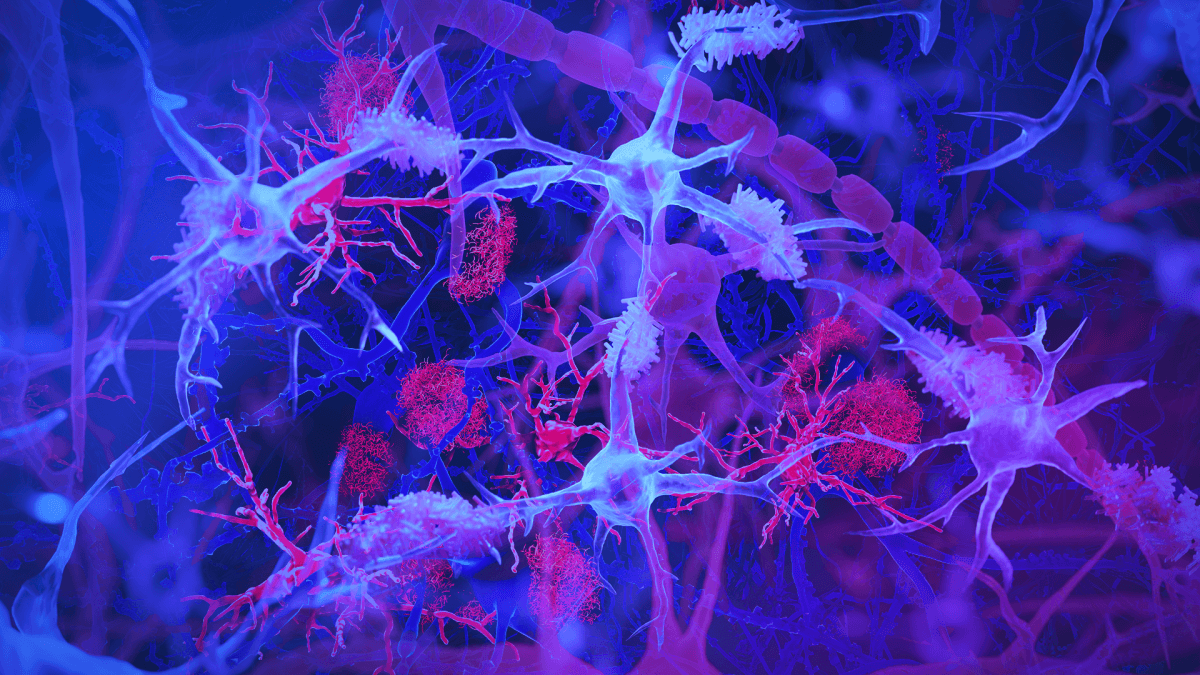
The brain's immune cells, or microglia (light blue/purple), are shown interacting with amyloid plaques (red) — harmful protein clumps linked to Alzheimer’s disease. The illustration highlights the microglia’s role in monitoring brain health and clearing debris. (Illustration by Jason Drees/Arizona State University)
TEMPE, Ariz. — In the gut of some Alzheimer’s patients lies an unexpected culprit: a common virus that may be silently contributing to their disease. While scientists have long suspected microbes might play a role in Alzheimer’s disease, new research has uncovered a surprising link between a virus that infects most humans and a distinct subtype of the devastating neurological condition.
The research suggests that human cytomegalovirus (HCMV) — a virus that infects between 80% of adults over 80 — may play a more significant role in Alzheimer’s disease than previously thought, particularly when combined with specific immune system responses.
The study, led by researchers at Arizona State University and multiple collaborating institutions, focused on a specific type of brain cell called microglia marked by a protein called CD83. These CD83-positive microglia were found in 47% of Alzheimer’s patients compared to 25% of unaffected individuals.
This study, published in the journal Alzheimer’s and Dementia, is particularly notable because it examines multiple body systems, including the gut, the vagus nerve (which connects the gut to the brain), and the brain itself. The researchers found that subjects with CD83-positive microglia in their brains were more likely to have both HCMV and increased levels of an antibody called immunoglobulin G4 (IgG4) in their colon, vagus nerve, and brain tissue.
“We think we found a biologically unique subtype of Alzheimer’s that may affect 25% to 45% of people with this disease,” says study co-author Dr. Ben Readhead, a research associate professor with ASU-Banner Neurodegenerative Disease Research Center, in a statement. “This subtype of Alzheimer’s includes the hallmark amyloid plaques and tau tangles—microscopic brain abnormalities used for diagnosis—and features a distinct biological profile of virus, antibodies and immune cells in the brain.”
