
(© Yakobchuk Olena - stock.adobe.com)
KOBE, Japan — In a groundbreaking procedure, scientists have successfully used stem cells to treat a difficult-to-repair eye condition that could cause serious vision problems. The research, conducted on monkeys, focused on macular holes — a condition that can cause distorted or blurry central vision and even blind spots. This successful transplant could soon pave the way for future eye procedures involving human patients losing their sight.
Macular holes occur when the central part of the retina, called the macula, develops a break or tear. While many cases can be treated with surgery, some patients experience recurring holes or those that are resistant to standard treatments. For these challenging cases, researchers have been exploring innovative approaches, including the use of stem cells.
The study, published in the journal Stem Cell Reports, details how Japanese scientists used human embryonic stem cells to create retinal tissue in the lab. They then transplanted this lab-grown retinal tissue into the eye of a monkey with a macular hole. The results were promising: the transplanted tissue successfully filled the hole and showed signs of developing into functional retinal cells.
“We confirmed for the first time in a non-human primate model that embryonic stem-derived retinal organoid sheet transplantation facilitates the closure of macular holes,” says senior study author Michiko Mandai of the Kobe City Eye Hospital in a media release. “Our results suggest that this method could become a practical, safe, and effective treatment option with minimal invasive risks, particularly for difficult macular hole cases.”
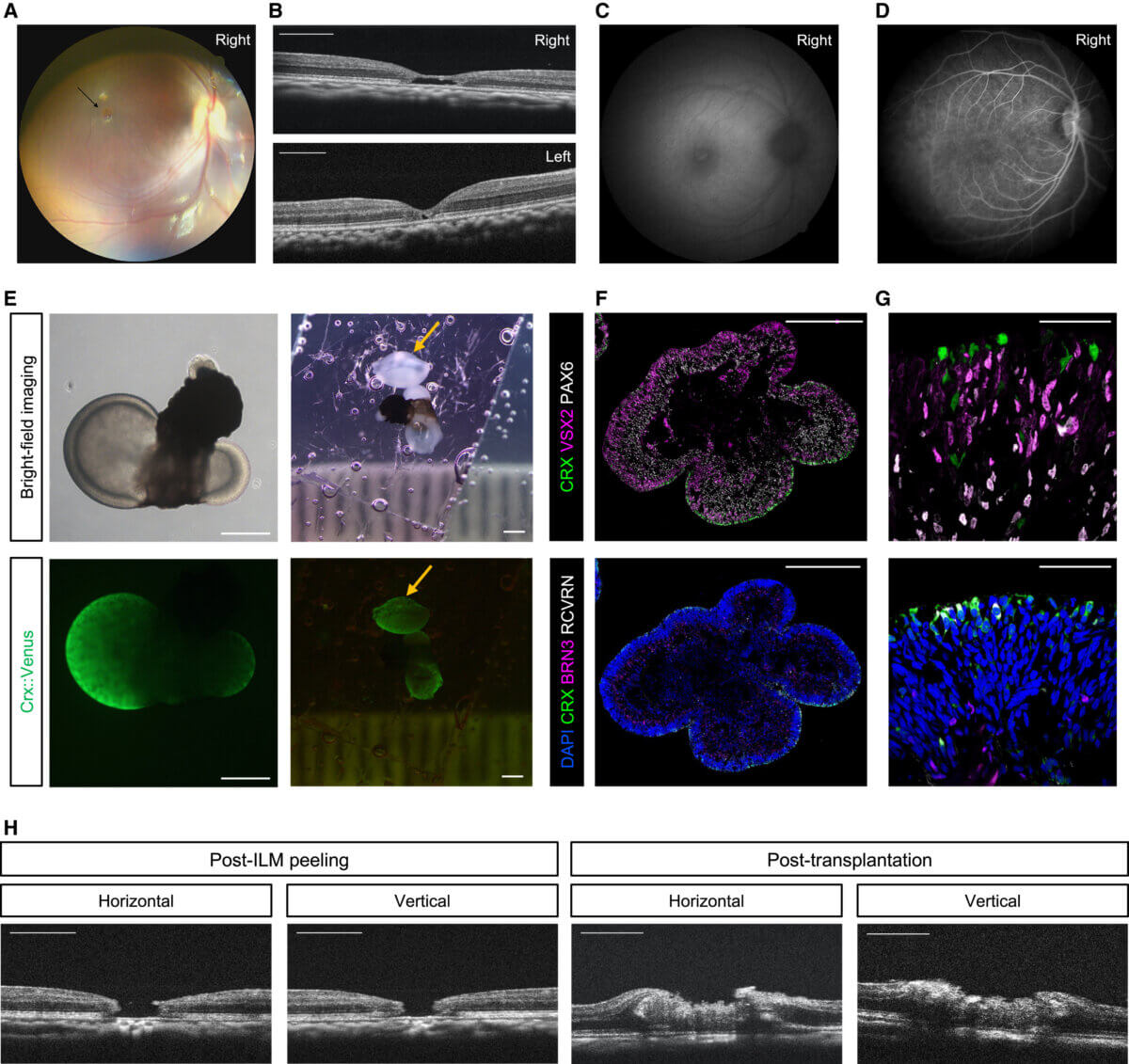
What makes this approach particularly exciting is its potential to overcome the limitations of current treatments. Unlike some existing techniques that use the patient’s own retinal tissue from other parts of the eye, this stem cell method doesn’t require sacrificing healthy retinal tissue. This could mean preserving more of the patient’s peripheral vision.
