
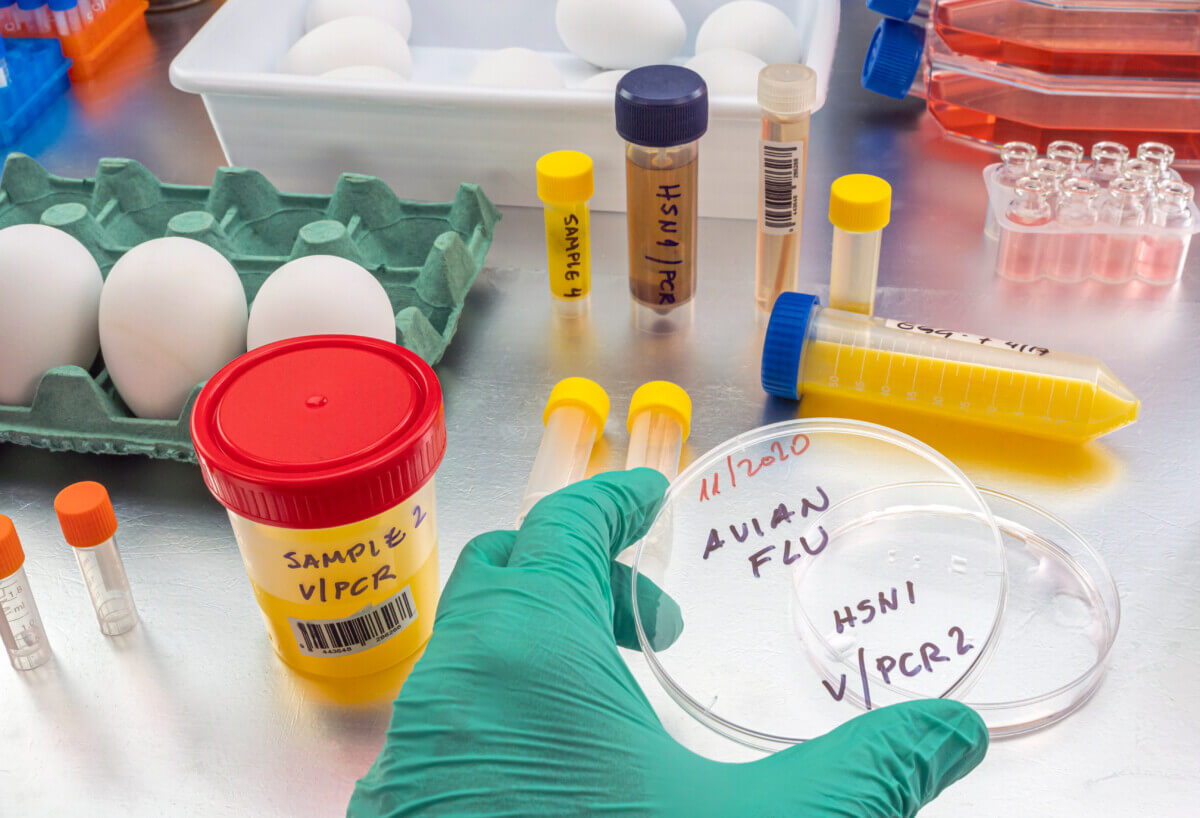
(Photo by Goksi on Shutterstock)
Nearly a third of pasteurized milk in U.S. stores likely contains remnants of the H5N1 virus.
In A Nutshell
- Up to 30% of U.S. pasteurized milk contains genetic fragments of H5N1 bird flu, but these fragments are not infectious and do not appear to harm consumers.
- Mouse experiments at St. Jude showed that repeated consumption of pasteurized milk spiked with inactivated H5N1 did not make animals more vulnerable to the virus later.
- Pasteurization kills the virus but preserves proteins, which raised concerns about possible immune side effects. The study found no evidence of harmful immune suppression or tolerance.
- Prior H1N1 flu exposure provided strong cross-protection against H5N1 in mice, highlighting the role of past infections and vaccinations.
- Bottom line: properly pasteurized milk poses minimal health risks, while raw or improperly pasteurized milk remains dangerous.
