(Image by Shutterstock AI Image Generator)
In A Nutshell
- Human brain tissue has been found to contain far more microplastics than other organs, with the highest levels in people diagnosed with dementia.
- Ultra-processed foods, which make up more than half of calories consumed in the United States, are a major delivery vehicle for these plastic particles.
- A blood-filtering medical procedure shows early promise as a way to remove microplastics from the body, but scientists say more measurement tools are needed before it can be confirmed to work.
A plastic spoon’s worth of tiny fragments, quietly accumulating inside the human brain. That image is no longer science fiction, it’s where a new scientific perspective begins, and it argues that the growing buildup of plastics in the human body is one of the most pressing brain health questions of the moment.
Prior research found that brain tissue from deceased donors contained concentrations of microplastics anywhere from seven to thirty times higher than what was found in their liver or kidney tissue. The brain may be the organ most saturated with this pollution. That burden grew by roughly 50% between 2016 and 2024, according to the same research. Donors who had been diagnosed with dementia carried the heaviest load of all.
A new scientific perspective published in the journal BrainHealth is pulling together what researchers know, what they still can’t measure, and what needs to happen next. A particular emphasis was placed on pregnant women, children, and people already living with brain or heart disease. The authors argue that the combination of high plastic levels in brain tissue, scientifically credible explanations for how those plastics cause harm, and a clear dietary source that most Americans consume daily makes this a brain health concern deserving urgent attention.
A Brain Saturated With Microplastics
Science has confirmed that microplastics and their even tinier counterparts, nanoplastics, have turned up in human blood, in the placenta during pregnancy, inside the fatty deposits that clog arteries, and in brain tissue. Plastic particles found in arterial deposits were associated with a roughly fourfold increase in the combined risk of heart attack, stroke, or death over a follow-up period of thirty-four weeks, according to research cited in the perspective. Since stroke is a brain event, the authors note that this finding carries direct relevance to brain health.
Why the brain accumulates so much more plastic than other organs may come down to size. In animal studies, nanoscale plastic particles crossed the brain’s protective filtering system, known as the blood-brain barrier, within two hours of being swallowed. Larger particles did not make it through. Only the smallest ones did. Once inside, how the brain clears them remains unknown.
The brain’s high fat content may also play a role in how these particles accumulate, though researchers note that this same quality makes the brain one of the hardest organs to test accurately for plastics. Measuring what’s actually in brain tissue, reliably and in a way the broader scientific community agrees on, remains an unsolved problem.
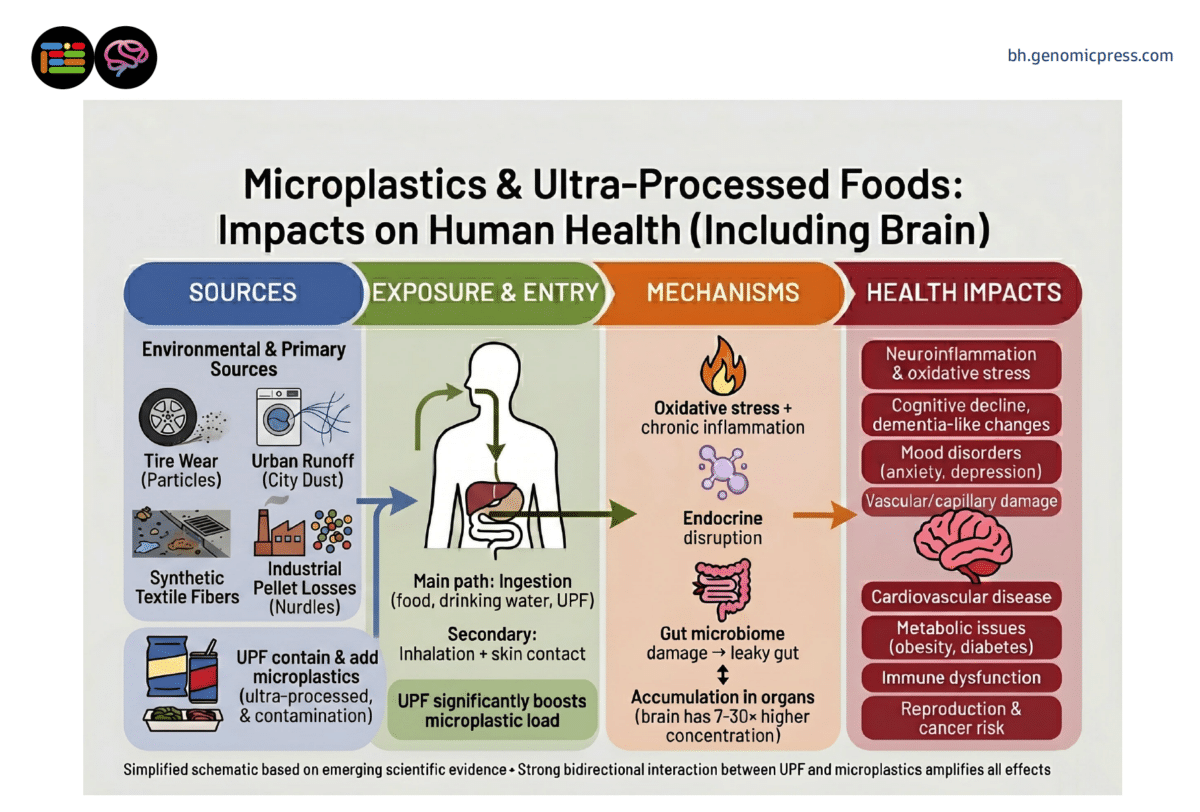
The Junk Food Connection to Microplastics in the Brain
