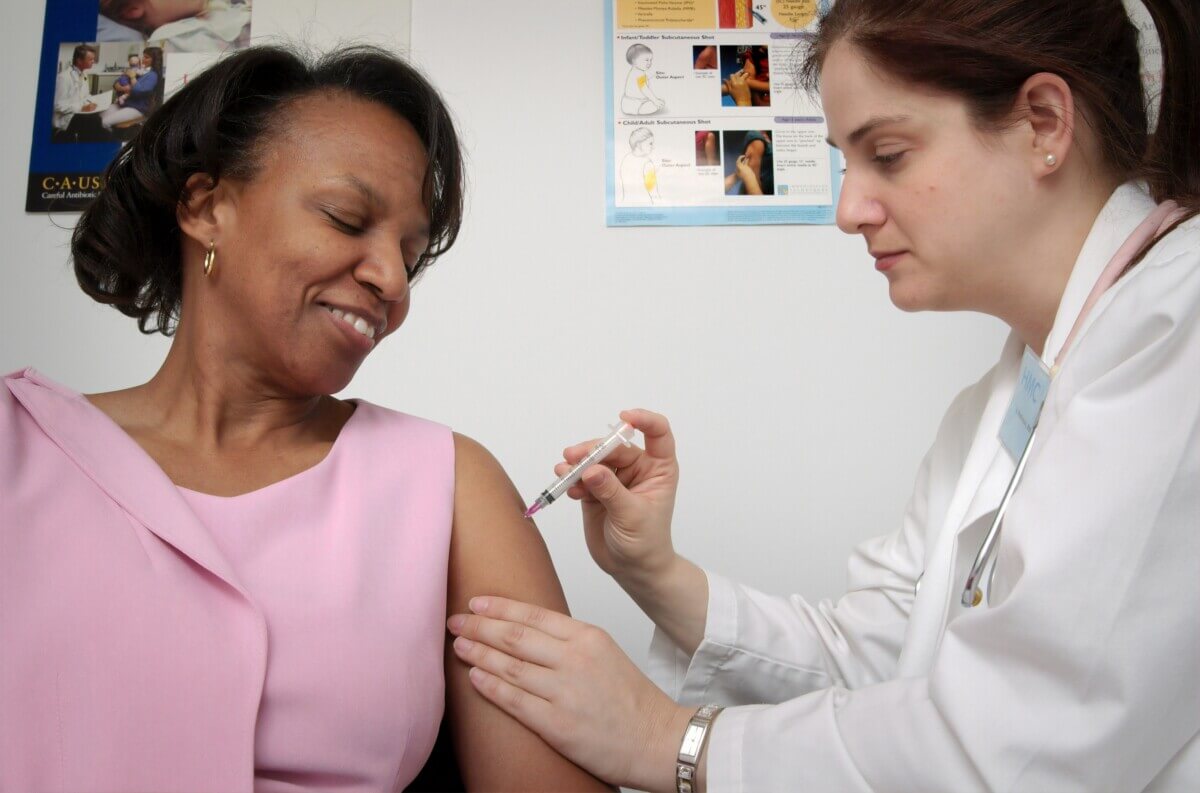
Photo by CDC on Unsplash
In A Nutshell
- Vaccinated adults over 70 showed cellular markers of slower aging compared to unvaccinated peers, including younger-looking DNA patterns and lower inflammation levels
- The anti-aging signals appeared strongest within three years of vaccination for molecular markers, while inflammation benefits emerged after four or more years
- Researchers can’t prove the vaccine caused these differences: healthier people may simply be more likely to get vaccinated in the first place
- The study examined the older Zostavax vaccine; whether the newer, more effective Shingrix produces similar effects remains unknown
Your birth certificate says one age. Your body might tell a different story. Scientists can now look at your cells and DNA to determine your “biological age,” which is essentially how old your body acts compared to how many birthdays you’ve had. Now, research suggests people who received the shingles vaccine show cellular signs of slower aging.
Researchers at the University of Southern California examined blood samples from nearly 4,000 Americans over age 70. Those who’d gotten the shingles shot showed markers of slower biological aging compared to people who skipped the vaccine. The difference remained even after accounting for factors like income, education, smoking history, and existing health problems.
Two people who are the same chronological age might show different rates of aging at the cellular level. The vaccinated group in this study, published in the Journal of Gerontology, leaned toward the slower-aging end of that spectrum, though the study can’t prove the vaccine caused this difference.
Your Cells Keep Their Own Calendar
Scientists have developed several ways to measure biological age using blood tests. Some look at chemical tags attached to your DNA that change predictably as you age. Others check which genes are turned on or off in your cells. Still others measure inflammation levels, since chronic inflammation speeds up aging.
The shingles vaccine appeared to improve several of these aging markers. Vaccinated people had less inflammation in their blood, healthier patterns on their DNA, and gene activity that looked younger than expected for their age.
The inflammation finding may be key. After you’ve had chickenpox, the virus that causes it never completely leaves your body. It hides in your nerve cells and can periodically wake up, sometimes causing shingles but other times just triggering low-level inflammation you’d never notice. This constant, subtle immune activation may contribute to aging.
One possible explanation for the findings is that by preventing the virus from reactivating, the vaccine might reduce this inflammatory burden. Less inflammation could mean slower aging at a cellular level. However, the study didn’t directly test this mechanism.
When the Benefits Show Up
The anti-aging associations followed an interesting timeline. People vaccinated within the past three years showed the strongest benefits in their DNA patterns and gene activity. Those vaccinated more than four years ago showed different benefits, mainly lower inflammation and better innate immune function.
This suggests the vaccine might affect different biological systems on different timescales, though more research would be needed to confirm this pattern.