MEMPHIS — Up to 30% of the milk sitting in grocery store refrigerators across America contains genetic fragments of H5N1 bird flu virus. Federal health officials have known about widespread contamination since the virus jumped from birds to dairy cows in March 2024. What they didn’t know until now was whether drinking that milk day after day might harm people.
A new study from St. Jude Children’s Research Hospital delivers the first experimental answer to that question, and it’s reassuring. Researchers fed mice pasteurized milk spiked with H5N1 virus daily for five days, then exposed them to lethal doses of the virus. Mice that consumed contaminated milk fared just as well as those that never consumed it.
Pasteurization kills infectious viruses but leaves behind viral “ghosts,” or proteins and genetic material that persist in milk, testing negative for live virus. These molecular remnants raised questions about whether they might trigger harmful immune responses over time.
“We found that repeated oral exposure to inactivated HPAI H5N1 virus in milk did not cause morbidity or mortality in mice,” the researchers wrote in the paper, published in Science Advances. Simply put, drinking milk with viral fragments doesn’t appear to make animals sicker when they encounter the real virus later.

Why Heat Treatment Leaves Bird Flu Remnants Behind In Milk
Pasteurization has been the gold standard for milk safety since the early 1900s, designed to eliminate dangerous bacteria and viruses through controlled heating. The process works by heating milk to 72°C (about 162°F) for 15 seconds. This is hot enough to destroy most pathogens while preserving taste and nutrition.
H5N1 presents an unusual challenge. The virus’s outer shell contains a protein called hemagglutinin that helps it attach to and infect cells. When researchers heated H5N1 virus in regular salt water, this protein broke apart as expected. When they heated the same virus in milk, however, the protein remained largely intact.
Milk proteins and fats create a protective coating around viral particles during heating, shielding some components from complete destruction. Other studies have shown that milk can stabilize various viruses during heat treatment.
This protective effect means that even properly pasteurized milk can contain recognizable viral proteins. Using computer modeling, researchers confirmed that H5N1’s surface proteins would likely survive pasteurization in milk, much like seasonal flu viruses do.
Scientists Test Extreme Exposure Conditions
Research teams designed experiments to test extreme exposure conditions using bovine H5N1 virus isolated directly from infected Ohio cattle. They spiked milk with concentrations far higher than anything found in commercial products. Mice received daily doses equivalent to drinking heavily contaminated milk for a work week.
The virus strain proved remarkably lethal in laboratory conditions. Just 10 infectious particles were enough to kill half the mice exposed directly. When researchers accidentally used improperly pasteurized milk containing live virus, naive mice died quickly while those with previous flu immunity survived.
Mice that consumed properly pasteurized milk with inactivated virus showed no increased vulnerability. When exposed to lethal H5N1 doses weeks later, their survival rates matched those of animals that had never encountered contaminated milk.
Multiple validation methods confirmed complete viral elimination through proper pasteurization: growing viruses in cell cultures, testing chicken eggs for infection, and monitoring viral reproduction over extended periods. All approaches showed that heating milk to pasteurization temperatures completely eliminated infectious virus.
One of the biggest theoretical concerns about consuming viral proteins involves a process called oral tolerance. The digestive system normally learns to ignore harmless substances like food proteins to prevent unnecessary immune reactions. If this same process occurred with viral proteins, it could potentially weaken immune responses to future infections.
The study found no evidence of this happening. Mice that consumed viral proteins in milk developed normal immune responses when infected with live virus later. They produced appropriate antibody levels and fought off infection just as effectively as unexposed animals.
Researchers also tested whether viral protein consumption might boost immunity. Mice that drank pasteurized milk with inactivated virus showed no detectable antibody responses and no better protection than control animals when exposed to live virus.
The neutral response means viral proteins in pasteurized milk exist in a form that doesn’t activate immune recognition, possibly due to changes during heat treatment or interactions with milk components.
How Prior Flu Infection Provides Unexpected Protection
The study’s most notable discovery emerged from mice with previous flu immunity. Animals that had recovered from H1N1 infection weeks earlier remained completely protected against H5N1 exposure, regardless of whether they consumed contaminated milk.
This cross-protection persisted despite major genetic differences between the viruses. The seasonal H1N1 strain shared only 65% similarity with bovine H5N1 in key surface proteins, yet still offered complete protection against death.
