
(© Svyatoslav Lypynskyy - stock.adobe.com)
In A Nutshell
- Your brain amplifies cold signals during fever. When you’re sick, a molecule called prostaglandin E2 cranks up activity in neurons that make normal temperatures feel freezing cold: even though your body is running hot.
- The feeling and the shivering use different pathways. Scientists discovered that the brain circuit creating the cold sensation during fever is separate from the one that triggers automatic responses like shivering and heat production.
- It goes to your emotions, not your thermostat. The amplified cold signals travel to your amygdala (emotion center) rather than your brain’s temperature control region, which is why chills feel so unbearable.
- This may be an evolutionary advantage. By making you feel cold during infection, your brain motivates warmth-seeking behaviors that help raise body temperature and support immune function: without burning energy through shivering.
The thermometer reads 102°F. Your skin burns to the touch. Yet you’re shivering under three blankets, convinced the room is an icebox.
It’s one of the strangest sensations of being sick. Your body is blazing hot, but you feel absolutely freezing. Now, scientists working with rats have identified a specific neural pathway that may explain this paradox and why it happens in the first place.
Researchers at Nagoya University in Japan discovered that a molecule called prostaglandin E2, which the body produces during infection, amplifies cold signals traveling through a specific relay station in the brain. In rats, this amplification makes normal temperatures feel unbearably cold, driving them to seek warmth even as their body temperature rises. The finding, published in The Journal of Physiology, reveals that the brain uses largely separate circuits for the feeling of being cold versus automatic responses like shivering.
The Relay Station That Shifts Into Fever Mode
The action happens in a brain region called the lateral parabrachial nucleus. This region can be likened to a switchboard operator for temperature information traveling from your skin up to your brain. During infection, prostaglandin E2 activates specific neurons in this relay station that connect to your amygdala, the brain’s fear and emotion center.
To prove this, Yahiro’s team ran a clever experiment with rats. They built a chamber with two side-by-side floor plates maintained at different temperatures: one at 28°C (about 82°F, comfortable for rats) and another at 39°C (102°F, an innocuously warm temperature). Healthy rats avoided the warm plate and lounged on the comfortable one, as expected.
But rats that received tiny injections of prostaglandin E2 directly into this brain relay station did the opposite. They fled the comfortable plate and huddled on the warm one. Their core body temperature increased as they sought out heat, driven by an amplified sensation of cold.

Why It Goes to Your Emotions, Not Your Thermostat
When the researchers traced where these activated neurons send their signals, they found dense connections to the amygdala, the part of your brain that processes threats and generates the urge to avoid unpleasant things. It’s why pain feels bad, why scary movies make you jumpy, and apparently, why chills feel so awful you’ll do anything to get warm.
But very few connections went to the brain’s actual thermostat (the preoptic area) that controls automatic responses like shivering and ramping up heat production in your body’s brown fat.
To confirm this split, researchers monitored the nerves controlling brown fat while injecting prostaglandin E2 into different brain regions. When they injected it into the relay station, nothing happened. No shivering signals. No activation of brown fat thermogenesis. No measurable automatic fever response.
But when they injected prostaglandin E2 into the thermostat region itself, brown fat nerves fired like crazy, body temperature shot up, and all the classic automatic fever responses kicked in.
The study suggests two largely separate pathways for fever. One creates the cold sensation that makes you pile on blankets. The other triggers shivering and heat production. They often run simultaneously during illness, but they operate through different wiring.
Why This Happens
Researchers and other scientists have long argued that raising body temperature during infection helps the immune system work better and slows down many germs. A fever between 100-104°F can hamper bacterial growth while boosting immune cell activity. By making normal temperatures feel unbearably cold, the brain may motivate behavioral changes that support fever (piling on blankets, cranking the heat, curling up in warm spots) without requiring the metabolic energy that shivering demands.
The amygdala handles this well because it specializes in generating avoidance behaviors. Cold temperatures pose a real survival threat (hypothermia), so the brain routes cold information to the emotion center to make sure it feels urgent and unpleasant. During infection, prostaglandin E2 amplifies this pathway, cranking up the signal until the amygdala responds as if facing severe cold, even during a fever.
Previous studies in rats showed that animals with damage to their thermostat region can still develop behavioral fever by seeking warmth, suggesting this pathway can function independently.
