Multiple sclerosis nerve disorder and damaged myelin (© freshidea - stock.adobe.com)
ST. LOUIS — In an unexpected twist that has researchers scratching their heads, a recent study suggests that people diagnosed with multiple sclerosis (MS) may have more protection against developing Alzheimer’s disease. This surprising finding challenges previous assumptions about MS and opens up new avenues for understanding both conditions.
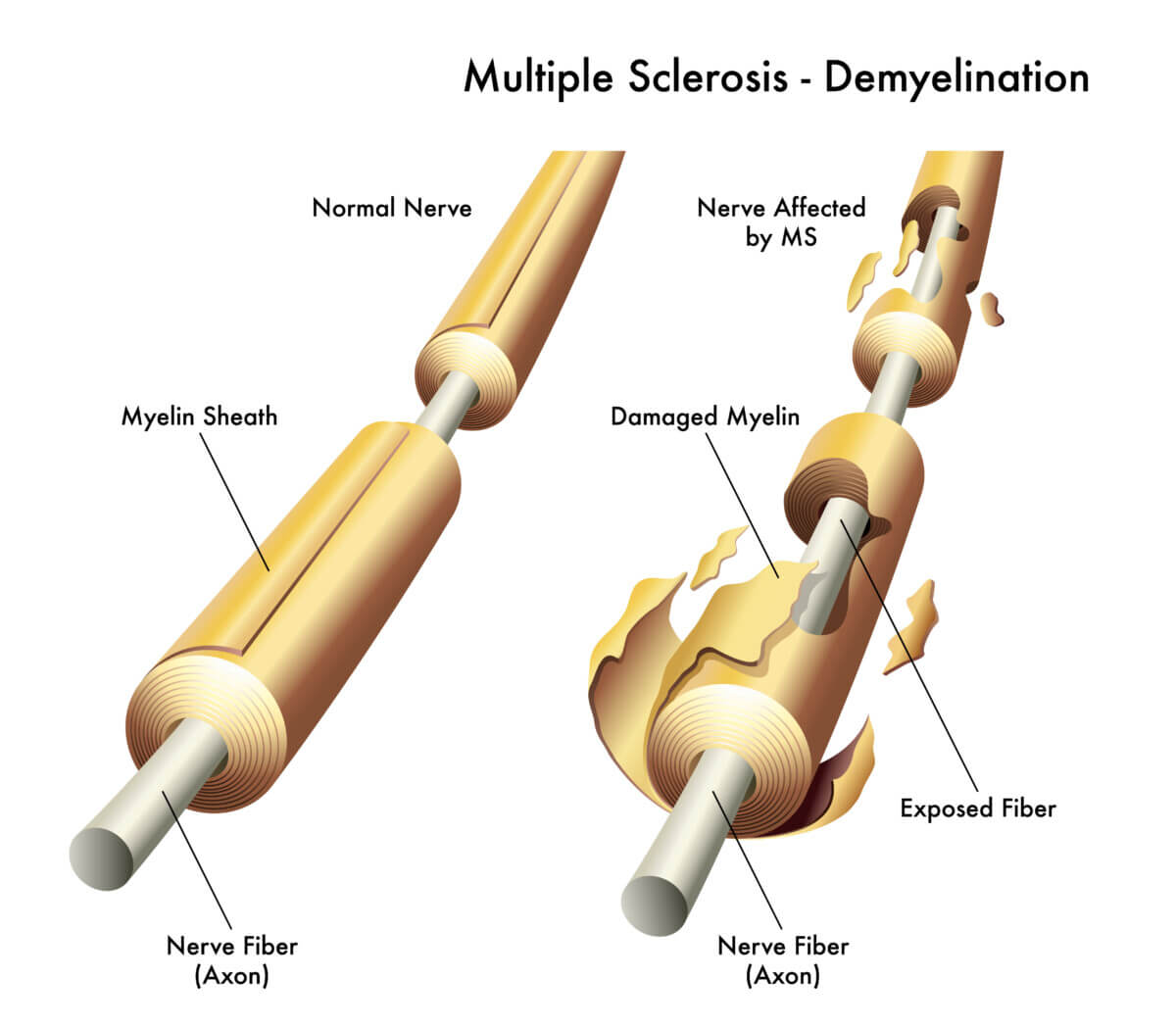
Multiple sclerosis is an autoimmune disease where the body’s immune system mistakenly attacks the protective covering of nerves in the brain and spinal cord. This can lead to a wide range of symptoms, from vision problems to difficulty with movement and balance. On the other hand, Alzheimer’s disease is a progressive brain disorder that slowly destroys memory and thinking skills, eventually affecting a person’s ability to carry out simple tasks.