The effect likely stems from antibodies targeting neuraminidase, a viral enzyme that differs from hemagglutinin. Previous studies have shown that neuraminidase antibodies generated by H1N1 infection can recognize H5N1 viruses and contribute to protection, even when surface proteins differ substantially.
For humans, this discovery means prior flu infections or vaccinations might provide some level of protection against H5N1, even through oral exposure. Most adults have been exposed to multiple flu strains over their lifetimes, creating a diverse antibody collection that could cross-react with H5N1.
What This Means For Milk Safety As Bird Flu Outbreaks Continue
Experimental conditions used viral concentrations much higher than those detected in commercial milk supplies. While up to 30% of pasteurized milk samples have tested positive for H5N1 genetic material, the levels are typically quite low, often just detectable traces rather than high concentrations.
“We found that consuming pasteurized milk multiple times, even if it has inactivated H5N1 virus, poses minimal health risks,” said corresponding author Stacey Schultz-Cherry, from the St. Jude Department of Host-Microbe Interactions, in a statement. “It’s reassuring to find that these inactivated H5N1 viral components in pasteurized milk present minimal health risks and don’t alter flu immunity. However, we also reaffirmed that consuming unpasteurized milk can expose people to this potentially dangerous infectious agent. We must continue to watch this virus and mitigate its risk of spilling over into the human population.”
Federal agencies continue monitoring milk supplies as the outbreak spreads among dairy herds. The virus has been detected in cattle across 17 states, with occasional spillover infections in farm workers who handle infected animals or contaminated milk.
Current surveillance focuses on ensuring proper pasteurization and detecting any viral changes that might affect heat sensitivity. Quality control measures remain critical because the research confirmed that improperly pasteurized milk containing live virus can cause infection, particularly in people without prior flu immunity.
Raw milk consumption carries significantly higher risks and remains strongly discouraged by health authorities. Unpasteurized milk from infected cows contains high levels of infectious virus that can survive for extended periods.
The research provides reassurance about one aspect of the H5N1 outbreak while highlighting the importance of existing food safety systems. Pasteurization protocols exist specifically to handle contamination events like this, and the study shows they’re working as designed.
For most consumers, the research suggests that properly pasteurized milk poses minimal health risks, even when it contains viral fragments from H5N1. The fragments themselves don’t appear to harm people who consume them repeatedly, and most adults likely have some level of pre-existing immunity that could offer additional protection.
Research teams emphasized that their discoveries depend entirely on proper pasteurization. Industrial-scale milk processing operates under strict temperature and timing controls, but equipment failures or inadequate heating could create risks. Continued monitoring and quality control remain essential as the outbreak evolves.
For now, your morning cereal and coffee remain safe, even if the milk contains molecular ghosts of one of the world’s most feared viruses.
Your Questions Answered
Q: Can I get bird flu from drinking milk?
A: Not if it’s pasteurized. The new study shows that heating milk to standard pasteurization levels completely inactivates H5N1 virus. While fragments of viral proteins and genetic material can remain, they are harmless and don’t make animals more vulnerable when exposed to the live virus latersciadv.aeb3906.
Q: Why are bird flu fragments showing up in milk at all?
A: H5N1 jumped from birds to dairy cows in 2024. Infected cows shed virus into their milk, which is why traces can be detected even after pasteurization. The heating process kills the virus but doesn’t always destroy all of its proteins, leaving behind harmless “ghosts.”
Q: Does this mean raw milk is dangerous?
A: Yes. Raw milk from infected cows can contain large amounts of live, infectious H5N1 virus that survives for days or weeks. Drinking it could pose a real health risk. That’s why public health officials strongly advise against consuming raw or unpasteurized milk.
Q: What about improperly pasteurized milk?
A: In the study, mice that drank milk that hadn’t been heated enough died quickly if the virus was still alive. Only those with prior flu immunity survived. This underscores why strict temperature and timing controls in industrial pasteurization are critical.
Q: Could drinking milk with viral fragments weaken my immune system?
A: The researchers tested this and found no evidence of harmful effects like “oral tolerance” — where the immune system learns to ignore a pathogen. Mice that consumed viral fragments developed normal immune responses when later infected with live H5N1sciadv.aeb3906.
