove the association with brain health.
A spare tire around the midsection is more than a cosmetic concern. Research suggests that a specific type of fat buried deep in the abdomen may be quietly speeding up brain shrinkage and mental decline in middle age, and that getting rid of it could slow the damage for years, even a decade later.
A large, long-running follow-up study tracked more than 500 adults for up to 16 years. People who lost and kept off visceral fat — the deep belly fat packed around internal organs — showed slower brain shrinkage and better scores on thinking and memory tests well into their early sixties. General weight loss, as measured by body mass index or BMI, didn’t show the same brain-protective pattern. It was specifically the deep abdominal fat that mattered.
That distinction could reshape how doctors and public health officials think about obesity and dementia risk. While the link between being overweight and mental decline has been studied for years, this research singles out one particular fat deposit as uniquely harmful, and as a target that lifestyle changes can actually shrink.
It’s important to note that this research was published as an advance, unedited manuscript in Nature Communications to allow early access to its findings. The paper has not yet undergone final editorial review, and the authors note that errors may be present.

Tracking Belly Fat and Brain Scans Across 16 Years
Called the Follow-up Intervention Trials (FIT) project, the research brought together participants from four prior clinical trials conducted between 2005 and 2018 in Israel. Those original trials had tested various lifestyle changes, including different diets and exercise programs, over 18 to 24 months. For the FIT project, the researchers tracked down 647 of the original 881 eligible participants years later, collecting new brain scans, abdominal fat measurements, and cognitive test scores between 5 and 16 years after the original programs ended.
Of those, 533 adults completed brain MRI scans at the follow-up visit. The group was 86 percent male, with an average age of about 61. Participants had started the original trials at an average age of 52, with an average BMI of about 30, placing most in the overweight-to-obese range. Many had excess belly fat, abnormal cholesterol levels, or Type 2 diabetes. The heavily male sample is an important caveat: the findings may not fully apply to women, who tend to store and metabolize fat differently.
Using MRI machines, researchers measured both abdominal fat and brain structure. For abdominal fat, they distinguished between three types: visceral fat (the deep, organ-hugging kind) and two layers of fat sitting just beneath the skin. For the brain, they measured total brain volume, gray matter, white matter, the fluid-filled spaces inside the brain called ventricles, and how much room the hippocampus, a region central to memory, occupied.
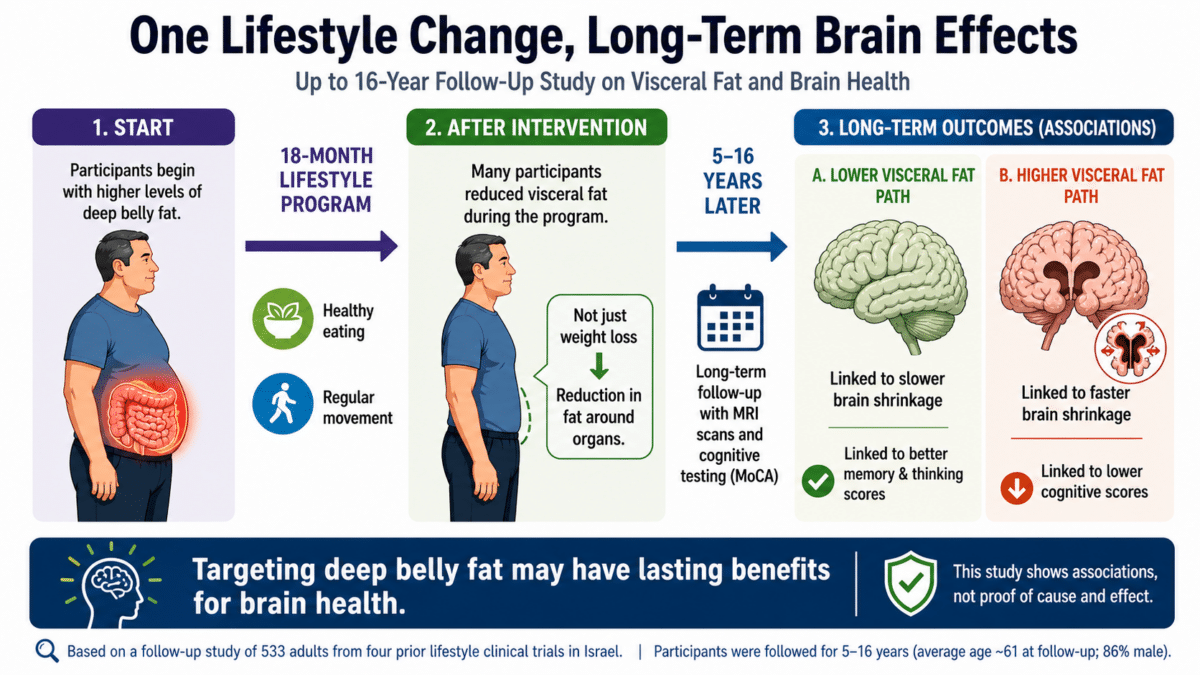
Visceral Fat Was the Only Kind Tied to Brain Shrinkage
At the follow-up visit, people with more visceral fat scored lower on the Montreal Cognitive Assessment, or MoCA, a widely used screening test for thinking and memory problems. The average score suggested mild cognitive difficulties for the group, though the researchers noted this was consistent with the metabolic health profiles of the participants.