The researchers observed the monkey’s progress for seven months after the transplantation. They found that the stem cell-derived tissue not only filled the hole but also began to develop into various types of retinal cells, including the light-sensitive photoreceptors crucial for vision.
Perhaps most encouragingly, the monkey showed signs of improved visual function. Through a series of eye tests, the researchers noted that the animal’s ability to focus on targets improved significantly after the treatment. While it’s important to note that this is just one case and human trials are still necessary, the results offer hope for those suffering from persistent macular holes.
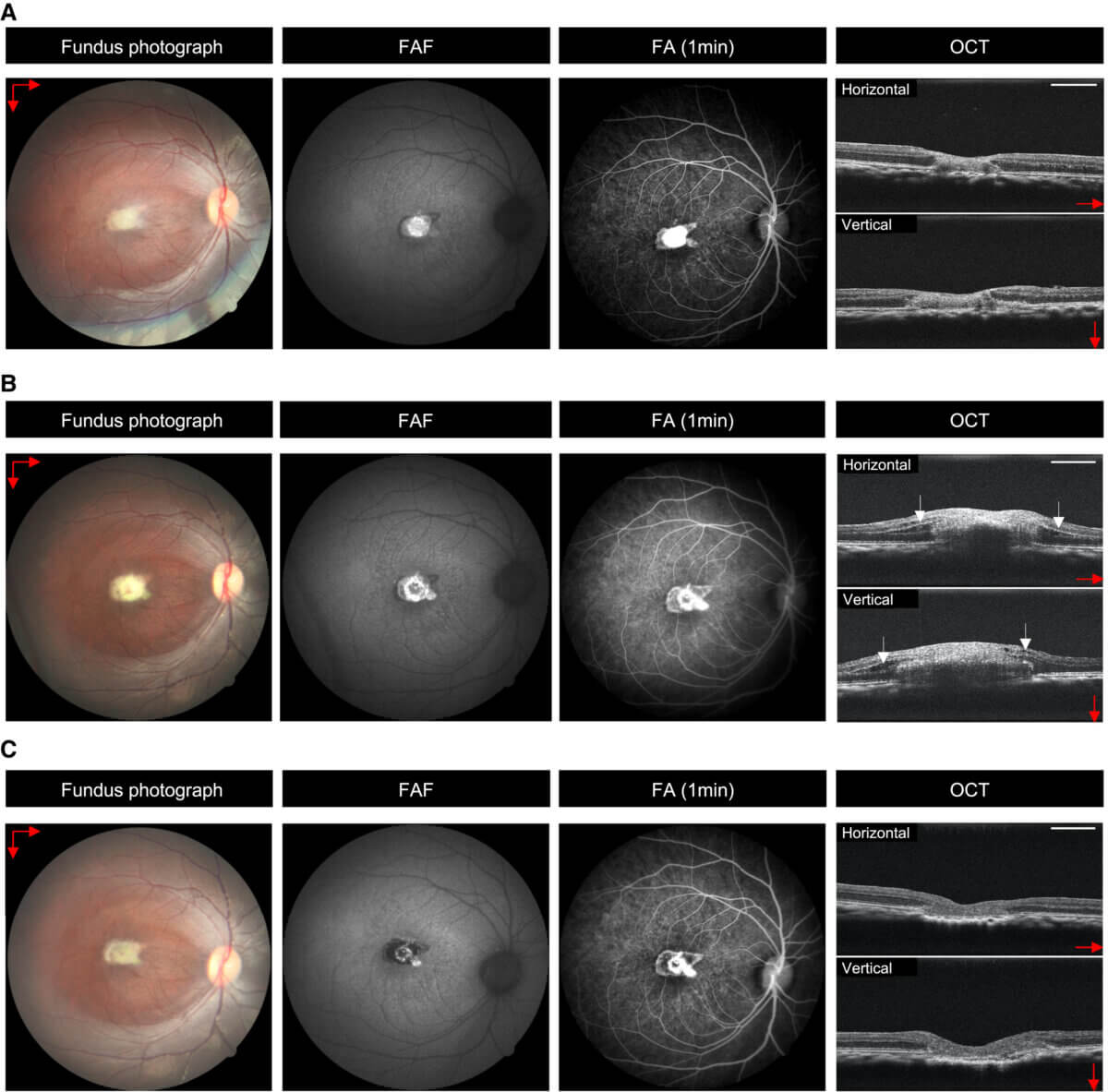
This research represents a significant step forward in the field of regenerative medicine for eye conditions. Demonstrating that lab-grown retinal tissue can successfully integrate into the eye and potentially improve vision opens up new possibilities for treating not just macular holes but potentially other retinal disorders as well.
However, the path from successful animal studies to human treatments is often long and complex. The researchers noted some challenges, including a mild rejection response to the transplanted tissue. While this was controlled with medication, it highlights the need for further refinement of the technique before it can be considered for human trials.
“The mild rejection may have limited the functional integration of the transplanted tissue,” Mandai concludes. “Additionally, this was a single-case result for one eye, and the model did not exactly replicate the pathology of human refractory macular holes. However, the findings suggest that the surgical technique is feasible for human macular holes.”
Paper Summary
Methodology
