
(© Op Creator - stock.adobe.com)
Brain Scans of Kids With ADHD Reveal Two Distinct Neurological Subgroups
In A Nutshell
- Brain scans of children with ADHD reveal two distinct subgroups with opposite gray matter patterns: one group has more gray matter than neurotypical peers, the other has less.
- When all children with ADHD were analyzed together, no brain differences appeared at all. Only after splitting them into subgroups did the opposing patterns emerge.
- Subtype 1 is most closely linked to inattentiveness and involves the frontal lobes and cerebellum. Subtype 2 is tied to broader ADHD severity and centers on the cerebellum and hippocampus.
- Researchers suggest the two subgroups might eventually benefit from different treatment approaches, though this has not yet been tested in clinical trials.
Brain imaging studies have long linked ADHD to differences in certain brain regions, but those findings have been frustratingly inconsistent across studies. A new paper published in General Psychiatry may help explain why. Researchers in China found that children with ADHD appear to cluster into two neurologically distinct subgroups, and the brain patterns separating them run in opposite directions.
Gray matter is the tissue most closely linked to thinking, attention, and decision-making. More of it isn’t automatically better or worse. What makes this finding worth attention is that two groups of children carrying the same ADHD diagnosis showed opposing gray matter patterns compared to healthy peers, one group with more than typical, one with less.
For decades, ADHD has been officially classified into three behavioral subtypes: predominantly inattentive, predominantly hyperactive/impulsive, and combined. Researchers suggest these behavioral categories may not fully capture the brain’s structural differences. Using MRI scans, they found that ADHD may map onto two biologically distinct subgroups, defined not by behavior checklists but by measurable differences in brain structure.
Two ADHD Brain Subtypes With Opposite Structures
Researchers analyzed brain scans from 135 children and adolescents with ADHD alongside 182 neurotypical peers, drawing data from the publicly available ADHD-200 dataset collected across five research sites. All participants were under 18 and right-handed. After filtering for data quality, the team used a machine-learning algorithm called HYDRA to group ADHD participants based on gray matter patterns relative to neurotypical controls.
Two distinct subgroups emerged. Children in the first showed increased gray matter relative to neurotypical peers across much of the brain. Children in the second showed the reverse: reduced gray matter across much of the brain. Both patterns were statistically significant once the groups were separated.
Equally telling was what happened before the split. When researchers analyzed all 135 children with ADHD as a single group, no significant brain differences appeared compared to neurotypical peers at all. Only after dividing participants into the two subgroups did the opposing patterns become visible. Grouping all children with ADHD together effectively canceled out the signal, which may help explain why brain imaging studies of ADHD have produced inconsistent results for years.
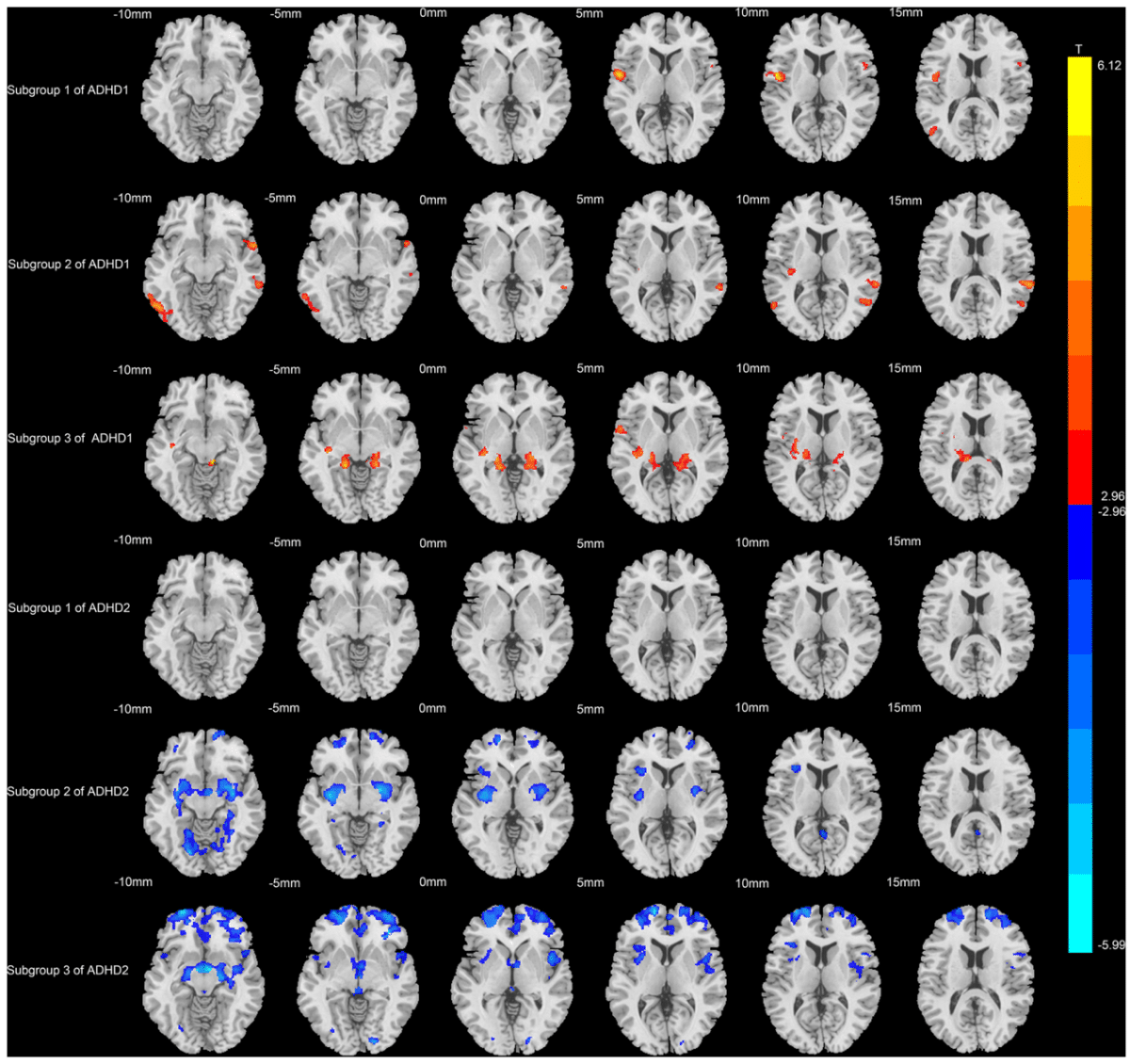
What Each Subtype Looks Like in the Brain
Children in subtype 1, the group with higher gray matter, showed symptoms most closely linked to inattentiveness. The brain changes clustered in two areas: the frontal lobes and the cerebellum. Frontal lobes help regulate attention and impulse control. The cerebellum, which most people associate with balance and coordination, has increasingly been recognized as a key player in attention processing. As symptom severity increased within this group, gray matter gains spread further into the cerebellum on top of changes already present in the frontal, parietal, and temporal regions.
