
Credit: Photo by Logan Stone on Unsplash
In A Nutshell
- Older adults who regularly napped in the morning had a 30% higher relative risk of dying over the study period compared to those who napped in the early afternoon.
- Longer and more frequent naps also predicted higher mortality, independent of nighttime sleep quality and chronic health conditions.
- Morning napping may signal underlying health problems rather than cause them, and cognitive decline could be a key factor driving the association.
- Wearable sleep trackers could one day help doctors flag at-risk patients earlier by monitoring daytime nap patterns over time.
A nap before lunch might feel harmless, but a long-running study suggests it could be a warning sign worth paying attention to.
Researchers tracked more than 1,300 older adults for up to 19 years and found that people who regularly napped in the morning had a 30% higher relative risk of dying during the study period compared with those who napped in the early afternoon. That gap generally held up in the main analysis even after researchers accounted for nighttime sleep quality, chronic health conditions, depression, physical activity, disability, and medication use. In statistical terms, being a habitual morning napper carried roughly the same added death risk as being about two and a half years older.
Published in JAMA Network Open, the study was led by a team at Harvard Medical School, Mass General Brigham, and Rush University Medical Center. Rather than relying on self-reported habits, researchers used wrist-worn activity monitors to track exactly when, how long, and how often participants slept during the day, making it one of the first studies to measure nap timing with this precision and connect those patterns to long-term survival.
How Researchers Tracked Napping and Death Risk
Data came from the Rush Memory and Aging Project, an ongoing study initiated in 1997 that enrolls adults aged 56 and older from retirement communities, senior housing, and church groups across northern Illinois. Starting in August 2005, participants wore a small wrist device on their non-dominant hand for up to 14 days, continuously recording movement and rest to identify sleep episodes between 9 a.m. and 7 p.m.
Of the 1,338 community-dwelling participants in the final analysis, the average age was about 81, and 76% were female. Nearly all of them, 99%, took at least some naps during the monitoring period. Over an average follow-up of roughly 8.3 years, 926 participants, about 69%, died.
Researchers tracked four nap characteristics: average daily nap length, number of naps per day, how much nap length varied from day to day, and the time of day when naps were most concentrated. Participants were sorted into three groups: morning nappers, early afternoon nappers, and late afternoon nappers.
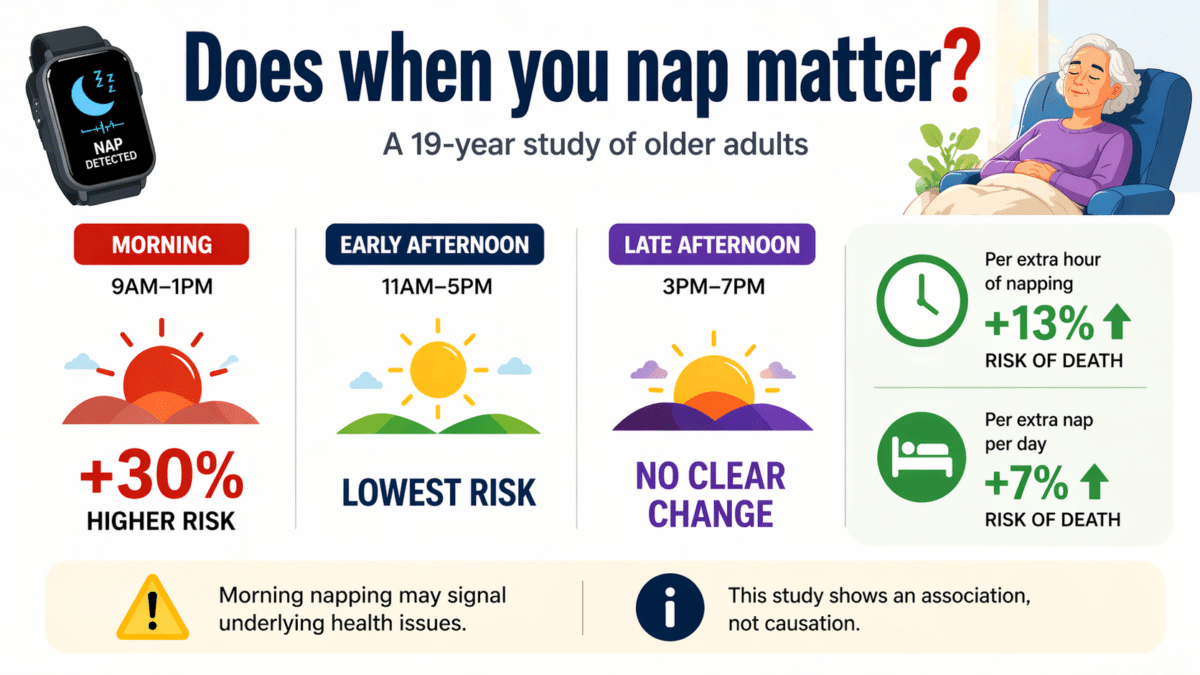
Morning Naps Stood Out as the Biggest Risk Factor
After adjusting for age, sex, race, education, nighttime sleep, body mass index, depression, chronic conditions, medications, physical activity, and disability, both longer and more frequent napping predicted a higher chance of dying.