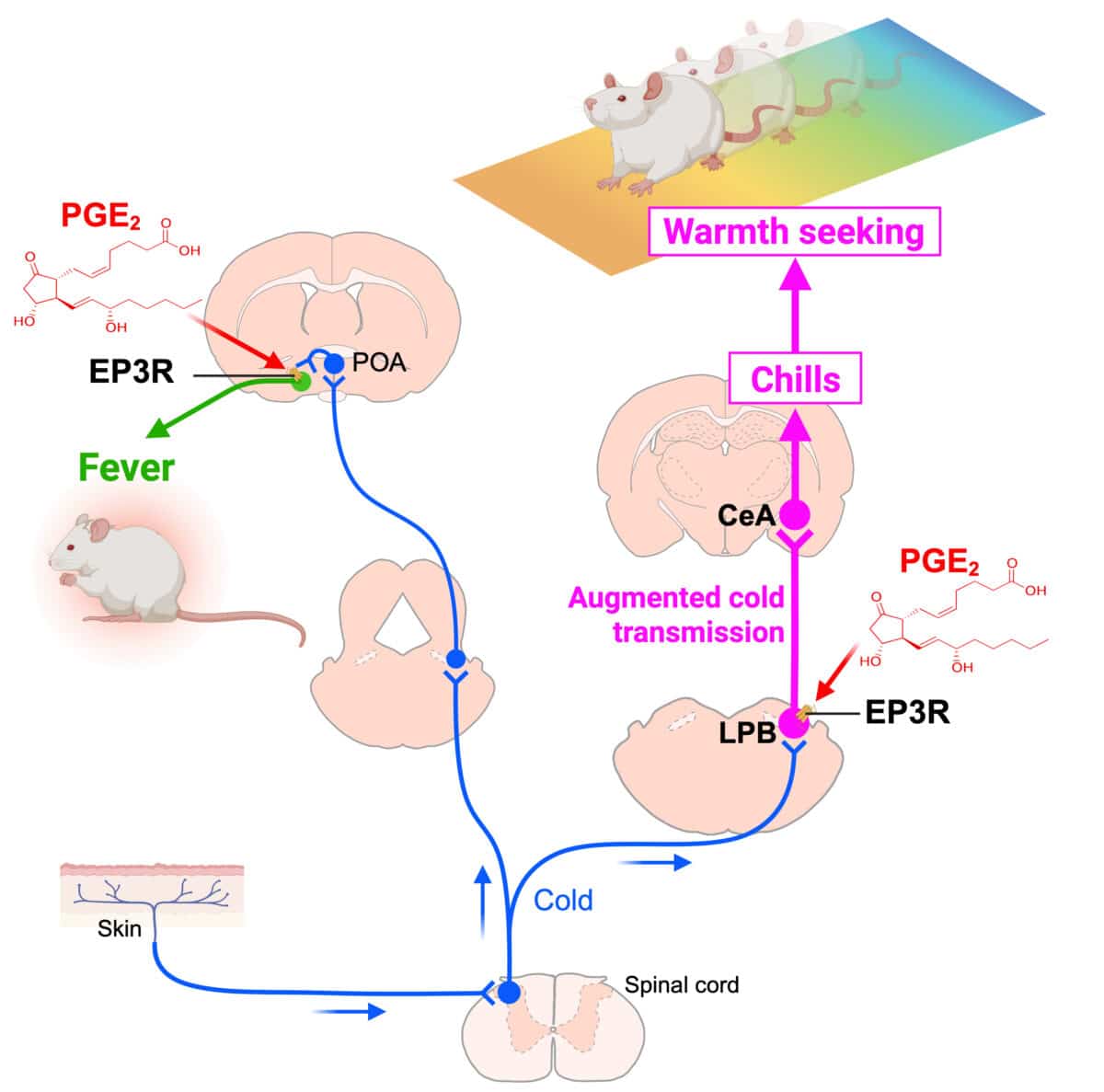
When Hot Feels Cold
What makes chills particularly miserable is the disconnect. Your emotional brain signals danger from cold while your thermostat registers rising temperature. It’s not just ordinary coldness: it’s coldness that doesn’t match reality, that persists even when you logically know you have a fever.
The researchers found that the relay station actually contains two separate groups of cold-sensing neurons, building on previous studies of temperature pathways. One group sends signals to the thermostat to trigger shivering. The other sends signals to the amygdala to create the feeling of cold. During infection, prostaglandin E2 specifically amplifies the emotional pathway.
This discovery clarifies previous assumptions. Earlier studies noted that prostaglandin receptors existed in the relay station but their function was unclear. This new research suggests these neurons help generate the cold sensation associated with fever rather than the automatic physical responses.
For anyone who’s ever huddled under blankets while running a 102° fever, the research provides a potential explanation. The brain may be running an adaptive program that amplifies cold signals to drive warmth-seeking behavior. Whether the same pathway functions identically in humans requires further study, but the basic thermoregulatory circuits are highly conserved across mammals.
Disclaimer: This article reports on research conducted in laboratory rats. While the basic brain circuits controlling temperature regulation are highly conserved across mammals, the subjective experience of fever chills in humans has not been directly studied using these methods. The findings provide a plausible biological mechanism but should not be interpreted as definitive proof of how human fever chills work.
Paper Notes
Study Limitations
All experiments used male rats aged 8-12 weeks, so sex differences and age-related changes weren’t explored. The temperature tests used only one comparison (28°C versus 39°C), and experiments were performed during rats’ normal rest period, which could affect behavior. The pharmacological compounds, while carefully validated, could have off-target effects that genetic studies might better control. Extrapolating from rat neurobiology to human subjective experience requires caution, though basic thermoregulatory circuits are highly conserved across mammals. The study did not directly test whether the behavioral pathway conserves metabolic energy compared to shivering.
Funding and Disclosures
This research received support from Moonshot R&D (JPMJMS2023) from the Japan Science and Technology Agency; Grants-in-Aid for Scientific Research (JP25K10154, JP21K06767, JP23H00398, JP20H03418) from Japan’s Ministry of Education, Culture, Sports, Science and Technology; and the Japan Agency for Medical Research and Development (JP25gm1910003). Takaki Yahiro received additional support from the Takeda Science Foundation. Ono Pharmaceutical provided prostaglandin receptor compounds but had no role in study design, data collection, analysis, or manuscript preparation. The authors declared no competing interests.
Publication Details
Title: The pyrogenic mediator prostaglandin E2 elicits warmth seeking via EP3 receptor-expressing parabrachial neurons: a potential mechanism of chills | Authors: Takaki Yahiro, Yoshiko Nakamura, and Kazuhiro Nakamura, Department of Integrative Physiology, Nagoya University Graduate School of Medicine, Nagoya, Japan | Journal: The Journal of Physiology (2026), published by The Physiological Society | DOI: 10.1113/JP289466 | Received: June 15, 2025; Accepted: January 7, 2026; Published online: February 6, 2026