Neither type of fat sitting closer to the skin showed the same harmful associations. Only visceral fat stood out.
Researchers also looked at how much visceral fat a person had carried over the full span from their original trial through the follow-up. Among 295 participants with complete data across three time points, higher cumulative visceral fat exposure was tied to lower scores on both the MoCA and its memory-specific portion. Fat beneath the skin showed no such link, and neither did BMI.
Among 188 participants from one of the trials who had brain scans at three separate points, those who had accumulated more visceral fat showed faster rates of brain shrinkage across multiple measures. Their gray matter declined more quickly, their hippocampus shrank faster, and the ventricles in their brains expanded more rapidly — a classic signature of brain aging.
People who had lost visceral fat during the original lifestyle programs, meanwhile, showed meaningfully better brain preservation years later. A greater reduction in visceral fat during the 18-month program was associated with higher total brain volume and gray matter volume at follow-up. A reduction in the proportion of visceral fat relative to other abdominal fat was also linked to better hippocampal preservation. These relationships held up even after the researchers accounted for overall weight loss, age, sex, dietary habits at follow-up, and other potential confounding factors.
Because this was an observational follow-up rather than a controlled experiment, these associations cannot prove that losing visceral fat directly caused the brain benefits. But the consistency of the pattern across multiple measures and time points strengthens the case.
Changes in the fat beneath the skin during the original programs had no relationship to brain outcomes years later. And while BMI change during the programs was linked to later cognitive test scores, it was not linked to brain structure, hinting that BMI may influence thinking ability through different pathways that don’t show up on a brain scan.
The Blood Sugar Connection: Why Visceral Fat May Harm the Brain
To understand why visceral fat might harm the brain, the team examined a range of blood markers related to blood sugar control, cholesterol, and inflammation. After rigorous statistical testing, only two markers were tied to the rate of brain shrinkage over time: fasting blood sugar and HbA1c, a measure of average blood sugar over several months. Cholesterol and inflammation markers did not show consistent links.
This makes sense given what scientists already know about visceral fat. Unlike the fat one can pinch beneath the skin, visceral fat is metabolically active tissue that pumps out substances promoting insulin resistance, a condition in which the body’s cells stop responding properly to the hormone that regulates blood sugar. Over time, chronically elevated blood sugar can damage blood vessels throughout the body, including in the brain. The researchers noted that their results are consistent with a previous study from the same group showing that improvements in blood sugar control were associated with slower brain aging.
Among participants who had genetic data available, about 17 percent carried a variant of the APOE gene, the strongest known genetic risk factor for Alzheimer’s disease. But carrying that gene variant did not change the relationship between visceral fat and brain shrinkage. The visceral fat effect appeared to operate on its own, independent of genetic Alzheimer’s risk.
A Finding That Could Change How Doctors Think About Dementia Prevention
These results carry weight at a time when both obesity and dementia are surging globally. While the 2024 Lancet Commission on dementia prevention identifies obesity as a modifiable midlife risk factor, it does not separately call out visceral fat. This study makes a case that it should — that not all fat is created equal when it comes to the brain, and that the deep abdominal kind deserves special attention.
