
(© Prostock-studio - stock.adobe.com)
In A Nutshell
- Researchers used a machine learning model to rank all 50 U.S. states and Washington, D.C. by socioeconomic vulnerability to flu-like illness, finding wide regional variation in risk.
- Washington, D.C. topped the list, followed by Massachusetts, Hawaii, New Mexico, and Rhode Island: states that reached the highest tier for different socioeconomic and demographic reasons.
- Migration patterns were the strongest predictor of vulnerability, while states with more uninsured residents paradoxically reported lower flu rates, likely because uninsured people avoid testing and formal diagnosis.
- Researchers say the framework could help direct vaccines and public health resources to the most vulnerable communities before flu season begins.
Researchers have used machine learning to score every U.S. state on socioeconomic vulnerability to flu-like illness, and the results do not look anything like what most people would expect. Washington, D.C. ranked as the most at-risk place in the country. Massachusetts and Hawaii were not far behind. Meanwhile, states often associated with poverty and limited healthcare, like Mississippi and Wyoming, scored among the least vulnerable.
A team at Washington University in St. Louis built the map by feeding 39 social and economic data points into a machine learning model, letting the algorithm determine which factors are most strongly associated with flu rates at the state level. Flu costs the United States an estimated $11.2 billion annually in medical expenses and lost productivity, according to the study, and that burden is not shared equally across state lines.
How the AI Flu Map Was Built
Public health officials have long relied on a tool from the Centers for Disease Control and Prevention called the Social Vulnerability Index, originally built to assess disaster preparedness for floods and hurricanes. Researchers at Washington University say the index is designed for disasters and may miss factors that matter specifically for infectious disease, because a pandemic and a hurricane hit communities through completely different mechanisms.
Their alternative pulled 39 indicators from U.S. Census data and CDC flu surveillance records, covering everything from income and housing to race, employment, and healthcare access. A type of machine learning called a Random Forest model, which runs hundreds of simulations and weighs their combined results, ranked which of those factors most strongly predicted flu rates at the state level. After removing indicators that overlapped too much with each other, the model settled on 22 variables. It used 2022 peak weekly flu infection data from the CDC, adjusted for state population size to allow fair comparisons across all 50 states and Washington, D.C. Results were published in PLOS Computational Biology.
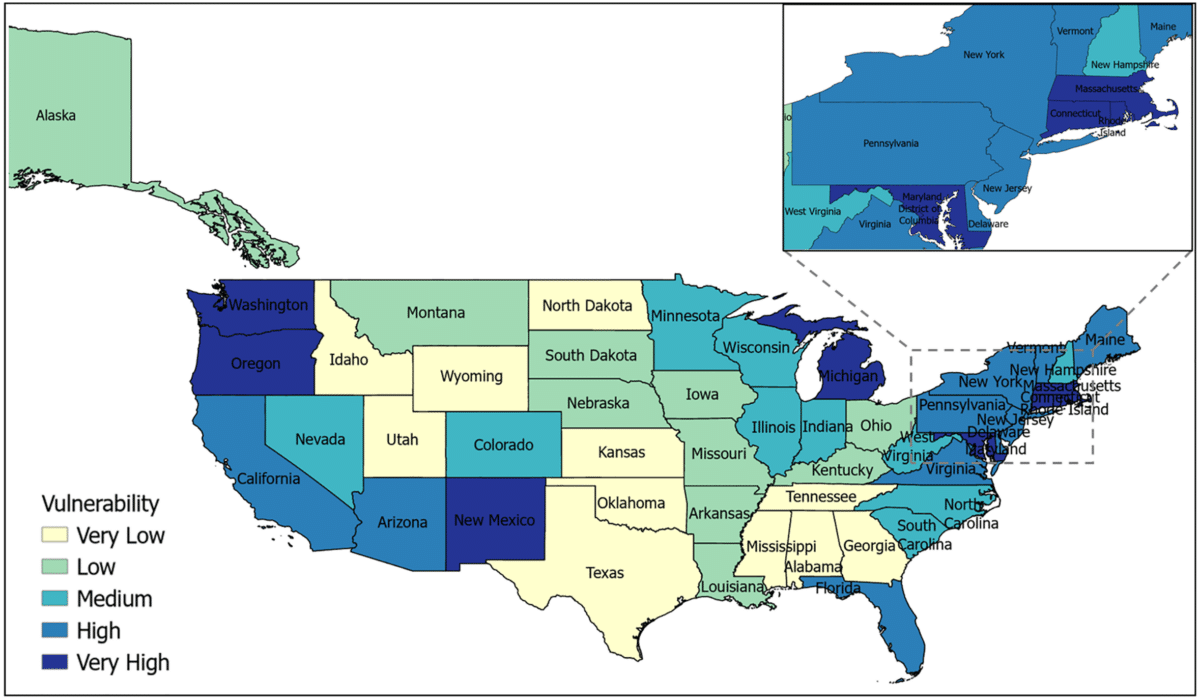
States are classified as follows (normalized indices in parentheses): Very Low (0.0–0.13), Low (0.13-0.21), Medium (0.21-0.28), High (0.28-0.35), and Very High (0.35–1.0). The maps were generated in ArcGIS Pro using shape files from the U.S. Census Bureau. Credit: Chakrabarty et al. PLOS Computational Biology, doi.org/10.1371/journal.pcbi.1013839.g002
Why D.C. Tops the List, and Why That Makes Sense
Washington, D.C. topping a flu vulnerability ranking can seem counterintuitive. It has well-funded hospitals, solid vaccination rates, and healthcare access that many rural states cannot match. But the model identified a different set of problems: extreme population density, long daily commutes that pack people together, and a large share of foreign-born residents without health insurance. Those conditions create serious transmission risk regardless of how good the nearest hospital is.
