Credit: KK Stock on Shutterstock
In A Nutshell
- A new animal study found that SNAC, the absorption-boosting additive in Rybelsus (oral semaglutide), was linked to significant reductions in gut bacteria associated with fiber fermentation and metabolic health after 21 days of daily dosing.
- SNAC-treated rats showed a 70% spike in a key inflammation marker and a 77% drop in butyrate, a fatty acid critical to colon health and gut barrier function.
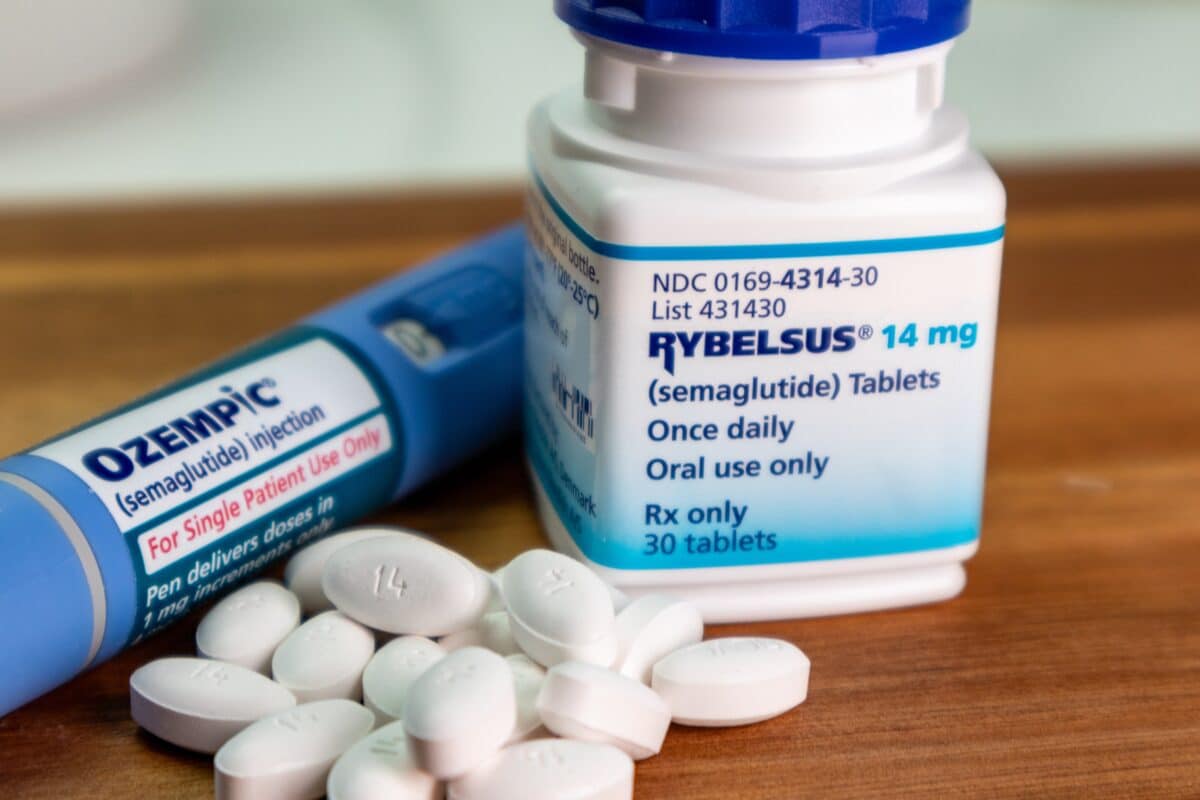
- The pill form of semaglutide, Rybelsus, is the only version of the drug that contains SNAC: injectable forms like Ozempic and Wegovy do not.
- Researchers stress that findings are associative, based on healthy rats over three weeks, and do not prove SNAC causes gut damage in people.
Semaglutide is a hot topic in weight loss these days, but concerning research suggests the pill form of this supposed weight loss wonder drug may hold unseen consequences for gut health.
Within three weeks of daily dosing, a chemical additive found in the pill form of semaglutide significantly reduced populations of gut bacteria associated with fiber fermentation and metabolic health in laboratory rats. Additionally, a cascade of inflammatory and metabolic changes were also seen that researchers say warrant a much closer look. The additive isn’t semaglutide itself, the active compound behind Ozempic, Wegovy, and Rybelsus. It’s salcaprozate sodium, known as SNAC, and it’s only found in Rybelsus, the oral pill version.
Published in the Journal of Controlled Release, the paper is the first to examine what daily SNAC exposure does to the gut microbiome in a living animal. The authors are careful to note that the findings are associative, not causal. Thus, the study cannot determine whether these changes would occur in people or persist with longer use.
Semaglutide is a large, fragile molecule. Stomach enzymes would normally destroy it before it could reach the bloodstream, and the gut wall blocks most of what survives. SNAC gets around both problems by temporarily altering the stomach lining’s permeability just enough for a sliver of the drug to slip through. Less than one percent of each dose makes it into circulation. The remaining SNAC travels unabsorbed into the small intestine and colon, regions densely populated by bacteria that govern metabolism, immunity, and brain health. What happens there has never been formally studied. This paper is a first attempt.
The “Safe” Label That Wasn’t Designed With the Microbiome in Mind
SNAC carries a “Generally Recognized As Safe” designation from the FDA and is used in a prescription vitamin B12 supplement. But the paper notes that SNAC’s mechanism of action remains a topic of scientific debate, and that existing safety designations may not have accounted for chronic daily exposure and its potential effects on the gut microbiome. Rybelsus patients take it every morning, potentially for years. No prior study had asked what that sustained exposure does to gut bacteria.
