
(Credit: dizain/Shutterstock)
PARKVILLE, Australia — Imagine a medical condition so severe that it can turn a simple rash into a life-threatening emergency. Toxic epidermal necrolysis (TEN) has been just such a nightmare for patients, with no effective treatment — until now.
In a landmark study published in the journal Nature, researchers have achieved the unthinkable: a potential cure for this rare but deadly skin disease. The breakthrough came from an international team that included scientists from the Max Planck Institute of Biochemistry and the Walter and Eliza Hall Institute of Medical Research (WEHI).
TEN is a rare condition typically triggered by severe reactions to common medications like gout treatments or over-the-counter antibiotics. With a mortality rate of around 30%, patients can quickly develop widespread skin blistering that requires intensive care, similar to treating burn victims.
The researchers’ approach was ingenious. Using an advanced technique called spatial proteomics, they created a detailed molecular map of the disease.
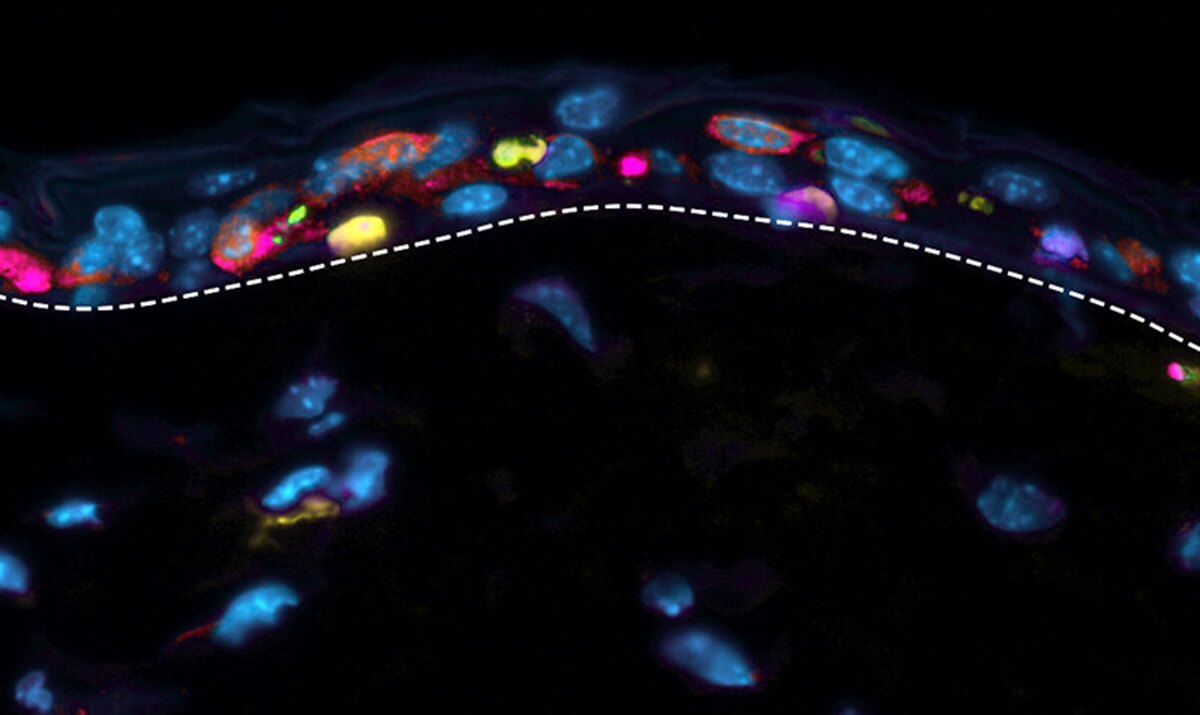
“By applying spatial proteomics to archived patient samples suffering from toxic epidermal necrolysis, we were able to precisely isolate and analyze individual cell types and understand what is actually occurring in the skin of these patients,” explains Dr. Thierry Nordmann, the study’s first author, in a media release.
They discovered a critical insight: a hyperactive inflammatory pathway in the body that drives the disease’s progression. This led them to test JAK inhibitors — drugs already approved for treating inflammatory conditions like rheumatoid arthritis — as a potential treatment.
The results were nothing short of miraculous. When the team administered JAK inhibitors to seven patients suffering from TEN, every single patient experienced rapid improvement and full recovery.
“Finding a cure for lethal diseases like this is the holy grail of medical research. I am beyond proud of this incredible research collaboration that has already helped to save the lives of multiple patients,” notes Dr. Holly Anderton, the study’s second author.
The researchers hope their findings will soon lead to clinical trials and regulatory approval, potentially transforming the treatment of this devastating disease. For patients with TEN, this breakthrough offers a ray of hope where once there was none.
Paper Summary
Methodology
The researchers employed a method called Deep Visual Proteomics (DVP). This technique allows scientists to look at proteins in specific types of cells from human tissue, even from preserved biopsy samples. They studied samples from patients with various drug-related skin reactions, focusing on keratinocytes (skin cells) and immune cells.
Using advanced imaging and artificial intelligence, they separated these cell types, extracted their proteins, and analyzed them. By doing this, they identified thousands of proteins and mapped changes linked to the severity of the skin conditions.
Key Results
The study found that a particular signaling pathway, the JAK/STAT pathway, was highly active in patients with toxic epidermal necrolysis (TEN), the most severe skin reaction studied. This pathway contributes to inflammation and skin damage. They tested drugs that block this pathway, called JAK inhibitors, in lab settings and on mice.
These drugs reduced the severity of the skin damage and sped up recovery. When used on seven patients with TEN, these inhibitors helped stop the disease progression and improved healing, with no significant side effects.
Study Limitations
The study included a small group of patients (seven) for testing the treatment. The mouse models and lab experiments may not fully replicate human TEN. Long-term safety and effectiveness of the JAK inhibitors need further exploration. The study focused on a specific subset of patients, so the findings may not apply to all cases of TEN or other drug-induced skin conditions.
Discussion & Takeaways
The study emphasizes the critical role of the JAK/STAT pathway in severe drug-induced skin conditions like TEN. Targeting this pathway with JAK inhibitors offers a potential treatment option that not only stops the disease from worsening but also promotes faster healing. This approach could transform how we treat TEN and similar conditions, moving away from general supportive care to targeted therapies.
For healthcare providers, this research provides a new understanding of the underlying mechanisms of TEN and highlights the importance of early intervention. For patients, it offers hope for a safer and more effective treatment.
Funding & Disclosures
The research was conducted by a team from multiple institutions and supported by grants from the Max Planck Society. The authors disclosed no conflicts of interest that might have influenced the study’s outcomes.







