(© Alex - stock.adobe.com)
In A Nutshell
- Big picture: A large Swedish study tracked nearly 150,000 people with ADHD and found those on medication had fewer serious outcomes beyond attention issues.
- Key findings: Estimated reductions included 17% fewer suicidal behaviours, 15% fewer cases of substance misuse, 13% fewer criminal convictions, and 12% fewer transport accidents in first events.
- Details: Benefits were generally greater for people who had already experienced these problems, and stimulants outperformed non-stimulants in most comparisons.
- Caveats: Results are based on statistical estimates, not direct cause-and-effect proof, and may not apply the same way outside Sweden.
STOCKHOLM — A huge Swedish study suggests ADHD medicines may do more than help with focus. Scientists say they might also be linked to fewer serious problems like suicidal behavior, substance misuse, and trouble with the law.
Researchers followed nearly 150,000 people with ADHD for two years, comparing those who started medication soon after diagnosis with those who didn’t. Based on their analysis, the medicated group experienced an estimated 17% fewer suicidal behaviors, 15% fewer cases of substance misuse, 13% fewer criminal convictions, and 12% fewer traffic accidents in first-time events. These percentages come from the study’s statistical results, not direct headcounts, so they should be seen as careful estimates. There was no clear overall reduction in first accidental injuries.
Many patients and caregivers may not fully understand the potential risks and benefits of ADHD drug treatment, the authors note. This lack of awareness was a key motivation for doing the research.
How the Study Worked
Instead of running a traditional clinical trial, the Karolinska Institutet-led team used Sweden’s national health and crime registers, which track prescriptions, hospital visits, and even criminal convictions for the whole population.
They identified everyone aged 6–64 who was newly diagnosed with ADHD between 2007 and 2018. About 57% began medication within three months, and 43% didn’t. Both groups were followed for two years to track suicidal behaviors, substance misuse, accidental injuries, traffic accidents, and criminal convictions.
The researchers used advanced statistical techniques designed to make the comparison between medicated and non-medicated groups as fair as possible.
What They Found
In just two years, the numbers added up:
- Suicidal behaviors: 4,502 people affected
- Substance misuse: 17,347 people affected
- Accidental injuries: 24,065 people affected
- Automobile accidents (age 15+): 4,345 people affected
- Criminal convictions (age 15+): 11,248 people affected
When comparing the two groups, medication was linked to lower rates for most outcomes. Among people with a history of suicidal behavior, the estimated drop was around 21%, compared to 13% for those without such a history.
For accidental injuries, there was no significant difference for first events overall. In people with no prior injuries, the analysis suggested a very small increase (about 1%), but it wasn’t statistically meaningful.
When looking at repeat events, medication was linked to fewer incidents across all five outcomes.
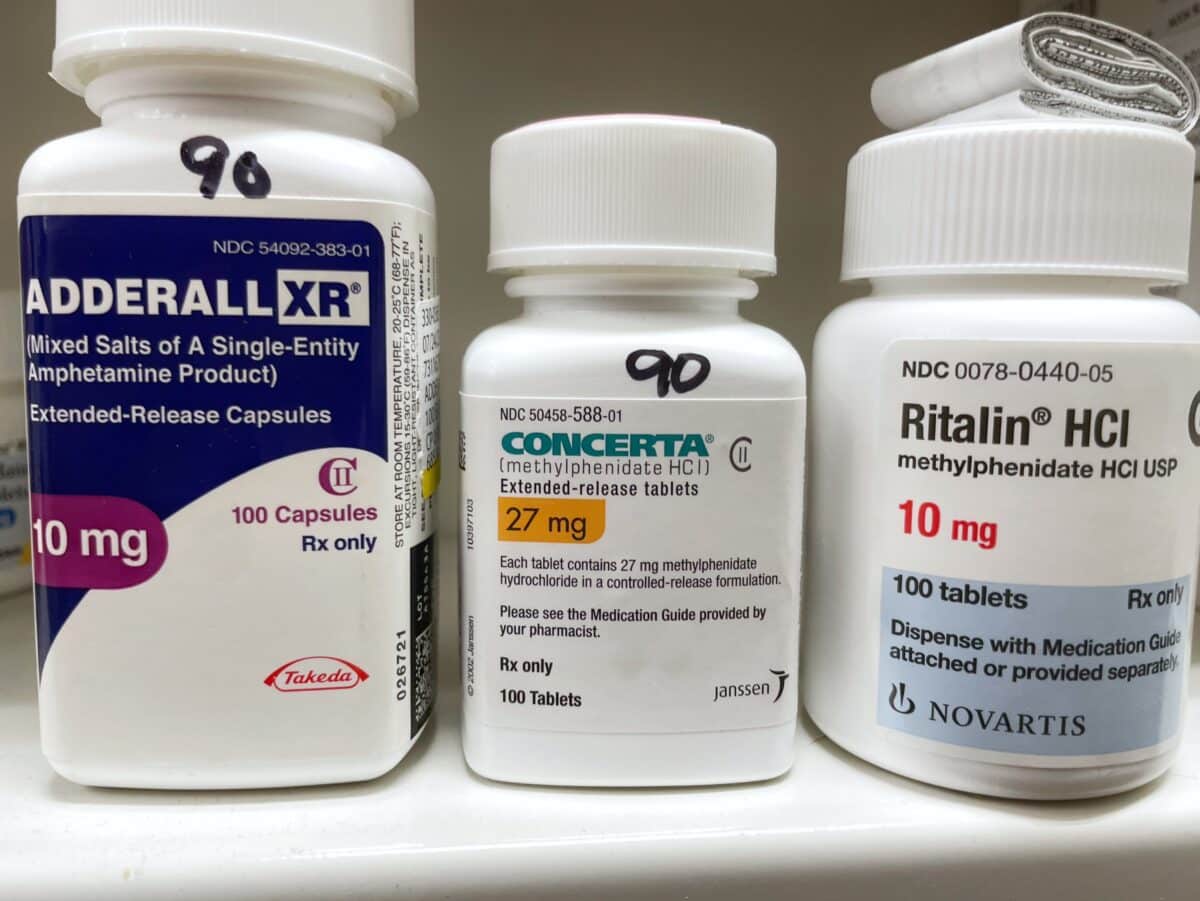
Stimulants Outperform Non-Stimulants
Most people (about 88%) started on stimulants like methylphenidate (Ritalin). In head-to-head comparisons, stimulants generally outperformed non-stimulants such as atomoxetine. For substance misuse, stimulants were linked to an estimated 26% fewer first episodes than non-stimulants.