Researchers split 24 healthy male rats into four groups, dosing them daily for 21 days: semaglutide alone, SNAC alone, both compounds together in the same ratio used in Rybelsus, or a saline control. They tracked gut bacteria before and after, measured fermentation byproducts, tested blood for inflammation markers, and weighed organs at the study’s close.
Overall bacterial diversity held steady across all groups. But which specific bacterial families remained told a different story.
SNAC-treated animals showed a pronounced reshuffling of microbial communities that didn’t appear in animals given semaglutide alone. Two bacterial families associated with fiber fermentation and short-chain fatty acid production, Muribaculaceae and Bacteroidaceae, were reduced by 62 and 77 percent, respectively. Simultaneously, Desulfovibrionaceae, a group associated with inflammatory gut conditions, expanded seven-fold. Prior research has linked the hydrogen sulfide this group produces to intestinal barrier disruption, though the current study did not directly measure barrier damage.
A Chain of Changes, With Important Caveats
Muribaculaceae and Bacteroidaceae ferment dietary fiber and convert it into butyrate, a fatty acid that serves as the primary fuel for the cells lining the colon and helps maintain gut barrier integrity. Butyrate dropped 77 percent in SNAC-only animals and 75 percent in those receiving both compounds. Lower butyrate levels are associated with weaker barrier function, though this study did not directly test intestinal permeability or perform tissue biopsies to confirm structural damage.
Blood tests added to the picture. SNAC-only rats showed a 70 percent increase in tumor necrosis factor-alpha, a marker of systemic inflammation tied to insulin resistance and cardiovascular risk. Animals receiving both compounds showed a 25 percent rise in interleukin-6, another inflammation marker, alongside an 85 percent drop in brain-derived neurotrophic factor, a protein involved in brain signaling and metabolic regulation. In humans, lower levels of that protein have been associated with type 2 diabetes and obesity, though the study did not examine clinical outcomes or imply that SNAC would affect human patients the same way. Importantly, the study cannot determine whether the microbiome shifts caused these inflammatory changes, or whether both were driven by some other factor.
Only SNAC monotherapy significantly changed organ weights. SNAC-treated rats had livers roughly 13 percent heavier than control animals and cecums about 30 percent lighter, a pattern the authors say is consistent with reduced fermentation activity and lower butyrate. Semaglutide-only animals did not show significant organ weight changes, though the combination group did show elevated inflammation markers and reduced brain-derived neurotrophic factor.
“These findings indicate that SNAC-based therapies, even without altering overall microbial diversity, can suppress family-level taxa central to short-chain fatty acid production and create conditions that favour the growth of less beneficial taxa,” the authors wrote.
What It Means and What It Doesn’t
Gastrointestinal side effects remain the leading reason people stop taking oral semaglutide. Post-market drug safety data cited in the paper found a higher reporting odds ratio for GI disorders, including pancreatitis, with oral semaglutide than with the injectable forms, which contain no SNAC. That correlation does not prove SNAC is the cause, and the current study does not establish that either.
To be clear about what this research does and doesn’t show: it documents associations in healthy young male rats over the course of 21 days. It does not demonstrate that SNAC causes gut damage in people, nor does it establish that these changes would persist with longer use or translate to the metabolically compromised patients who actually take the drug. No endotoxin levels were measured, no permeability tests were run, and semaglutide plasma levels in the treated rats fell below detectable limits.
What it does establish is that the ingredient making Rybelsus possible has been traveling the full length of patients’ digestive tracts every day, largely unexamined. For the millions taking this pill, this study is less a warning than an overdue question.
Disclaimer: This article is based on preclinical animal research and should not be interpreted as medical advice. The findings reflect associations observed in healthy male rats over a 21-day period and have not been replicated in humans. Anyone taking oral semaglutide or any GLP-1 medication should consult their physician before making any changes to their treatment.
Paper Notes
Study Limitations
This study used healthy young male rats rather than animals modeling obesity or type 2 diabetes, limiting direct translation to patient populations. The 21-day window captures early microbiota changes but cannot determine whether effects persist, worsen, or reverse with longer treatment or after stopping. Using only male animals excludes potential sex-based differences in microbiota response. No intestinal permeability testing, tissue biopsies, or endotoxin measurements were performed, so barrier and organ changes cannot be confirmed at the cellular level. Bacterial enzyme activity was inferred computationally rather than measured directly. Pharmacokinetic data on intestinal SNAC concentrations were not collected, and semaglutide plasma levels fell below detectable limits in treated animals.
Funding and Disclosures
Supported by The Hospital Research Foundation (THRF), grant number 2022-CF-EMCR-004-25314. Authors declared no competing financial interests.
Publication Details
Authors: Amin Ariaee, Karim Noueihad, Alex Hunter, Anthony Wignall, Hannah R. Wardill, Maya Davies, Clive A. Prestidge, Paul Joyce — University of South Australia; Wardill and Davies also affiliated with the University of Adelaide and the South Australian Health and Medical Research Institute. | Journal: Journal of Controlled Release, Volume 392, 2026, Article 114711 | Title: “Gut microbiota perturbation and systemic inflammation are associated with salcaprozate sodium (SNAC)-enabled oral semaglutide delivery” | DOI: https://doi.org/10.1016/j.jconrel.2026.114711 | Published online: February 9, 2026







