
(© stock.metket.com - stock.adobe.com)
In a nutshell
- America’s deadly overdose epicenter shifted from western to eastern states around 2016, coinciding with fentanyl’s spread and rising Black mortality rates.
- The study identified 27 distinct overdose “hotspots” across the country, with Black communities experiencing a delayed but more severe impact starting after 2013.
- Urban counties dominate high-mortality clusters in eastern states, while rural counties face greater risks in western states—requiring different regional prevention strategies.
CINCINNATI — Every 10 minutes, someone in America dies from an overdose. But this epidemic isn’t static – it’s moving like a storm system across the country, with new hotspots emerging in surprising places and hitting different groups at different times.
New research published in The Lancet reveals a startling pattern: around 2016, America’s deadliest overdose zones began moving from western states to eastern ones. This shift coincided with fentanyl flooding drug supplies and a troubling spike in deaths among Black Americans who had previously experienced lower overdose rates.
According to the paper, we’re not dealing with a single nationwide epidemic but rather numerous localized outbreaks with unique characteristics requiring targeted interventions.
“The epidemic is really a series of mini-epidemics, which we identify as hotspots, across rural and urban America,” said study co-author Neil McKinnon, president of Central Michigan University, in a statement. “We hope our results will assist those in addressing the opioid crisis.”
The Four Waves of America’s Drug Crisis
Researchers from the University of Cincinnati and Central Michigan University examined over 665,000 overdose deaths between 2005 and 2020, using advanced statistical methods to find places where death rates far exceeded normal expectations. They identified 27 distinct overdose “hotspots” across the country, where mortality rates reached nearly 26 deaths per 100,000 person-years – almost double the rate in other areas.
The paper describes the crisis as unfolding in four overlapping waves:
- Wave 1: Prescription painkillers (2000-2016)
- Wave 2: Rising heroin deaths (starting 2007)
- Wave 3: Deadly synthetic opioids like fentanyl (from 2013)
- Wave 4: Post-COVID mixing of multiple substances
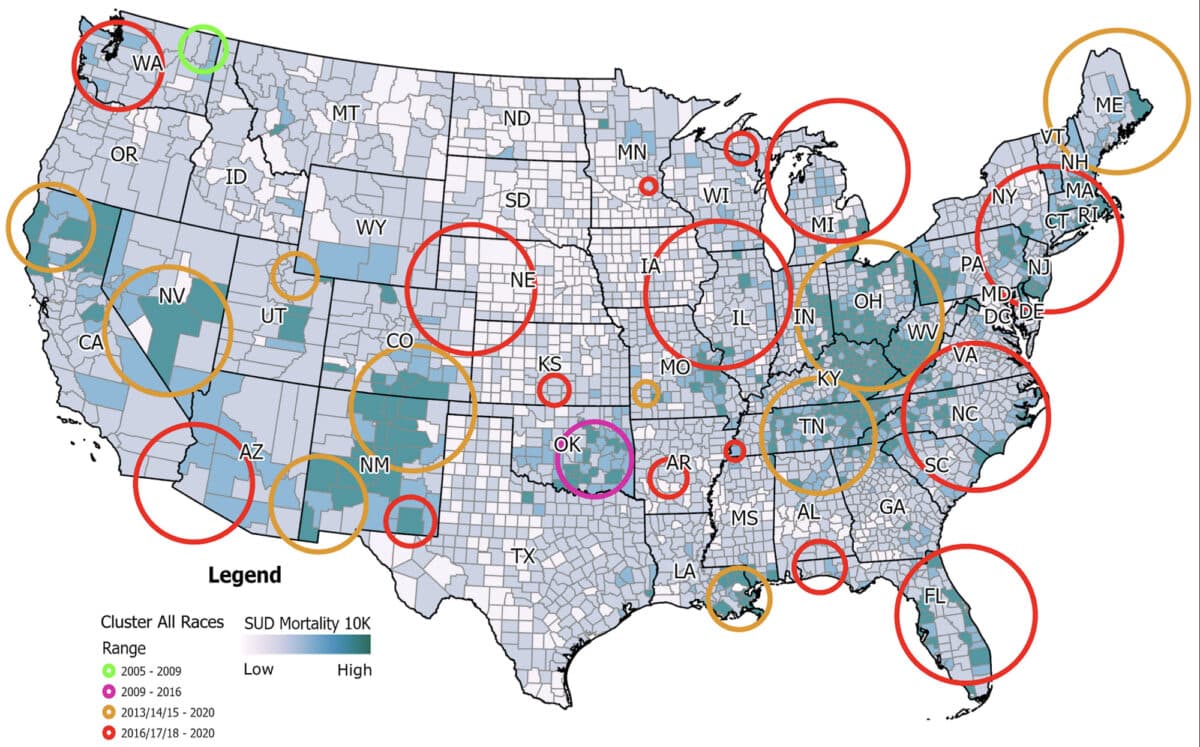
Racial Disparities Reveal a Changing Epidemic
Perhaps most concerning is how the crisis has changed across racial groups. While early phases hit White Americans hardest, the study found that Black Americans have faced an alarming surge since 2013. In some hotspot clusters, Black mortality rates reached 33 deaths per 100,000 person-years – far exceeding the rate outside these zones (13.36).
