(© Romario Ien - stock.adobe.com)
In A Nutshell
- Advanced dialysis shows promise: New kidney treatment techniques achieved impressive results in some studies, with one method showing 71% kidney recovery rates in critically ill patients.
- Results are frustratingly mixed: While some trials found major benefits, other well-designed studies showed no clear advantage over standard treatments, leaving doctors without clear guidance.
- Study design problems: Most research involved small groups with different patient types and treatment approaches, making it nearly impossible to determine which treatments actually work reliably.
- Better trials urgently needed: Researchers say larger, standardized studies are essential to finally prove whether these advanced techniques can consistently save kidney function in ICU patients.
When kidneys fail in the intensive care unit, the stakes couldn’t be higher. Patients often face two options: lifelong dialysis or death, with families watching helplessly as their loved ones fight for survival. Now, emerging research on advanced dialysis techniques is offering new hope — even as conflicting study results leave doctors and families without clear answers about which treatments actually work.
A comprehensive 2025 review published in the Journal of Intensive Medicine reveals a complex picture of kidney-saving treatments that show genuine promise but deliver frustratingly mixed results. While some advanced dialysis techniques achieved impressive outcomes like 71% kidney recovery rates, other well-designed trials found no clear benefit, highlighting an urgent need for better research to guide critical treatment decisions.
The Promise and the Problem
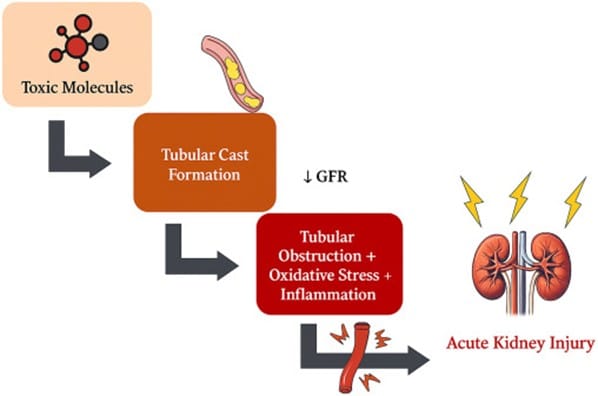
The challenge lies in a condition called cast nephropathy, where toxic proteins form casts that block kidney tubules like debris clogging pipes. This occurs in critically ill patients with conditions ranging from multiple myeloma to severe muscle breakdown. Traditional dialysis often can’t remove these harmful substances effectively, leaving kidneys to suffer permanent damage.
Enter advanced dialysis techniques designed to work like specialized filters, targeting specific toxic molecules before they cause irreversible harm. These include high-cutoff hemodialysis, medium-cutoff membranes, and polymethylmethacrylate (PMMA) dialysis — each engineered to remove different types of kidney-damaging substances more effectively than standard treatments.
The early results looked genuinely promising. According to a meta-analysis of five studies reviewed by researchers, high-cutoff hemodialysis achieved approximately 90% reduction in harmful free light chains — the toxic proteins that damage kidneys in multiple myeloma patients. In another study of 38 patients, PMMA dialysis combined with chemotherapy yielded an impressive 71% renal recovery rate at 60 days.
Medium-cutoff membranes also showed substantial promise in a retrospective study of 55 myeloma patients, producing a 70% reduction in one type of toxic protein and a 37% reduction in another. These numbers suggested that advanced dialysis techniques might finally offer a way to preserve kidney function in critically ill patients.
What the Research Shows
But the picture quickly became complicated when larger, more rigorous trials began reporting their results. The MYRE multicenter randomized trial found higher rates of dialysis independence at 6-12 months when high-cutoff dialysis was combined with chemotherapy in patients with biopsy-proven cast nephropathy. This seemed to confirm the promise of advanced techniques.
However, the EuLITE multicenter randomized trial — involving 90 myeloma patients — found no significant difference in survival or kidney outcomes when comparing high-cutoff dialysis to conventional therapy. This directly contradicted the earlier optimistic findings and left researchers scratching their heads about why results varied so dramatically between studies.
The conflicting evidence extends beyond just these major trials. The review, which synthesized literature through May 2024, found that while multiple advanced techniques showed potential benefits in smaller studies, robust randomized trials demonstrating definitive kidney benefits remained frustratingly elusive.