For years, scientists believed that people with MS might be at higher risk for Alzheimer’s. The thinking was that the damage caused by MS could make the brain more vulnerable to the kind of changes seen in Alzheimer’s. However, this new research, published in the Annals of Neurology, turns that idea on its head.
“I noticed that I couldn’t find a single MS patient of mine who had typical Alzheimer’s disease,” says Anne Cross, MD, the Manny and Rosalyn Rosenthal and Dr. John Trotter MS Center Chair in Neuroimmunology, in a media release. “If they had cognitive problems, I would send them to the memory and aging specialists here at the School of Medicine for an Alzheimer’s assessment, and those doctors would always come back and tell me, ‘No, this is not due to Alzheimer’s disease.’”
The study, conducted by a team of researchers from Washington University School of Medicine in St. Louis, looked at the brains of people with MS after they had passed away. What they found was surprising: these brains had much less buildup of a protein called amyloid-beta than expected.
Amyloid-beta is a key player in Alzheimer’s disease. When it accumulates in the brain, it forms clumps or “plaques” that are a hallmark of the condition. Finding less of this protein in MS patients’ brains suggests that they might be less likely to develop Alzheimer’s.
“We found that 50% fewer MS patients had amyloid pathology compared to their matched peers based on this blood test,” says Matthew Brier, MD PhD, an assistant professor of neurology and radiology and the study’s first author.
This discovery is particularly intriguing because it goes against what we might expect. MS causes inflammation in the brain, and inflammation is generally thought to increase the risk of Alzheimer’s.
Why would MS patients show signs of being protected against Alzheimer’s?
The researchers have a few theories. One possibility is that the immune system changes triggered by MS might somehow help clear away amyloid-beta before it can build up. Another idea is that the medications used to treat MS might have a protective effect against Alzheimer’s.
If confirmed, these findings could have significant implications. They might lead to new ways of preventing or treating Alzheimer’s disease, inspired by what we learn from MS. It’s a reminder of how studying one disease can sometimes provide unexpected insights into another.
However, it’s important to note that this doesn’t mean people with MS are immune to Alzheimer’s or other forms of dementia. The study suggests a lower risk, not no risk at all. And MS itself can cause cognitive problems that might be mistaken for dementia.
Paper Summary
Methodology
The researchers examined brain tissue samples from 64 people with MS who had donated their brains to science after death. They compared these samples to brain tissues from people without MS. Using special staining techniques, they looked for the presence of amyloid-beta plaques, which are typically associated with Alzheimer’s disease. They also considered factors like age, sex, and genetic risk for Alzheimer’s to ensure a fair comparison.
Key Results
The study found that only about 5% of the MS patients had significant amyloid-beta buildup in their brains. This is much lower than what would be expected in a general population of similar age. Even in older MS patients, who would typically be at higher risk for Alzheimer’s, the rate of amyloid-beta pathology remained surprisingly low.
Study Limitations
One key limitation of this study is its relatively small sample size. While 64 brain samples provide valuable information, larger studies would be needed to confirm these findings. Additionally, the study looked at brain tissue after death, which doesn’t allow for tracking changes over time or assessing cognitive function in living patients.
Discussion & Takeaways
The researchers suggest that something about MS or its treatment might be protective against amyloid-beta accumulation. This could be due to changes in the immune system, effects of MS medications, or other factors not yet understood. The findings challenge the idea that brain inflammation always increases Alzheimer’s risk and suggest that the relationship between these diseases is more complex than previously thought.
These results open up new research directions. Future studies might investigate whether MS treatments could be repurposed to prevent or treat Alzheimer’s. They also highlight the need to better understand the role of the immune system in Alzheimer’s disease.
However, the researchers caution against over-interpreting these results. MS is a serious condition with its own set of challenges, and this study doesn’t suggest that having MS is beneficial overall. Instead, it provides a new perspective on the intricate workings of the brain and immune system.
Funding & Disclosures
The study was supported by grants from the National Institutes of Health, the National Multiple Sclerosis Society, and other research foundations. Some of the researchers disclosed receiving fees or grants from pharmaceutical companies, but these were not directly related to this study. As always in scientific research, it’s important to consider potential conflicts of interest, though there’s no indication that they influenced the results of this particular study.