Each additional hour of daily nap time was linked to a 13% increase in relative death risk, and each additional nap per day added another 7%. Those numbers compound quickly for older adults who nap often and long.
But the most notable result involved timing. Morning nappers had a 30% higher relative death risk compared with early afternoon nappers in the fully adjusted analysis. Late afternoon nappers fell in between, showing no statistically significant difference from either group once all health factors were accounted for.
One idea the researchers tested but did not find support for: that nap lengths varying widely from day to day would predict higher death risk. That kind of variability showed no meaningful connection to mortality.
Why Morning Napping May Be a Warning Sign
Researchers offered several possible explanations. Napping when healthy individuals are typically alert may reflect underlying health problems, perhaps disrupted internal body clocks, hidden cardiovascular issues, or conditions not yet diagnosed. Sleep disruption and disrupted sleep-wake rhythms have been associated with elevated blood pressure, reduced blood vessel function, and heightened stress responses, all of which may be linked to increased cardiovascular risk.
Low-grade, persistent inflammation may also be part of the picture. Prior research found that habitual nappers tend to have higher levels of inflammation markers in their blood, and some evidence points to morning and evening fatigue arising from distinct biological pathways, which could help explain why the timing of a nap carries different health weight than simply taking one.
Perhaps most telling, the link between napping and death risk held up even after accounting for how well participants slept at night. Morning napping is not simply a sign that someone had a rough night. It appears to be a red flag in its own right, one that reflects something about a person’s underlying health that a full night of sleep cannot explain away.
Important Caveats
Researchers were clear that this was an observational study and cannot prove morning napping causes higher mortality. Excessive or poorly timed napping is likely a symptom of declining health rather than a driver of it. When participants with mild cognitive impairment or dementia were excluded, the association between nap timing and mortality weakened and lost statistical significance, raising the question of whether cognitive decline may be driving part of the relationship.
With wearable sleep trackers becoming more common, the researchers see a real opportunity to monitor nap patterns and flag potential health risks earlier. As the paper concludes, integrating wearable-based nap assessments into routine care “could enable clinicians to identify older adults with high daytime sleep burdens and initiate timely evaluations or preventive interventions.”
Fitness trackers already count steps and flag irregular heartbeats. A persistent pattern of morning napping may soon be one more data point doctors use to get ahead of trouble.
Disclaimer: This article is based on an observational study and does not establish that morning napping causes increased mortality. Associations reported here do not apply to all individuals, and napping habits vary widely across ages, cultures, and health conditions. Consult a qualified healthcare provider with any concerns about sleep health.
Paper Notes
Limitations
Several limitations apply to this study. Wrist actigraphy, while objective, cannot always distinguish actual sleep from quiet rest or stillness, which could introduce some misclassification of nap episodes. No concurrent self-reported nap data were collected, so the researchers could not directly compare the two methods. The study population was predominantly White (93.3%) and drawn from community-dwelling older adults in a specific region of northern Illinois, limiting how broadly these results apply. Cultural norms around napping, such as the afternoon siesta common in Hispanic-Latino, Mediterranean, and Chinese communities, were not represented, and napping may carry different health meanings in those contexts. Participants were also older and retired, so findings may not translate to younger or working-age adults whose nap patterns are shaped by job schedules. Seasonal variation in sleep and napping was not examined. Finally, specific causes of death were not analyzed, leaving open the question of which diseases are most tightly linked to nap timing.
Funding and Disclosures
This study was supported by a grant from the Alzheimer’s Association Research Fellowship to Promote Diversity (Dr. Chenlu Gao) and a grant from the National Institute on Aging (Dr. Kun Hu). Rush University’s Memory and Aging Project received additional funding from the National Institutes of Health. Several authors reported receiving grants from organizations including the Alzheimer’s Association, the American Academy of Sleep Medicine Foundation, the National Heart, Lung, and Blood Institute, and the National Institute of General Medical Sciences. Drs. Hu and Peng Li reported receiving personal fees from iFutureLabs outside the submitted work. Dr. Li also reported consulting fees and an honorarium from China Pharmaceutical University and Shandong University. No other disclosures were reported. Funders had no role in study design, data collection, analysis, or the decision to publish.
Publication Details
Authors: Chenlu Gao, PhD; Ruixue Cai, PhD; Xi Zheng, MS; Arlen Gaba, MD; Lei Yu, PhD; Aron S. Buchman, MD; David A. Bennett, MD; Lei Gao, MD; Kun Hu, PhD; Peng Li, PhD | Affiliations: Department of Anesthesiology and Division of Sleep Medicine, Mass General Brigham, Harvard Medical School; Division of Sleep and Circadian Disorders, Brigham and Women’s Hospital; Tufts Medical Center; Rush Alzheimer’s Disease Center, Rush University Medical Center; Broad Institute of MIT and Harvard | Journal: JAMA Network Open | Title: “Objectively Measured Daytime Napping Patterns and All-Cause Mortality in Older Adults” | Published: April 20, 2026 | DOI: 10.1001/jamanetworkopen.2026.7938