Part of the problem lies in the heterogeneous nature of the evidence. The researchers noted that many studies were small and non-randomized, making it difficult to draw firm conclusions about which treatments actually work. Different studies used different patient populations, treatment protocols, and outcome measures, making direct comparisons nearly impossible.
Why the Evidence Is Mixed
The review’s authors, led by researchers from Italian medical centers, identified several key reasons why the evidence remains so mixed. First, the narrative review methodology itself — while comprehensive — doesn’t follow the rigorous systematic approach that would allow for more definitive conclusions.
More importantly, the underlying studies varied dramatically in their design and execution. Some were observational studies that simply tracked patients receiving different treatments, while others were randomized controlled trials that more rigorously tested specific interventions. Sample sizes ranged from small case series to larger multicenter trials, each with different statistical power to detect meaningful differences.
The patient populations also differed significantly between studies. Some focused specifically on multiple myeloma patients with kidney damage, while others included various types of cast nephropathy from different underlying conditions. These differences make it challenging to determine which treatments work best for which patients.
Timing also emerged as a critical factor that wasn’t standardized across studies. Some research suggested that early intervention with biomarker-guided recognition might be key to success, but studies varied in when treatments were initiated and how kidney injury was detected and monitored.

What This Means for Patients and Families
For families facing kidney failure in the ICU, these mixed results present both hope and frustration. The promising signals from multiple studies suggest that advanced dialysis techniques may indeed offer better outcomes than traditional approaches. The 71% recovery rate seen with PMMA dialysis and the substantial toxin reductions achieved with high-cutoff membranes provide genuine reasons for optimism.
However, the conflicting trial results mean that doctors still lack clear guidance on which treatments work best for which patients. The EuLITE trial’s failure to show benefit despite the promising earlier studies highlights how complex medical research can be, and why definitive answers often take years to emerge.
The current uncertainty doesn’t mean these treatments are ineffective — it means we don’t yet know which ones work reliably enough to recommend as standard care. Some patients may indeed benefit from these advanced techniques, but predicting who will respond remains challenging without better research.
The researchers emphasized that prospective, adequately powered randomized trials comparing different extracorporeal modalities with standardized treatment protocols are urgently needed. These studies would need to include biomarker-guided timing and consistent outcome measures to finally establish which treatments provide definitive kidney and survival benefits.
Despite the promising early signals, the reality is that families and doctors still face difficult decisions without clear roadmaps. The next phase of research must move beyond small, heterogeneous studies toward larger, better-designed trials that can finally answer whether these advanced techniques can reliably save kidney function in critically ill patients. Until then, the promise remains tantalizing but unproven, leaving hope tempered by the sobering recognition that definitive answers are still needed.
Disclaimer: This research summary is for educational purposes only and does not constitute medical advice. Treatment decisions for kidney failure and intensive care support should always be made in consultation with qualified healthcare professionals and specialists.
Paper Notes
Limitations
The review is designed as a narrative synthesis rather than a systematic review, meaning it does not adhere to a predefined protocol, which limits the reproducibility of the search strategy and selection process. Additionally, the available evidence is highly heterogeneous, consisting primarily of small, non-randomized observational studies and case reports. Consequently, the analysis lacks robust randomized controlled trials necessary to establish definitive renal benefits or causal links between extracorporeal strategies and patient outcomes.
Funding and Disclosures
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors. The authors declare that they have no known competing financial interests or personal relationships that could have appeared to influence the work reported in this paper.
Publication Details
De Rosa, Silvia, Fiorenza Ferrari, Diana Zarantonello, Alessia Dalpiaz, and Sergio Lassola. “Cast nephropathy in the ICU: Early recognition and extracorporeal strategies to improve outcomes.” Journal of Intensive Medicine, 2025. DOI: 10.1016/j.jointm.2025.10.006. The study is a narrative review based on a literature search of the PubMed database up to May 4, 2024, and manual screening of reference lists, covering observational studies, randomized controlled trials, and case reports regarding critically ill ICU patients with cast-induced acute kidney injury. Silvia De Rosa, Diana Zarantonello, Alessia Dalpiaz, and Sergio Lassola are affiliated with Santa Chiara Hospital, APSS, Trento, Italy, with De Rosa also affiliated with the Silvia De RosaUniversity of Trento. Fiorenza Ferrari is affiliated with Fondazione IRCCS Cà Granda Ospedale Maggiore Policlinico, Milano, Italy.