Nearly half the people in the study (49.6%) had received the shingles vaccine. Those who had been vaccinated tended to be slightly more educated and had higher incomes than those who didn’t. This makes sense, since people with better access to healthcare are more likely to get preventive shots.
The researchers accounted for these differences statistically, but there’s always the possibility that people who choose to get vaccinated also make other healthy choices that weren’t measured.
The Confusing Immune Results
Not everything pointed in a positive direction. One part of the immune system (the adaptive immune response that learns to recognize specific threats) looked different in vaccinated people based on blood cell counts, in a way that might suggest older immune function.
This puzzled the researchers. Vaccines work by training this exact part of the immune system, so seeing it look worse seems contradictory. One possibility is that the blood tests being used can’t tell the difference between a well-trained immune system (which has lots of memory cells from past exposures) and an exhausted one (which also has lots of memory cells but doesn’t work as well).
The study didn’t show the vaccine made people sicker or more vulnerable to infections. It raised a measurement question about how to interpret immune cell counts in older adults.
Some earlier research has suggested a link between shingles vaccination and lower dementia risk, but this study didn’t see the same pattern in the brain-related blood markers it measured.
That doesn’t necessarily contradict those findings. The vaccine might reduce dementia risk through indirect routes, like lowering overall inflammation, rather than by directly preventing the buildup of harmful proteins in the brain. Or the blood markers being measured might not capture the relevant brain changes.
The Shingles Vaccine That Was Studied vs. What’s Available Now
The vaccine examined in this research was Zostavax, the older single-dose formulation recommended for people 60 and up. In 2017, it was replaced by Shingrix, a newer two-dose vaccine that’s more effective at preventing shingles and is recommended starting at age 50.
Whether Shingrix produces the same anti-aging associations remains unknown. Its stronger immune response might amplify these effects, change them, or make no difference at all.
This study can’t prove the vaccine caused the biological age differences. It’s possible that people who get vaccinated are already healthier in ways the researchers couldn’t measure, even after accounting for other factors like income and existing medical conditions.
To determine if the vaccine slows aging, scientists would need to measure people’s biological markers before vaccination, give some people the shot and others a placebo, then measure again months or years later. That kind of research hasn’t happened yet.
If these associations do indeed hold up in future research, they’d suggest adult vaccines might do more than prevent specific diseases. They might play a role in healthier aging. The shingles vaccine already prevents a painful condition and costs less than many other medical interventions. If it also correlates with slower cellular aging, that’s an additional potential benefit worth investigating.
The bigger question is whether looking younger at a cellular level actually translates to feeling better, staying healthier, or living longer. That requires longer-term studies tracking real health outcomes, not just blood markers.
For now, the reasons to get the shingles vaccine remain the same as before: preventing shingles and its complications. The possibility of anti-aging benefits is intriguing but ultimately needs more research.
Disclaimer: This article reports on a single observational study that found associations between shingles vaccination and biological aging markers. The research cannot prove the vaccine causes slower aging, and results may not apply to the newer Shingrix vaccine currently in use. Readers should consult healthcare providers about vaccination decisions.
Paper Summary
Limitations
This was an observational study that measured people’s biology at a single point in time rather than tracking changes before and after vaccination. This design cannot prove the vaccine caused the differences observed. Healthier people may simply be more likely to get vaccinated.
The study examined only people who received Zostavax, the older vaccine formulation. Results may not apply to Shingrix, the newer vaccine now in use.
Sample sizes varied from 1,464 to 3,662 participants depending on which biological tests were available for each person. Some participants couldn’t recall exactly when they’d been vaccinated, requiring researchers to estimate the timing.
The adaptive immunity findings were difficult to interpret and may reflect limitations in how immune aging is measured rather than actual harm from vaccination.
Blood markers of brain health showed no association with vaccination despite previous research linking the vaccine to lower dementia rates, suggesting these particular markers may not capture the relevant protective mechanisms.
Funding and Disclosures
This work was supported by the National Institute on Aging at the National Institutes of Health (grant P30 AG017265). The Health and Retirement Study is supported by the National Institute on Aging (grant U01AG009740).
The authors declared no conflicts of interest.
Publication Details
Authors: Jung Ki Kim, PhD, and Eileen M. Crimmins, PhD, both from the Davis School of Gerontology at the University of Southern California | Title: “Association between shingles vaccination and slower biological aging: Evidence from a U.S. population-based cohort study | Journal: Journal of Gerontology: Biological Sciences (advance online publication) | DOI: 10.1093/gerona/glag008 | Publication Date: January 20, 2026








Lots of pro-vaccine bias here. “The adaptive immunity findings were difficult to interpret and may reflect limitations in how immune aging is measured rather than actual harm from vaccination.” Note that they questioned this result of lower adaptive immunity because it did not fit their goal of promoting the vaccine. They did not question any of the measurements or their limitations for the results that supported their bias. So they selectively questioned results that showed a negative effect, while giving a free pass to results that supported their hypothesis. That’s biased science.
Some other unanswered questions: If vaccination in general improves aging profiles, then what other vaccines have these study participants had, and when? People who get shingles vaccines are more likely to also get flu, COVID, and other recommended vaccines. On the other hand, if these results were due to the Zostavax only, which is no longer used, and may not apply to Shingrix, which is what is used today, then why study the outdated vaccine?
Finally, the concept of biological aging compared to chronological aging is suspect. People naturally age at different rates, depending on genetics and epigenitics. Comparisons to an idealized aging timeline ignore individual differences in aging that are not about pathology. Also, biomarkers tell the story about current conditions, and these can change. They may say nothing about future health.
Overall, this is a promotion for shingles vaccines.