By 2016, Black Americans were dying at higher rates than Whites, a reversal from earlier patterns. This shift appears connected to the spread of fentanyl, which contaminated eastern drug supplies sooner than western ones.
“As the supply and demand dynamic of the substance evolved, so, too, did the vulnerable populations,” lead author and UC graduate Santiago Escobar said. “The type of substances being abused, as well as the means used to access them, were key determinants of which populations suffered a higher mortality.”
The Urban-Rural Divide
The urban-rural picture adds another layer of complexity. Cities had higher average death rates (1.3 per 10,000 annually versus 1.03 in rural areas). But location matters enormously: in eastern states, urban counties formed the majority of high-mortality clusters, while in western states, rural counties were at greater risk.
This east-west divide likely stems from different drug supply patterns. Eastern markets typically feature powdered heroin from Colombia, which mixes easily with fentanyl. Western markets more commonly have Mexican “black tar” heroin, which is less frequently cut with synthetic opioids.

Study authors suggest that region-specific prevention strategies are needed. Eastern cities might need expanded fentanyl testing, naloxone distribution, and medication-assisted treatment focused on Black communities. Western rural areas might require addressing prescription practices and treatment access in isolated communities.
The research makes one thing painfully clear: America’s overdose crisis isn’t fading – it’s changing form and finding new victims. Our public health response must evolve just as quickly.
Paper Summary
Methodology
Researchers analyzed county-level data on substance use disorder deaths across the continental United States from 2005 to 2020. They focused on deaths coded as unintentional poisonings among people aged 5-84. Using specialized statistical techniques, they identified significant clusters where death rates were much higher than expected for at least two consecutive years. They broke down results by race (White and Black) and whether counties were urban or rural.
Results
The study found 27 distinct overdose hotspots that mostly emerged after 2013 and continued through 2020. Around 2016, these clusters shifted from western to eastern regions. In white communities, 26 clusters had death rates averaging 28.42 per 100,000 person-years, compared to 14.83 in non-cluster areas. Black communities saw 17 clusters with even higher death rates (33.16 per 100,000 person-years vs. 13.36 outside). Urban areas had higher overall death rates, but western rural counties were more likely to form clusters than eastern ones, suggesting geographic influences on risk factors.
Limitations
The researchers acknowledge several limitations. Using standard medical codes for overdose deaths may introduce errors since substances are sometimes misidentified. As a population-level study, findings show broad patterns rather than individual risks. The analysis doesn’t account for specific drug types or examine how race and urban-rural status might interact.
Publication Information
The study, “Spatiotemporal analysis of substance use disorder mortality in the United States: an observational study of emerging hotspots and vulnerable populations (2005–2020),” was authored by Santiago Escobar, Neil J. MacKinnon, Preshit Ambade, Zach Hoffman, and Diego F. Cuadros. It appears in The Lancet Regional Health – Americas, volume 45, May 2025, article 101075. The study received no specific funding from any source.