The researchers first created retinal tissue from human embryonic stem cells in the laboratory. They then surgically transplanted this tissue into the eye of a monkey that had a macular hole. The monkey’s vision was tested before and after the procedure using eye-tracking tests and electrical recordings of retinal activity. The researchers also performed detailed microscopic examinations of the eye tissue after the study period to see how well the transplanted cells had integrated and developed.
Key Results
The transplanted tissue successfully filled the macular hole and showed signs of developing into various types of retinal cells, including photoreceptors. The monkey’s ability to focus on visual targets improved significantly after the treatment. Electrical recordings showed increased retinal activity in the treated area. However, there was a mild rejection response to the transplanted tissue, which was controlled with medication.
Study Limitations
This study was performed on only one monkey, so the results need to be replicated in larger studies. The follow-up period was relatively short at seven months, so longer-term effects are unknown. The use of human embryonic stem cells may raise ethical concerns for some. There was a mild rejection response, indicating that immune suppression might be necessary for this treatment.
Discussion & Takeaways
The successful integration of lab-grown retinal tissue and the improvement in visual function are very promising. This approach could potentially overcome limitations of current treatments for macular holes, particularly for difficult cases. The development of different retinal cell types in the transplanted tissue suggests this method could have applications beyond just macular holes. However, more research is needed to refine the technique, address the immune response, and ensure long-term safety before human trials can begin.
Funding & Disclosures
The study was supported by several Japanese research institutions and government agencies, including the Japan Agency for Medical Research and Development and the Japan Science and Technology Agency. The researchers declared no competing interests related to this study.







