
(Credit: Andrea Piacquadio from Pexels)
Why Pounding Headaches Get Worse When The Air Is Dirty And The Weather Turns
In A Nutshell
- A 23-year study of over 7,000 migraine patients found that traffic-related air pollution and sunlight intensity were associated with higher odds of emergency migraine visits the following day.
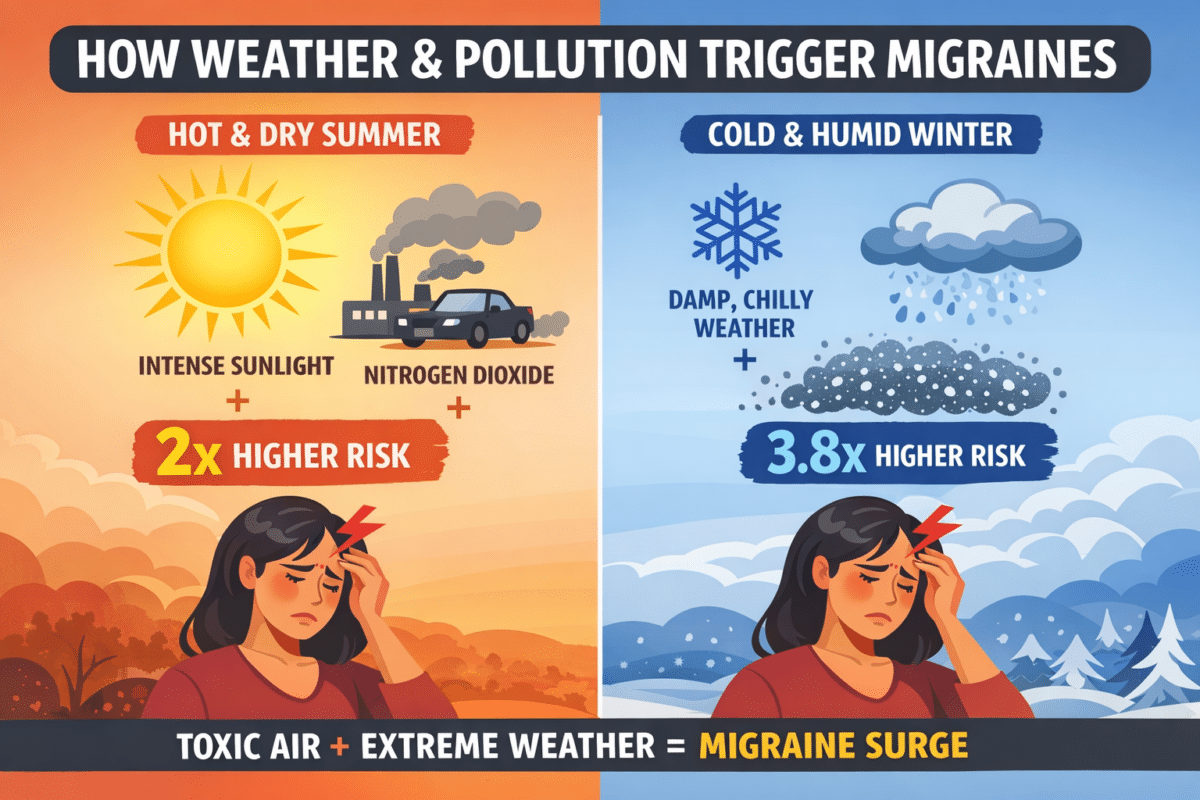
- Hot, dry summer weeks roughly doubled the migraine risk linked to nitrogen dioxide spikes; cold, humid winter weeks nearly quadrupled the risk tied to fine airborne particles.
- Months of accumulated pollution exposure were linked to increased overall migraine activity, suggesting that dirty air may raise the brain’s baseline vulnerability over time.
- Researchers say the findings could eventually support migraine prediction tools that use real-time air quality and weather data to help patients prepare for high-risk days.
For the roughly one billion people worldwide who live with migraines, the question “What triggered this?” is a constant source of frustration. Many sufferers have long suspected that weather and air quality play a role in their attacks, but solid scientific evidence has been hard to come by. Now, a large-scale study spanning more than two decades offers some of the strongest population-level support for those suspicions.
Moreover, it reveals one of the most notable findings in recent migraine research: the air people breathe and the weather outside may be working together in season-specific combinations to push vulnerable brains past their tipping point.
Researchers in Israel tracked over 7,000 migraine patients across 23 years and found that spikes in nitrogen dioxide, a common traffic-related pollutant, along with increases in sunlight intensity (measured as solar radiation), were associated with a higher risk of emergency migraine visits the very next day, though the study cannot prove cause and effect. What stood out was what happened when those daily pollution spikes collided with certain weekly weather patterns. During summer weeks marked by extreme heat and low humidity, the effect of nitrogen dioxide on migraine risk roughly doubled. During cold, humid winter weeks, the risk tied to fine airborne particles nearly quadrupled.
Published in the journal Neurology, the research proposes a “layered model” for understanding how the environment influences migraine. Rather than pointing to a single trigger, it frames short-term pollution spikes as the match, while the broader weather pattern of the surrounding week acts as the kindling.
Tracking 23 Years of Migraines, Pollution, and Weather
Researchers drew from the Negev Migraine Cohort, a database of patients identified through medical records from Clalit Health Services and Soroka University Medical Center in Be’er Sheva, a city of roughly 220,000 in the arid northern Negev desert. Patients qualified if they were adults aged 18 or older with a migraine diagnosis or a prescription for triptans, a class of medication used to treat acute migraine attacks. Daily air pollution and weather data came from a dense network of fixed monitoring stations; each patient was assigned exposure values based on the nearest station to their home.