Subtype 2 showed the opposite overall pattern. Gray matter losses were concentrated in the cerebellum, hippocampus, and other regions tied to memory, motivation, and emotional regulation. Most people know the hippocampus as a memory structure, but it also helps regulate motivation and emotion, two areas frequently disrupted in ADHD. In the earliest severity stage, children in this subtype showed no detectable brain differences from neurotypical peers. It was only in the moderate and severe stages that gray matter losses became apparent across the cerebellum, frontal regions, and hippocampus. Symptoms in this subtype covered the full ADHD picture, including inattention, hyperactivity, and impulsivity.
As the authors stated, “ADHD subtype 1 was closely associated with inattentiveness, involving prominent nodes,” meaning brain regions with outsized influence, “in the frontal regions and cerebellum,” while subtype 2 was “more strongly linked to overall disease severity, with the cerebellum and hippocampus as primary hubs.”
What These Findings Could Mean for Treatment
Perhaps the most consequential question raised by this research is whether the two subgroups might respond differently to treatment. Children in subtype 1, whose brain changes center on frontal and cerebellar regions tied to attention, might potentially benefit from cognitive training programs targeting attention networks. Children in subtype 2, who show more widespread brain changes and a broader symptom burden, might require more intensive approaches combining medication and behavioral therapy.
These are hypotheses, not prescriptions. The study did not test treatments or track how children responded to any intervention, and the researchers frame subtype-specific treatment as a direction for future investigation rather than a clinical recommendation. What the findings do offer is a neurological basis for something many parents and clinicians have observed in practice: two children with the same diagnosis can respond very differently to the same treatment.
ADHD affects an estimated 7.6% of children globally, and its diagnosis remains entirely behavioral, based on observed symptoms rather than any biological marker or brain scan. A single ADHD diagnosis may include multiple neurological patterns, and studies like this one are early steps toward understanding what those differences actually look like and what they might mean for the children living with them.
Disclaimer: This article is based on a single observational study and should not be interpreted as medical advice. The subgroups described are research clusters identified in one dataset, not clinically recognized ADHD categories. Consult a qualified healthcare professional for questions about ADHD diagnosis or treatment.
Paper Notes
Study Limitations
Several limitations bear on how broadly these findings can be applied. Because the study’s progression model works by ordering brain scans according to symptom severity scores rather than tracking individual children over time, it may not accurately reflect how ADHD actually develops in any given patient. The severity score used to rank participants may not fully capture the disorder’s breadth. Reliance on cross-sectional data means the study offers only a single snapshot of brain structure at one point in time. Longitudinal studies following the same children across years will be necessary to confirm whether these structural differences are stable, progressive, or responsive to treatment.
Funding and Disclosures
Funding was provided by the Department of Science and Technology of Shandong Province, the Natural Science Foundation of Shandong Province (grant ZR2023QH109), and the Taishan Scholars Program of Shandong Province (TS201712065). No competing interests were declared. Ethics approval was granted by the Institutional Review Board of Shandong First Medical University (No. 2025-H034), in accordance with the Declaration of Helsinki. All brain imaging data were drawn from the publicly available ADHD-200 dataset.
Publication Details
Authors Tianzheng Zhong and Feng Wang are affiliated with the Department of Radiology at the Second Affiliated Hospital of Shandong First Medical University in Tai’an, Shandong, China. Jianfeng Qiu is with the School of Radiology at Shandong First Medical University in Jinan, Shandong, China. Weizhao Lu, also of the Department of Radiology, served as guarantor and corresponding author. The paper, “Brain morphological changes across behaviour spectrums in attention-deficit/hyperactivity disorder,” was published in General Psychiatry in 2025. DOI: 10.1136/gpsych-2025-102340.