For their research, the team examined tissue samples from multiple areas of the body in both Alzheimer’s patients and healthy controls. They found that patients with CD83-positive microglia in their brains were significantly more likely to have both HCMV and elevated IgG4 levels in their colon, vagus nerve, and brain tissue.
“It was critically important for us to have access to different tissues from the same individuals. That allowed us to piece the research together,” says Readhead, who also serves as the Edson Endowed Professor of Dementia Research at the center.
To further investigate the potential impact of HCMV on brain cells, the team conducted experiments using cerebral organoids – simplified versions of human brain tissue grown in the laboratory. When these organoids were infected with HCMV, they showed accelerated development of two key markers of Alzheimer’s disease: amyloid beta-42 and phosphorylated Tau-212. The infected organoids also showed increased rates of neuronal death.
The researchers emphasize that while HCMV infection is common, only a subset of individuals showed evidence of intestinal HCMV infection, which appears to be the relevant factor in the virus’s presence in the brain.
Study authors suggest that in some individuals, HCMV infection might trigger a cascade of events involving the immune system that could contribute to the development or progression of Alzheimer’s disease. This is particularly interesting because it might help explain why some people develop Alzheimer’s while others don’t, despite HCMV being so common in the general population.
Looking ahead, the research team is developing a blood test to identify individuals with chronic intestinal HCMV infection. They hope to use this in combination with emerging Alzheimer’s blood tests to evaluate whether existing antiviral drugs could be beneficial for this subtype of Alzheimer’s disease.
“We are extremely grateful to our research participants, colleagues, and supporters for the chance to advance this research in a way that none of us could have done on our own,” notes Dr. Eric Reiman, Executive Director of Banner Alzheimer’s Institute and the study’s senior author. “We’re excited about the chance to have researchers test our findings in ways that make a difference in the study, subtyping, treatment and prevention of Alzheimer’s disease.”
With the development of a blood test to identify patients with chronic HCMV infection on the horizon, this research might not just explain why some people develop Alzheimer’s – it might also point the way toward preventing it. In the end, the key to understanding this devastating brain disease may have been hiding in our gut all along.
Paper Summary
Methodology
The study employed a multi-pronged approach to investigation. Researchers analyzed tissue samples from multiple areas of the body (brain, gut, and vagus nerve) using immunohistochemistry to detect the presence of HCMV and IgG4. They also examined cerebrospinal fluid samples to look for specific antibodies against HCMV. Additionally, they used laboratory-grown brain organoids to study the direct effects of HCMV infection on brain cells. The study included samples from both Alzheimer’s patients and healthy controls, with findings validated in an independent cohort.
Key Results
The key findings showed that patients with CD83-positive microglia had significantly higher levels of both HCMV and IgG4 in multiple tissues. In the laboratory experiments, HCMV infection led to increased production of Alzheimer’s-associated proteins and increased cell death. The study found strong statistical associations between these various factors, suggesting a connected pathway from viral infection to disease progression.
Study Limitations
While the study shows strong associations, it cannot definitively prove that HCMV causes Alzheimer’s disease. The sample sizes, while adequate, could be larger in future studies. Additionally, the study cannot explain why some people with HCMV infection develop Alzheimer’s while others don’t, suggesting other factors are likely involved.
Discussion & Takeaways
The study suggests a potential new pathway in Alzheimer’s disease development involving viral infection and immune response. This could lead to new therapeutic approaches, particularly in patients showing specific biomarkers. The findings also highlight the importance of considering multiple body systems in disease research, rather than focusing solely on the brain.
Funding & Disclosures
The research was supported by various organizations, including the National Institute on Aging, the NIH, the Global Lyme Alliance, and the Arizona Alzheimer’s Consortium. The researchers disclosed several potential conflicts of interest: one author has served as a consultant for multiple pharmaceutical and therapeutic companies, including J&J, Diagenic, Pfizer, Cognito Therapeutics, and others. Additionally, four of the authors are listed as co-inventors on a patent application for an IgG4-based peripheral biomarker to detect CD83(+) microglia. The remaining authors declared no relevant conflicts of interest.
Publication Details
This research was published in Alzheimer’s & Dementia: The Journal of the Alzheimer’s Association on December 19, 2024. The study is titled “Alzheimer’s disease-associated CD83(+) microglia are linked with increased immunoglobulin G4 and human cytomegalovirus in the gut, vagal nerve, and brain” (DOI: 10.1002/alz.14401). was an experimental study using human tissue samples.