All told, 11 states and Washington, D.C. landed in the highest vulnerability tier. Alongside D.C., that group includes Massachusetts, Hawaii, New Mexico, Rhode Island, Connecticut, Maryland, Oregon, Washington, Michigan, and Arizona. Each got there by a different route. New Mexico’s score was driven by an aging population, a large share of Hispanic and American Indian residents, high poverty rates, and limited access to computers and digital health information. Massachusetts scored high despite its robust healthcare system, pushed there mainly by dense population and high migration rates. Michigan, researchers noted, faces a dual problem: fast-spreading transmission in dense urban centers and rural communities with older, medically underserved populations.
A Surprising Finding About the Uninsured
One of the more unexpected patterns involves health insurance. States with higher rates of uninsured residents actually reported lower flu-like illness rates, the reverse of what most health equity data would suggest.
Researchers suggest the pattern may reflect testing and diagnosis behavior. Without insurance, people tend to skip doctor visits and avoid formal diagnosis, meaning their illnesses never get counted. A similar pattern appeared for chronic conditions like asthma and diabetes. Researchers suggest that higher health awareness among people with those conditions may lead to more preventive behavior, which could keep their reported infection rates below those of the general population.
Both patterns point to the same underlying problem: official flu surveillance likely undercounts the true burden in states with high uninsured populations, which skews how those states appear on any vulnerability assessment.
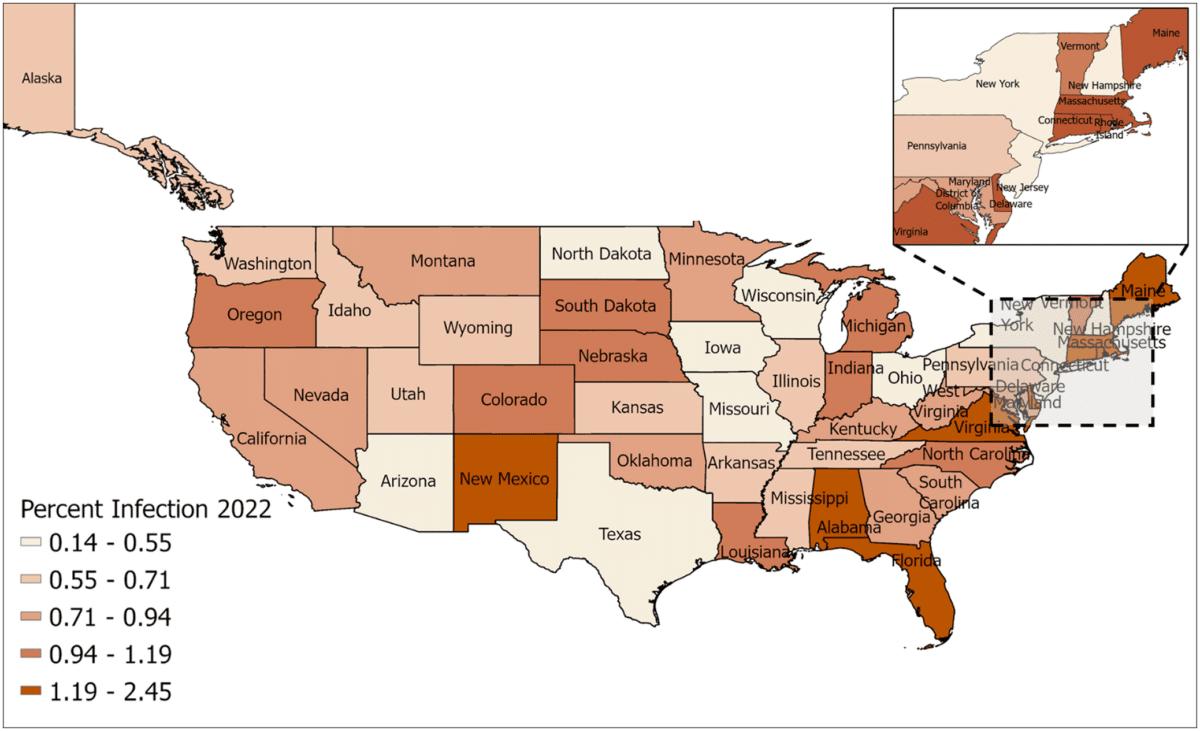
The maps were generated using ArcGIS Pro using shape files from the U.S. Census Bureau. Credit: Credit: Chakrabarty et al. PLOS Computational Biology, doi.org/10.1371/journal.pcbi.1013839.g002
What Drives a State’s Score
Migration patterns carried the most weight in the model. States with larger shares of recently arrived international residents consistently scored more vulnerable, consistent with previous research linking immigration status to barriers in healthcare access. The share of female residents was also strongly associated with vulnerability scores, as was the proportion of residents over 65. Adult vaccination rates ranked among the strongest predictors as well.
Lower-vulnerability states tended to have higher insurance coverage, lower levels of recent international migration, and lower population density. Wyoming and Mississippi fell into the lowest vulnerability tier, while Texas, Oklahoma, and Georgia landed in the low to medium range. Even so, researchers flagged that Texas, Oklahoma, Mississippi, Georgia, and Wyoming all had high rates of uninsured non-citizens, a pocket of risk that a statewide score would not immediately reveal.
