(© Sherry Young - stock.adobe.com)
In A Nutshell
- Metformin, a common diabetes medication costing less than $10 monthly, was linked to 37% fewer cases of progression to intermediate macular degeneration over five years.
- The study tracked over 2,000 people with diabetes using detailed eye photographs, a more accurate method than previous research relying on insurance claims.
- Laboratory studies suggest metformin may protect the retina through anti-inflammatory effects and by helping cells clear out cellular damage, though this hasn’t been proven in humans with AMD.
- Researchers are calling for a randomized clinical trial to definitively determine whether metformin can prevent vision loss in people with early or intermediate macular degeneration.
Millions of people with diabetes take metformin every day to manage their blood sugar, typically spending less than $10 a month for the generic version. Now researchers have found the drug might also help protect against progression to a vision-threatening stage of a leading cause of blindness in older adults. In a five-year study of more than 2,000 people, those taking metformin were 37% less likely to develop a dangerous stage of age-related macular degeneration.
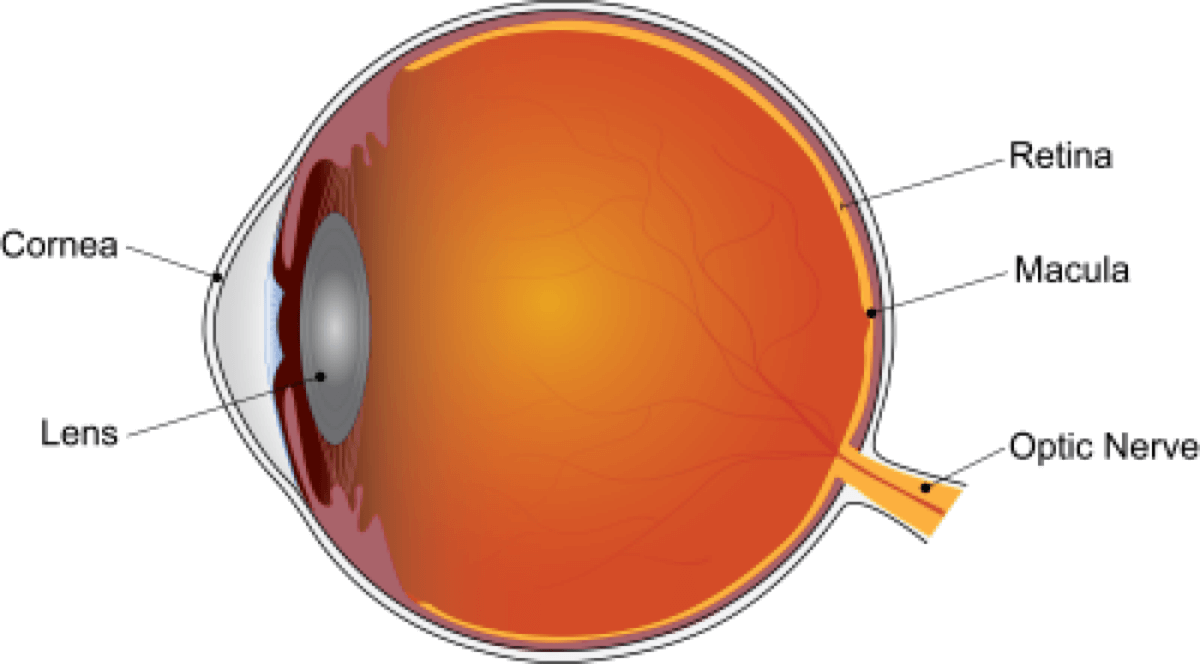
Age-related macular degeneration slowly destroys the central part of your vision, the part you need to read, drive, and recognize faces. It’s one of the most common causes of blindness in wealthy nations. Treatments for advanced stages cost thousands of dollars and don’t work well long-term. Finding a cheap, safe drug that could slow the disease before serious vision loss would change everything about how doctors handle this condition.
Researchers from the University of Liverpool took advantage of a unique opportunity. People with diabetes in Liverpool get their eyes photographed annually to check for diabetes-related damage. The scientists realized they could look at these same photos to track macular degeneration at the same time. They randomly selected 2,545 people aged 50 and older who had clear eye photos from 2011, then checked back in 2016 to see whose vision had worsened.
What the Photos Revealed About Vision and Metformin
Of the 2,545 people who started the study, 2,089 came back five years later with clear photos. About 40% had been taking metformin throughout. An eye specialist reviewed thousands of photos, looking for yellow deposits called drusen that build up under the retina, pigment changes, and damage to the central part of the eye.
The disease moves through stages. Early on, small deposits appear but vision stays normal. In the intermediate stage, the last stop before advanced disease steals sight, larger deposits accumulate and pigment changes become visible. Late-stage disease involves either abnormal blood vessels leaking fluid or patches of dead retinal tissue.
Here’s what caught researchers’ attention: people taking metformin were far less likely to hit that intermediate stage. Even after accounting for age, blood sugar control, and diabetes duration, metformin users still showed protection.
A 37% Drop in Risk, But Questions Remain
The research, published in BMJ Open Ophthalmology, also looked at late-stage disease, but with only 44 people reaching that point, the numbers were too small to draw firm conclusions. Metformin didn’t affect the earliest stage either, which makes sense since the disease may not have progressed far enough yet.
It’s important to note the caveat that people not taking metformin had more eye damage at the start, which could make them more likely to worsen regardless of medication. That’s why researchers are calling for a randomized clinical trial where people would be assigned to take either metformin or a placebo.