Fat accumulating around the organs of millions of middle-aged adults may be slowly eroding their brains. Lifestyle programs that specifically target visceral fat could offer lasting protection, not just for the waistline, but for the mind.
Disclaimer: The information presented is based on observational research and is intended for general education. It does not establish causality or replace professional medical guidance. The research was published as an advance, unedited manuscript in Nature Communications to allow early access to its findings. The paper has not yet undergone final editorial review, and the authors note that errors may be present. All legal disclaimers from the journal apply.
Paper Notes
Limitations
The study’s participants were predominantly male (86 percent) and started in the overweight-to-obese range, which may limit how broadly the findings apply to women and to people with lower body weight. While the initial fat loss occurred under the controlled conditions of randomized clinical trials, the long follow-up period of 5 to 16 years was observational, meaning participants were not randomly assigned to maintain specific behaviors after the trials ended. This limits the ability to draw firm cause-and-effect conclusions. Cognitive function was not systematically measured before or immediately after the original interventions, so individual-level cognitive changes over the full timeline could not be assessed. Baseline and end-of-intervention abdominal fat scans were only available from two of the four trials (CENTRAL and DIRECT-PLUS), and brain MRI scans at multiple time points were only available from the DIRECT-PLUS trial. The study also lacked Alzheimer’s disease biomarker data, such as PET imaging or blood-based markers, which would have helped determine whether the observed brain atrophy reflects Alzheimer’s-related processes specifically. The researchers also noted the absence of measurements of fat in organs like the liver and pancreas, which could be relevant. Dietary and lifestyle patterns at follow-up were assessed and adjusted for in the statistical models.
Funding and Disclosures
This work was supported by grants from the Deutsche Forschungsgemeinschaft (DFG, German Research Foundation) under Germany’s Excellence Strategy (Leipzig LeiCeM Cluster of Excellence), as well as ERA NET ERA4HEALTH, with funding directed to principal investigator Iris Shai and collaborating researchers including Michael Stumvoll, Matthias Blüher, and Veronica Witte. One co-author, Matthias Blüher, received honoraria for lectures and consultancy from Amgen, AstraZeneca, Bayer, Boehringer-Ingelheim, Lilly, Novartis, Novo Nordisk, and Sanofi. All other authors reported no conflicts of interest.
Publication Details
Title: Sustained visceral fat loss is associated with attenuated brain atrophy and improved cognitive function in late midlife
Authors: Dafna Pachter, Hadar Klein, Omer Kamer, Dana Tamar Goldberg Toren, Liav Alufer, Noa Ebstein Karamani, Tomer Atlas, Amit Yaary, Idan Hagbi, Yoash Chassidim, Ilan Shelef, Moti Salti, Frauke Beyer, Veronica Witte, Assaf Rudich, Uri Yoel, Gal Ben-Arie, Anat Yaskolka Meir, Alon Kaplan, Gal Tsaban, Hila Zelicha, Carmi Bartal, Lu Qi, Matthias Blüher, Michael Stumvoll, Uta Ceglarek, Berend Isermann, Dong D. Wang, Meir J. Stampfer, Frank B. Hu, Galia Avidan, and Iris Shai (corresponding author). Dafna Pachter and Hadar Klein contributed equally.
Journal: Nature Communications (Article in Press)
DOI: https://doi.org/10.1038/s41467-026-71141-4
Affiliated Institutions: Ben-Gurion University of the Negev (Israel); Soroka University Medical Center (Israel); Sapir Academic College (Israel); Max Planck Institute for Human Cognitive and Brain Sciences and University of Leipzig Medical Center (Germany); Helmholtz Institute for Metabolic, Obesity and Vascular Research (Germany); Harvard T.H. Chan School of Public Health (USA); Tulane University (USA); Reichman University (Israel); among others.
Clinical Trial Registrations: DIRECT (NCT00160108); CASCADE (NCT00784433); CENTRAL (NCT01530724); DIRECT-PLUS (NCT03020186).