Q: Could these fragments actually help build immunity, like a vaccine?
A: No. The study showed that viral proteins left in pasteurized milk didn’t boost protection or act like an oral vaccine. They were immunologically “neutral.”
Q: Does past flu exposure help against bird flu?
A: Surprisingly, yes. Mice that had already recovered from H1N1 flu were fully protected against H5N1, even without milk exposure. That protection likely comes from antibodies targeting a viral enzyme called neuraminidase, which shares similarities across flu strainssciadv.aeb3906.
Q: Should I be worried about drinking milk right now?
A: No — if it’s pasteurized. The study and federal monitoring both support that properly pasteurized milk poses minimal risk, even when viral fragments are detected. The real danger lies in raw or improperly treated milk.
Paper Summary
Methodology
Researchers tested H5N1 and H1N1 influenza virus inactivation using an in-house pasteurization protocol that heated milk samples to 72°C for 15-30 seconds. Male C57BL/6J mice were given daily oral doses of pasteurized milk containing inactivated virus for five days, then challenged with lethal viral infections. The team used multiple validation methods including cell culture assays, chicken egg infections, and extended viral growth monitoring to confirm complete viral inactivation. Some experiments included mice with prior H1N1 immunity to test cross-protection.
Results
Pasteurization completely eliminated infectious H1N1 and H5N1 virus in milk, reducing viral loads below detection limits. Viral proteins, particularly hemagglutinin, remained structurally intact after pasteurization in milk but not in salt water. Mice consuming pasteurized milk with inactivated virus showed no increased mortality or morbidity when challenged with lethal viral doses compared to control animals. Prior H1N1 immunity provided complete protection against H5N1 infection regardless of milk consumption. Accidental exposure to improperly pasteurized milk containing live virus caused death in naive mice but not those with prior immunity.
Limitations
The study used only male mice, potentially missing sex-specific responses. Sample sizes were limited for some experiments due to facility constraints and urgency of the research. The pasteurization protocol was conducted in-house rather than at industrial scale, which may not fully replicate commercial processing conditions. Testing focused on a single H5N1 strain and may not apply to all viral variants. The research cannot address long-term effects of repeated exposure over months or years.
Funding and Disclosures
This work was supported by the National Institute of Allergy and Infectious Diseases contract 75N93021C00016, the American Lebanese Syrian Associated Charities, and National Institutes of Health training grants T32AI106700-08 and F32AI183804. The authors declared no competing interests. All animal procedures were approved by St. Jude Children’s Research Hospital institutional committees.
Publication Information
Brigleb, P.H., et al. “Repeated oral exposure to H5N1 influenza virus in pasteurized milk does not cause adverse responses to subsequent influenza infection.” Science Advances, Vol. 11, Issue 39, September 26, 2025. DOI: 10.1126/sciadv.aeb3906.
Disclaimer: This article summarizes experimental findings in mice and should not be interpreted as direct proof of safety in humans. The study tested high-dose exposures under controlled laboratory conditions, and results may not capture long-term effects or all viral strains. Consumers should follow public health guidance: avoid raw milk and rely on properly pasteurized products.








Additionally, Bovine (cow) leukemia virus is readily found in cows milk (pasteurized as well as raw) and is clearly linked to breast cancer as well as other cancers. The milk of infected herds is mixed in large vats with other cow milk before treatment and bottling.
In cattle: BLV is widespread in cattle globally, with high prevalence rates in U.S. dairy herds.
In food products: Studies have detected BLV proviral DNA in milk and meat from infected animals.
In human tissues: BLV DNA has been found in human blood and is suspected of being linked to human cancers, particularly breast cancer.
University of California, Berkeley, researchers conducted a study published in September 2015 that established a link between bovine leukemia virus (BLV) and human breast cancer. They found that women with breast cancer were significantly more likely to have BLV DNA in their breast tissue.
Stronger odds ratio: The study reported an odds ratio of 3.07, meaning that the odds of having breast cancer among women with BLV in their breast tissue were over three times higher than among women without it. The researchers noted this figure is higher than many other known risk factors like alcohol consumption and obesity.