Why a Diabetes Drug Might Save Your Vision
Metformin has been grabbing attention lately for effects beyond blood sugar control. Laboratory studies suggest it acts like an antioxidant, tamps down inflammation, and helps cells clean up their internal garbage. All of these could theoretically benefit the retina, the light-sensitive tissue at the back of your eye.
Think of your retinal cells like tiny factories that need regular maintenance. As we age, cells get worse at taking out the trash: damaged proteins and defective parts pile up. Animal and cell studies indicate metformin may boost this cellular housekeeping system. In lab experiments with retinal cells, adding metformin helped the cells survive damage and cleared out the molecular junk that would otherwise accumulate and cause problems.
Inflammation plays a role too. Chronic, low-grade inflammation contributes to many aging-related diseases, and macular degeneration is no exception. The yellow deposits that pile up under the retina are partly driven by inflammatory processes. Laboratory research suggests metformin may dial down these inflammatory signals. Computer analyses that match drugs to diseases based on their genetic profiles have repeatedly flagged metformin as a strong candidate for treating macular degeneration.
Building on Previous Clues
This isn’t the first hint that metformin might protect vision. Earlier studies involving millions of people found that those taking metformin had lower rates of macular degeneration. But nearly all those studies relied on insurance claims or billing codes to identify who had the disease. These records often miss milder cases and don’t distinguish between the different stages, making them less reliable than actually looking at eye photographs.
One small trial tested metformin in 66 people who already had advanced macular degeneration with significant vision loss. The drug didn’t slow the disease at that point. But that doesn’t contradict the new findings: by the time you’ve reached late-stage disease, the damage may be too far gone. Metformin might work better as prevention, stopping people from reaching that point in the first place.
What We Still Don’t Know
The study didn’t track metformin dosage, how long people had been taking it before 2011, or consistency of use. It also lacked information about diet and vitamin supplements. And because everyone in the study had diabetes, whether metformin would help people without the disease remains unknown. This observational study can spot associations but can’t prove cause and effect the way a randomized trial can. Still, the biological mechanisms make sense, and the drug’s decades-long safety record supports moving forward with a proper trial.

What This Means for Preventing Vision Loss
Right now, people with intermediate AMD have limited options beyond vitamin supplements, which show only modest effects. No approved medications exist to prevent the disease from worsening before vision loss begins. Catching and stopping the disease at this stage could offer benefits that treating late-stage damage cannot.
A randomized trial could determine whether metformin truly prevents progression. Such a trial would assign people with early or intermediate AMD to receive either metformin or a placebo, then track their disease over several years. If the drug reduces progression by a third or more, it would offer millions of older adults an affordable, accessible way to protect their sight. For the estimated 196 million people worldwide affected by AMD, that could mean preserving vision before it’s too late. Whether metformin works in people without diabetes remains to be seen, but this study makes a strong case for finding out.
Disclaimer: This article reports on observational research findings and is intended for informational purposes only. It is not medical advice. People taking metformin should not change their medication regimen without consulting their healthcare provider. Those not currently taking metformin should not start taking it based solely on this research, as the findings have not been confirmed in randomized clinical trials and the study involved only people with diabetes. Always consult with a qualified healthcare professional before making any decisions about your medical treatment.
Paper Notes
Study Limitations
The research team acknowledges several important limitations to their work. As an observational study, baseline differences existed between people taking metformin and those who weren’t, particularly in AMD severity at the study’s start. People not on metformin had significantly more AMD initially, making progression more likely. Though researchers adjusted for these differences statistically, unmeasured confounding factors could still influence the results. The study lacked data on metformin dosage, duration of prior use, and medication compliance. Information about diet and use of AREDS supplements wasn’t available from general practitioner records. The number of participants who developed late-stage AMD was relatively small, limiting statistical power to detect effects at that stage. Smoking data had substantial missing values and combined current and former smokers into one category. All participants had diabetes, so generalizability to people without diabetes remains uncertain. Finally, optical coherence tomography would have provided better sensitivity for detecting AMD than the color fundus photographs used.
Funding and Disclosures
Dewi Fathin Romdhoniyyah received funding from The Ministry of Finance of the Republic of Indonesia through Indonesia Endowment Fund for Education (LPDP) scholarship for doctoral study, grant number 201711220412052. The data used came from the Individualised Screening for Diabetic Retinopathy (ISDR) study, funded by NIHR Programme Development Grant (reference RP-DG-0709-10138) and NIHR Five Year Programme of Applied Research (reference RP-PG-1210-12016). Simon Harding serves as Chief Medical Officer of AI-Sight, which offers an artificial intelligence system for diabetic retinal screening. Nicholas Beare has received travel expenses from Bayer. The other authors declared no conflicts of interest.
Publication Details
Authors: Dewi Fathin Romdhoniyyah, Ayesh Alshukri, David G Parry, Simon Harding, Nicholas A V Beare | Affiliations: Eye and Vision Science, University of Liverpool; Department of Ophthalmology, Universitas Gadjah Mada, Yogyakarta, Indonesia; Liverpool Ophthalmic Reading Centre, Liverpool University Hospitals NHS Foundation Trust; St Paul’s Eye Unit, Liverpool University Hospitals NHS Foundation Trust | Journal: BMJ Open Ophthalmology, Volume 11, 2026 | Title: Metformin and incidence of age-related macular degeneration in people with diabetes: a population-based 5-year case-control study | DOI: 10.1136/bmjophth-2025-002339 | Received: June 5, 2025; Accepted: January 18, 2026; Published: February 2, 2026 | The research data supporting this study’s findings are publicly available at the University of Liverpool Research Data Catalogue.