This is where the story gets uncomfortably familiar for most American households. Ultra-processed foods (soft drinks, packaged snacks, instant noodles, mass-produced bread, and ready-to-heat meals) now account for more than half of caloric intake in the United States. These are industrially manufactured products that barely resemble whole food ingredients. According to the perspective’s authors, they are one of the main ways plastic enters the human body.
Plastic-based packaging migrates into food during heating and storage. Industrial machinery used in processing causes plastic wear and contamination. By the time a packaged product reaches a consumer, it has had extensive contact with plastic at multiple stages. Whole foods encounter far less of it.
Evidence linking ultra-processed food to brain health problems comes from very large observational studies. One analysis of 385,541 participants found that higher consumption of ultra-processed food was associated with a 53% increase in the odds of common mental health disorder symptoms, a 44% increase for depression, and a 48% increase for anxiety. A separate large study using U.K. health data linked higher ultra-processed food consumption to an increased risk of dementia. Another study found that a 10% rise in ultra-processed food intake was associated with a 16% increase in the risk of thinking and memory problems and an 8% increase in stroke risk, and those associations held even after accounting for whether people followed well-regarded healthy eating patterns like the Mediterranean or DASH diets.
The authors are careful to note that ultra-processed foods are harmful for multiple reasons, including poor nutrition, food additives, and refined oils. But they argue that plastic content is one of the few candidate mechanisms that explains why ultra-processed food keeps showing up as a risk factor even when traditional nutritional measures are accounted for. These are observational findings, and they cannot on their own establish that plastics are causing the observed harms, but the authors view the pattern as worth taking seriously.
Can Plastic Be Removed From the Body?
Within the past year, a research group reported that a procedure called therapeutic apheresis (a clinical technique that filters a patient’s blood plasma outside the body, similar to dialysis) was able to extract material consistent with microplastic particles from human plasma. This was described as the first credible demonstration that an existing medical procedure might be able to engage these particles inside a living person.
Infrastructure for this procedure already exists at major medical centers around the world. The biological rationale is sound. But the authors are measured in their optimism. Without validated tools that can confirm how much plastic is actually being removed from plasma and tissue, and whether reducing plastic in the blood translates to less plastic in the brain, the signal from apheresis remains promising but preliminary.
There’s also the question of scale. This kind of procedure is resource-intensive and cannot realistically be made available to entire populations. People most at risk (pregnant women, children, workers with high exposure to plastics on the job, and patients already dealing with brain or heart disease) need solutions that reach them in everyday life, not just in specialized hospital settings.