Researchers say vulnerability maps like this could help guide more targeted public health planning, directing vaccines, telehealth resources, and outreach programs to the communities that need them most before flu season begins, not after the damage is already done.
Disclaimer: This article is based on a peer-reviewed study and is intended for general informational purposes only. It does not constitute medical advice. The vulnerability scores described reflect socioeconomic and demographic factors associated with flu-like illness rates and are not a prediction of individual health outcomes. Consult a qualified healthcare provider for personal health guidance.
Paper Notes
Study Limitations
Researchers acknowledge several constraints. Most significantly, the analysis operates at the state level, which is a fairly coarse geographic unit. Socioeconomic conditions and vulnerability can vary sharply between counties, cities, or even neighborhoods within the same state, and those differences are not captured here. The study also relies on 2022 data only, reflecting a single flu season, and does not account for how vulnerability patterns might shift across different years or flu strains. Working with 50 states plus D.C. as regional units limits the model’s predictive precision, and researchers note that a different variable set could produce a different map. Future work, they suggest, should aim for finer geographic resolution and draw on multiple flu seasons.
Funding and Disclosures
This work was supported by FluLab (grant GR0031819 to Rajan K. Chakrabarty and John R. Cirrito), Washington University’s Transdisciplinary Institute in Applied Data Sciences (TRIADS) Seed Grant program, and the WashU-IITB Joint Research and Education Initiative. Funders had no role in study design, data collection, analysis, the decision to publish, or preparation of the manuscript. Authors declared no competing interests.
Publication Details
Authors: Shrabani S. Tripathy, Joseph V. Puthussery, Taveen S. Kapoor, John R. Cirrito, and Rajan K. Chakrabarty. Tripathy, Kapoor, and Chakrabarty are affiliated with the Center for Aerosol Science and Engineering, Department of Energy, Environmental and Chemical Engineering, Washington University in St. Louis. Puthussery holds additional affiliation with the Department of Civil Engineering, Indian Institute of Technology Delhi. Cirrito and Puthussery are affiliated with the Department of Neurology, Hope Center for Neurological Disease, Knight Alzheimer’s Disease Research Center, Washington University in St. Louis. | Journal: PLOS Computational Biology | Title: “Spatial variation in socio-economic vulnerability to Influenza-like Infection for the US population” | Published: January 28, 2026 | DOI: https://doi.org/10.1371/journal.pcbi.1013839








Does not make sense. The algorithm is basically focused on the percentage of folks who have health insurance. Obviously whomever put the study together forgot to do a factor analysis first.