
(© Monkey Business - stock.adobe.com)
Only 1 in 1,000 People With Early Cognitive Decline See a Specialist. A Home Blood Test Could Change That.
In A Nutshell
- A home finger-prick blood test detected two Alzheimer’s-linked proteins that correlated with memory and cognitive performance in older adults.
- Only about 1 in 1,000 people with early cognitive decline currently reaches a specialist; this kind of test could help close that gap.
- A surprise finding: one protein, GFAP, was linked to heart disease history rather than Alzheimer’s specifically, suggesting the two markers may flag different types of cognitive risk.
- Nearly 80% of participants completed the test on their own at home, and about 78% said they’d use it routinely, with no clinic visit needed.
A small pinprick on the fingertip. A dried blood spot card dropped in the mailbox. Results that could help flag whether someone needs a fuller medical evaluation for Alzheimer’s disease, all without a waiting room, a specialist appointment, or a vial of blood drawn from your arm. That future may be closer than most people think.
A new study published in Nature Communications found that two proteins linked to Alzheimer’s disease, detected through a self-administered finger-prick blood test completed at home, correlated meaningfully with memory and cognitive performance in older adults, and in some cases with measures of daily functioning. To be clear, this test would not diagnose Alzheimer’s disease. Researchers explored it as a way to flag people who may need a fuller medical evaluation, including those who might otherwise never reach a specialist clinic at all.
According to the paper, only about one in every 1,000 people with early cognitive decline currently receives a specialist evaluation. A reliable, easy-to-use home test could change that equation, not just in the UK, where the study was conducted, but globally, especially in rural areas where specialized medical care is hard to come by.
Two Proteins, One Small Card
Researchers focused on two proteins in the blood associated with Alzheimer’s disease. One, called p-tau217, is considered among the strongest blood-based signals for Alzheimer’s-related brain changes. Another, called GFAP, is a marker of brain cell stress and inflammation. Both have been studied using traditional blood draws, but this research examined whether they could be reliably detected from tiny amounts of blood collected at home through a finger prick, similar to the one used for at-home blood sugar checks, but with the blood applied to a dried blood spot card and mailed to a lab for analysis.
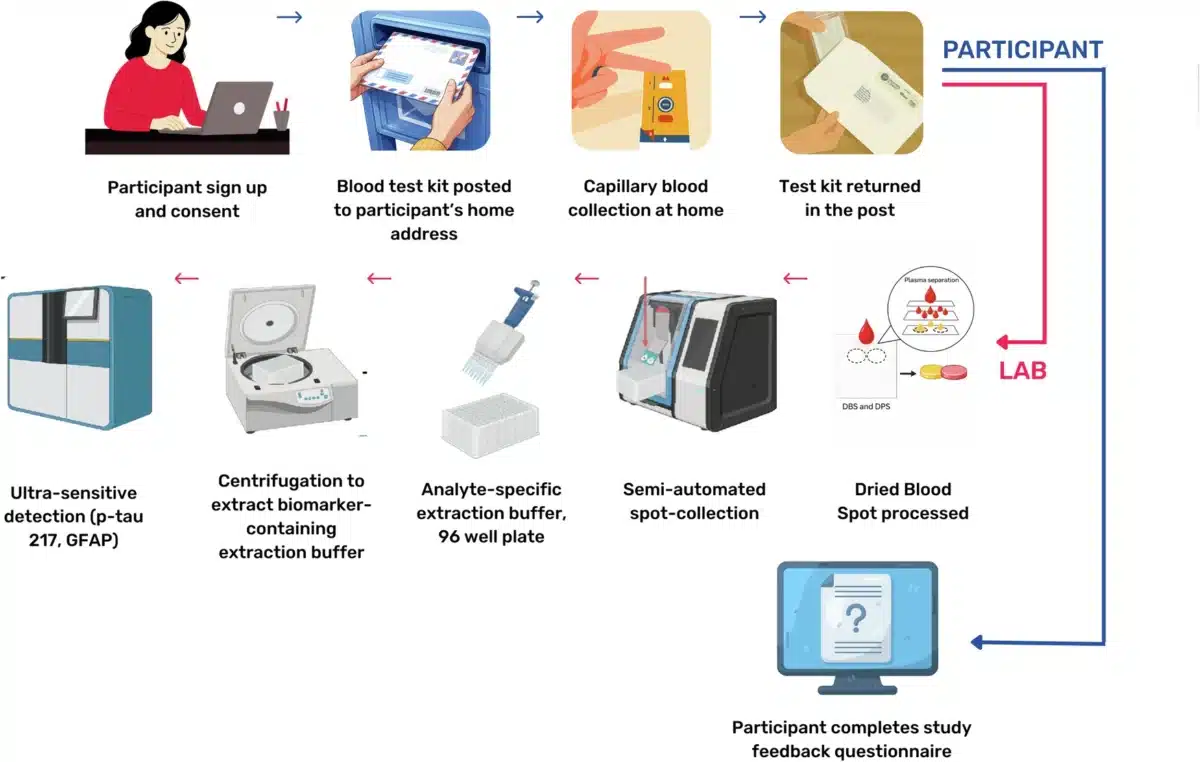
174 Older Adults Tested an Alzheimer’s Biomarker Kit at Home
Researchers recruited 226 participants through the PROTECT research program in the UK. Of those, 174 completed the blood test kits and were included in the final analysis. The average age was about 66, and just over half were female. The cohort included cognitively healthy participants, people with mild cognitive impairment, and 28 people diagnosed with dementia.