A key strength of the design was that researchers compared each patient to themselves, examining the environmental conditions on the day before a migraine emergency visit versus conditions on similar days when that person did not seek care. Because each person served as their own control, fixed personal factors like genetics, sex, and chronic health conditions were automatically accounted for.
Among the 7,032 patients, about 77% were female, with an average age of roughly 47 years. Nearly a third had at least one emergency migraine-related health care visit during the study period, producing a total of 24,608 such events.
What the Migraine Study Found About Pollution and Weather
When researchers examined conditions in the days before an emergency visit, nitrogen dioxide exposure one day prior stood out. People were 41% more likely to seek emergency care at their peak pollution exposure compared to their lowest, a figure that reflects each person’s individual exposure range over the full study period rather than typical day-to-day changes. Sunlight intensity the day before was tied to 23% higher odds.
Fine airborne particles, tiny specks often produced by combustion or dust, did not show a significant short-term trigger effect on their own. Over longer time frames, however, they mattered. Higher fine particle levels in the preceding three-month window were linked to about a 9% increase in triptan use; nitrogen dioxide showed a similar roughly 10% increase. Day-to-day pollution spikes appeared to act as immediate triggers, while months of accumulated exposure seemed to ramp up overall migraine activity, suggesting two processes that may operate on different timescales.
When Weather Patterns Turned Up the Dial on Migraine Risk
Researchers also examined how weekly weather patterns changed the impact of daily pollution spikes, dividing weeks into extreme categories by temperature and humidity and measuring how those conditions altered the relationship between daily pollution and emergency visits.
During hot, dry summer weeks, nitrogen dioxide’s effect was dramatically amplified. Cold, humid winter weeks intensified the effect of fine airborne particles to an even greater degree. Researchers noted that an abrupt weather shift, such as a hot day during an otherwise cold and humid week, may cause a larger physical disruption than the same temperature on a day that fits the surrounding pattern.
Sunlight intensity emerged as a significant and independent trigger, a factor the authors noted has rarely been examined within a broader environmental framework. Exploratory analyses added another wrinkle: the effects of nitrogen dioxide and temperature were more pronounced among men than women, a counterintuitive result given that migraines are far more common in women.
For migraine patients, the practical takeaway is validating. Forecasted high-risk exposure periods could guide preventive action, from limiting outdoor activity and using air filtration to starting short-term preventive medications before a bad stretch arrives. If the layered model holds up, it could eventually be built into migraine prediction apps that incorporate real-time air quality and weather data.
Migraines often strike without warning and leave patients scrambling for answers. This research points toward a future where at least some of those answers arrive in advance, written in the day’s air quality forecast and the week’s weather report. As the researchers concluded, their findings support moving migraine management “from a reactive treatment approach to a proactive, risk-based, and time-sensitive intervention.”
Disclaimer: This article is based on peer-reviewed research published in an academic journal and is intended for informational purposes only. It does not constitute medical advice. Readers with health concerns should consult a qualified healthcare provider.
Paper Notes
Limitations
The study relied on emergency health care encounters as its primary outcome, meaning it captured only the most clinically severe migraine episodes. Migraines managed at home were not included, likely leading to an underestimation of total migraine activity. Exposure was assigned based on fixed monitoring stations rather than individual-level measurements, and the study could not account for personal behaviors such as time spent indoors, use of air conditioning or air filtration, occupational setting, or daily mobility. Migraine patients may intentionally avoid outdoor activity during perceived high-risk conditions, which could further reduce measured associations. Triptan dispensation data were available only for 46.7% of patients and measured in 90-day intervals, limiting temporal precision. Data on preventive migraine therapies, including CGRP monoclonal antibodies, were not consistently available in the electronic medical records. Pollutants and lagged exposures were highly correlated, so the odds ratios reported do not represent fully independent tests. Finally, the study was conducted in a single city with a specific arid climate, which may limit generalizability to other geographic regions.
Funding and Disclosures
The study was supported by the Ministry of Innovation, Science and Technology, Israel (grant number: 1001591849; proposal no. 5604, 2022). The article processing charge was funded by the authors. Authors Ido Peles, Lena Novack, Michal Gordon, Batia Sarov, and Victor Novack reported no disclosures relevant to the manuscript. Gal Ifergane received consulting fees and honoraria from Teva, Novartis, Eli Lilly, Pfizer, and Abbvie, and received research support from Teva and Pfizer.
Publication Details
Title: Acute Environmental Triggers and Intermediate-Term Modulators of Emergency Migraine-Related Health Care Encounters | Authors: Ido Peles, Lena Novack, Michal Gordon, Batia Sarov, Victor Novack, and Gal Ifergane | Affiliations: Faculty of Health Sciences, Ben-Gurion University of the Negev; Clinical Research Center, Soroka University Medical Center; School of Public Health and Negev Environmental Health Research Institute, Ben-Gurion University of the Negev; Internal Medicine Division, Soroka University Medical Center; Department of Neurology, Brain Medicine Division, Soroka University Medical Center, all in Be’er Sheva, Israel. | Journal: Neurology, Volume 106, Number 9, May 12, 2026 | DOI: 10.1212/WNL.0000000000214936 | Received: September 17, 2025. Accepted: February 17, 2026. Handling editor was Associate Editor Rebecca Burch, MD.