Adults tended to see bigger benefits than children for substance misuse and criminal convictions. For first criminal convictions, women showed a stronger reduction than men, though both benefited overall.
Why This Matters — and the Caveats
The study can’t prove medication directly caused these reductions. It also didn’t track whether people took the drugs exactly as prescribed, changes in dosage, or other treatments like therapy. And because the data came from Sweden’s healthcare system, results might differ in other countries.
To test their methods, the researchers looked at people with Type 1 diabetes and found no link, suggesting their approach wasn’t producing false results.
While these estimated percentages may not sound huge, across a whole population they could mean thousands fewer harmful events. The findings hint that ADHD medication might have wider benefits than many people realize.
Disclaimer: This article is for informational purposes only and is not a substitute for professional medical advice, diagnosis, or treatment. Always seek the guidance of a qualified healthcare provider with any questions about ADHD, medications, or changes to your treatment plan.
Paper Summary
Methodology
The researchers used Swedish national health registers to conduct a study that mimics a randomized controlled trial using observational data. They identified 148,581 people aged 6-64 who received new ADHD diagnoses between 2007-2018 and divided them into two groups: those who started medication within three months (56.7%) and those who didn’t (43.3%). The team used sophisticated statistical techniques including “cloning, censoring, and inverse probability weighting” to eliminate bias and account for differences between groups. Participants were followed for two years, with researchers tracking five outcomes through national registers covering healthcare, crime, and death records.
Results
ADHD medication was associated with reductions in four of five adverse outcomes for first-time events: 17% reduction in suicidal behaviors, 15% reduction in substance misuse, 13% reduction in criminality, and 12% reduction in transport accidents. Accidental injuries showed no reduction for first events. For recurrent events, medication was protective against all five outcomes, with reductions ranging from 4% to 25%. Stimulant medications consistently outperformed non-stimulants across all outcomes. The protective effects were more pronounced in people with previous histories of these events and varied by age and gender for some outcomes.
Limitations
The study couldn’t account for non-drug treatments like psychotherapy, so comparisons reflect medication versus “usual care” rather than no treatment. Researchers couldn’t measure actual medication adherence, dosage variations, or ADHD symptom severity. The results might not apply to healthcare systems with different prescribing patterns. Some outcomes might be underestimated if they don’t result in medical or legal attention. Despite sophisticated statistical controls, unmeasured confounding factors like genetics, family support, or lifestyle differences could still influence results.
Funding and Disclosures
The study was supported by multiple Swedish research councils and foundations. Several authors reported financial relationships with pharmaceutical companies, including receiving speaker fees from companies that manufacture ADHD medications, though these relationships were described as outside the submitted work.
Citation
Zhang L, Zhu N, Sjölander A, et al. ADHD drug treatment and risk of suicidal behaviours, substance misuse, accidental injuries, transport accidents, and criminality: emulation of target trials. BMJ. 2025;390:e083658.