Participants completed a computerized cognitive test covering memory, attention, and mental skills needed for planning and problem-solving, and filled out standardized scales measuring their ability to handle daily activities like managing finances or medications.
A smaller subgroup of 40 participants also gave a traditional blood draw at a clinic, allowing researchers to directly compare the two collection methods.
Home Finger-Prick Results Matched Clinical Blood Draws
Both proteins detected through the finger-prick method correlated with performance on cognitive and functional tests. P-tau217 showed the strongest associations, particularly with memory scores and daily functioning. GFAP also correlated with planning ability and daily living skills. When researchers compared home finger-prick results against the traditional clinical blood draw in the 40-person subgroup, the correlation was strong, both in people with dementia and those without.
Researchers also developed a two-cutoff risk-sorting approach, combining p-tau217 levels with memory test scores to divide participants into high-risk, low-risk, and intermediate groups. People in the high-risk group performed worse on attention, executive function, and daily-function measures. People in the low-risk group performed better across the board. About 80% of participants completed the test without any assistance, guided only by written and video instructions. Nearly 78% said they would be willing to use it regularly as part of their routine healthcare.
A Surprise Finding About Heart Health
One of the more unexpected results involved GFAP. Even though both proteins identified people with cognitive problems, there was little overlap between individuals who tested high on GFAP and those who tested high on p-tau217. Only about 6% of participants were elevated on both.
Further analysis found that people with elevated GFAP were nearly five times more likely to report a history of heart disease compared to those with normal GFAP levels. P-tau217 showed no such connection. GFAP may be picking up a different pattern of risk, possibly related to vascular health, though that part of the study relied on self-reported heart-disease history and needs confirmation. For clinicians trying to understand why a patient’s thinking is declining, having both markers could paint a more complete picture.
Beyond everyday healthcare, this technology could also reshape how clinical trials for new Alzheimer’s treatments recruit participants. Screen failure rates in such trials, meaning people who enroll but don’t qualify after more detailed testing, can reach 90%. A simple at-home pre-screening tool could help researchers identify eligible participants far more efficiently.
For the many people with early cognitive changes who never make it through the door of a specialist clinic, a reliable, affordable, mailbox-ready blood test could be the first real shot at catching potential problems early. And for Alzheimer’s research and care, earlier evaluation is increasingly the goal.
Disclaimer: This article is based on a peer-reviewed research study, but findings have not been independently replicated and should not be taken as medical advice. The test described is not currently available for clinical or consumer use and has not been approved as a diagnostic tool. Anyone with concerns about memory or cognitive health should consult a qualified medical professional.
Paper Notes
Limitations
The authors identify several important limitations. While 80% of participants successfully completed the self-test independently, instructional materials will need further improvement to increase completion rates. The correlation between home-collected and clinically-drawn blood samples, though strong, leaves room for refinement in collection and processing protocols. The GFAP cardiovascular analysis relied on a single self-reported questionnaire item rather than verified clinical data, limiting its precision. The study has not yet been validated in an independent cohort, and the long-term predictive value of these home-collected biomarkers has not been established. Findings have also not been validated against brain imaging techniques that measure amyloid and tau buildup directly. The authors stress that this technology is intended for triage, not diagnosis, given the low sensitivity of the risk thresholds used.
Funding and Disclosures
This study was funded by the NIHR Invention for Innovation funding stream (NIHR204824) and by the Exeter Biomedical Research Centre (NIHR203320). Additional support came from the NIHR Collaboration for Leadership in Applied Health Research and Care South-West Peninsula and the NIHR Health Tech Research Centre in Brain Health. Further funding was provided through grants from the Swedish Research Council, the European Union’s Horizon Europe and Horizon 2020 programs, the Alzheimer Drug Discovery Foundation, the Alzheimer’s Association, and several other foundations and institutions listed in the paper. The views expressed are those of the authors and not necessarily those of the NIHR or the UK Department of Health and Social Care. Several authors, including Anne Corbett, Nicholas Ashton, Laia Montoliu-Gaya, Clive Ballard, Jeffrey Cummings, and Henrik Zetterberg, disclosed consultancy relationships and financial interests with multiple pharmaceutical and biotechnology companies, as detailed in the paper’s competing interests section. Cognitive tests were provided by Cognitron, Wesnes Cognition, and ECog Pro Ltd.
Publication Details
Paper title: Alzheimer’s Disease blood biomarkers measured through remote capillary sampling correlate with cognition in older adults | Authors: Anne Corbett, Millie Sander-Long, Nicholas J. Ashton, Hanna Huber, Jakub Vavra, Luisa Sophie Braun-Wohlfahrt, Henrik Zetterberg, Laia Montoliu-Gaya, Jeffrey Cummings, Freya Bateman, Christine Davis, and Clive Ballard | Journal: Nature Communications | DOI: https://doi.org/10.1038/s41467-026-71448-2