The Populations Who Can’t Wait
The perspective pays particular attention to groups facing compounded risk. Microplastics have been detected inside the placenta, the organ that sustains a developing baby, suggesting that exposure begins before birth, during the most sensitive window of brain development. Children face a longer lifetime of accumulation than adults and take in more plastic relative to their body weight. Workers in plastics manufacturing, recycling, textile production, and construction face high daily inhalation exposure and represent, in the authors’ view, an underutilized opportunity to study how dose relates to harm.
For patients already in neurological and cardiovascular care, the question the perspective raises is pointed: in people with dementia who show disproportionately high brain plastic loads, are those particles an innocent bystander, something that speeds up damage already underway, or an actual contributor to the disease? The authors do not claim to have the answer.
Three priorities emerge from the evidence. Standardized, reproducible methods for measuring plastic in brain tissue and in accessible biological samples are needed: without that, nothing else can be confirmed. Research also needs to move beyond general plastic toxicology and toward understanding which specific types of plastic, at which sizes, in which tissue cause which kinds of harm. Finally, removal strategies need to be tested against brain-relevant biological markers, with the apheresis finding as the anchor for a broader range of approaches.
For now, the one lever available at population scale, before any clinical removal method is validated, is cutting back on ultra-processed food consumption. The authors acknowledge this is not a simple ask, and that the science linking diet, plastics, and brain harm is still developing. But they argue it is the most actionable step currently available that matches the scale of the problem.
Brain plastic burden increased by approximately 50% in just eight years. If that pace continues, the consequences for population-level brain health could be substantial across generations. Researchers, clinicians, and public health officials are left with an urgent and still-unanswered question: what gets done about it before the numbers keep climbing?
Disclaimer: This article is for informational purposes only and is not medical advice. The findings described are based on a scientific perspective paper that synthesizes existing research, including animal studies and large observational studies in humans; they do not establish that microplastics directly cause the health outcomes discussed. Always consult a qualified healthcare professional before making any changes to your diet, supplements, or medical care.
Paper Notes
Limitations
The authors are transparent about substantial gaps in the current science. Validated, reproducible methods for measuring microplastics in brain tissue do not yet exist at a level the broader scientific community accepts as a gold standard. Different laboratories use different techniques and get different results. Brain tissue is particularly difficult to analyze because of its high fat content, which interferes with processing methods, and because contamination from blood vessels in post-mortem samples is difficult to rule out. It is also unknown whether regional differences within the brain are significant — whether a measurement from one area generalizes to deeper structures. The relationship between plastic levels in the blood and plastic levels in the brain has not been established, meaning that blood-based removal procedures cannot yet be confirmed to reduce brain burden. The perspective also notes that the apheresis findings are preliminary and cannot be considered confirmed without the measurement standards that don’t yet exist. The authors emphasize throughout that the field is operating ahead of its own analytical tools.
Funding and Disclosures
The paper does not report specific external funding sources. One author, Stefan R. Bornstein, is disclosed as serving on the Scientific Advisory Board of Ayus Medical Devices. All other authors declared no conflicts of interest related to this manuscript.
Publication Details
Authors: Julio Licinio, Charlotte Steenblock, Nicholas Fabiano, Stefan R. Bornstein, and Ma-Li Wong | Affiliations: GenomicPress, New York, New York; Department of Internal Medicine III, University Hospital Carl Gustav Carus, Technische Universität Dresden, Germany; University of Ottawa, Department of Psychiatry, Ottawa, Ontario, Canada; School of Cardiovascular and Metabolic Medicine and Sciences, Faculty of Life Sciences & Medicine, King’s College London, UK; Department of Endocrinology, Diabetology and Clinical Nutrition, University Hospital Zurich and University of Zurich, Switzerland | Journal: BrainHealth (GenomicPress) | Article Type: Perspective | Title: “The human microplastic burden and brain health: From measurement to pathophysiology and removal” | DOI: 10.61373/bh026p.0006 | Published online: May 5, 2026







