
(Credit: LightField Studios on Shutterstock)
Caring for a Loved One May Slow or Speed Mental Decline, Depending on the Burden
In A Nutshell
- People who provided light caregiving duties showed slower mental decline than non-caregivers, pointing to a possible brain-protective effect at manageable levels.
- Those providing very intensive care, caring for a spouse or partner, or caring for someone in their household experienced faster cognitive decline than non-caregivers.
- Neither gender nor household wealth changed these results, meaning the cognitive effects of caregiving appeared consistent across different groups.
- Whether caregiving helps or hurts cognitive health depends heavily on how much care is being provided and the relationship between caregiver and recipient.
For millions of Americans, taking care of an aging parent, a sick spouse, or an ailing friend is simply part of life. But a new study finds that not all caregiving is created equal, and that how much care someone provides, and for whom, may be linked to how their memory and thinking skills change as they age.
Researchers tracking older adults in England over nearly two decades found that people who took on lighter caregiving duties, say a few hours a week helping an elderly parent, actually showed slower mental decline compared to people who weren’t caregivers at all. But those who provided very intensive care, cared for someone in their household, or cared for a spouse or partner showed the opposite: their cognitive test scores declined faster than non-caregivers.
Whether caregiving is good or bad for the caregiver’s own mind appears to depend entirely on the situation.
A Long Look at Caregivers Over Time
Published in the journal Age and Ageing, the study drew from a large, long-running survey called the English Longitudinal Study of Ageing, which tracks people aged 50 and older in private households across England. Researchers used data from nine rounds of interviews spanning 2004–2005 through 2021–2023.
To make a fair comparison, the team paired 2,765 caregivers with 2,765 non-caregivers who had similar backgrounds, matching them on factors like age, sex, health conditions, education, wealth, and relationship status. Caregivers in the study were, on average, 60 years old, and 56% were women.
Cognitive ability was tracked two ways. One test, naming as many animals as possible in one minute, served as a rough measure of executive function, the set of skills involved in organizing thoughts, switching between ideas, and solving problems. Researchers note the test captures only part of that broader skill set. A second test measured memory by having participants learn a list of ten words and recall them immediately and after a short delay. Both tests were repeated across multiple rounds, allowing the team to track how each person’s scores changed before and after they became a caregiver.
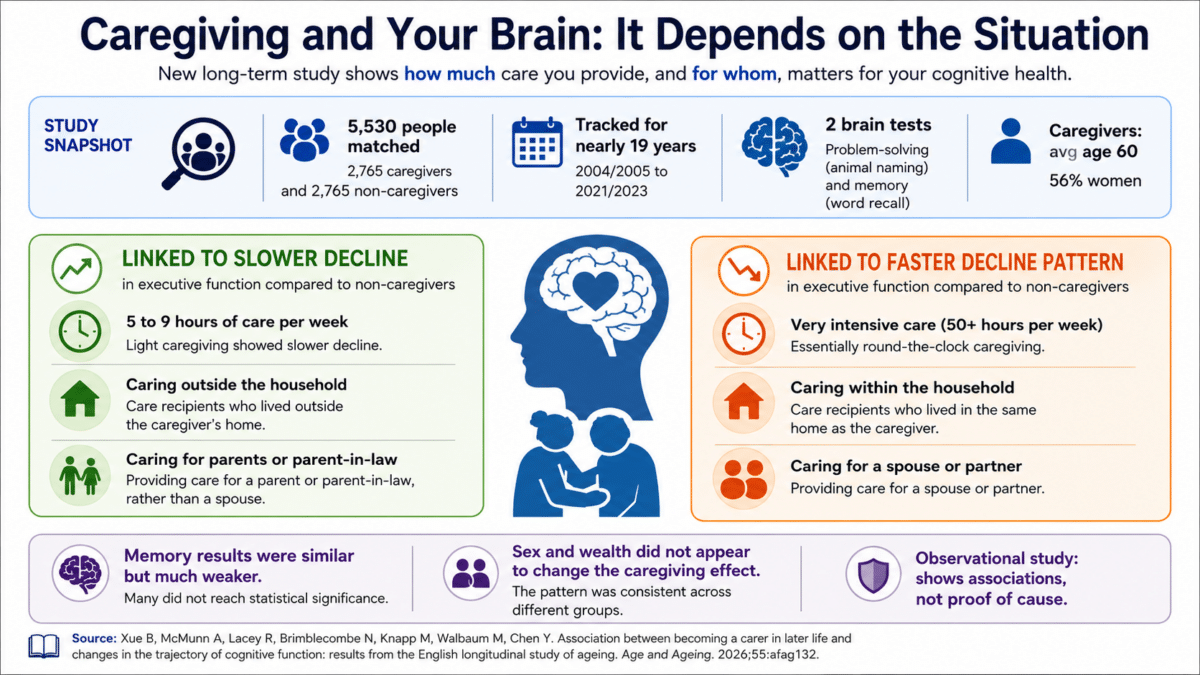
It’s Not Just Whether You Care, It’s How Much, and for Whom
When researchers looked at all caregivers as one group, they found no meaningful difference in cognitive decline compared to non-caregivers. Once they broke the data down by the type of caregiving, a far more revealing picture emerged.
People who provided between 5 and 9 hours of care per week showed a noticeably slower drop in executive function scores compared to non-caregivers. Those caring for a parent or parent-in-law also fared better cognitively, and caregivers helping someone who lived outside their own home showed slower decline than those providing care under their own roof.
On the other side, those caring inside the household or for a spouse or partner showed faster cognitive decline than non-caregivers, with statistically reliable results. Those providing 50 or more hours of care per week showed a similar pattern, though that result was somewhat weaker statistically. Caregivers in these situations tend to shoulder the heaviest burdens, often with little time off and limited ability to keep working. Memory followed a similar trajectory, though those effects were much weaker overall.
Too Much Caregiving Cancels Out the Mental Benefits
Researchers point to two competing theories. One, sometimes called the “use it or lose it” idea, holds that staying mentally and socially engaged helps keep the mind sharp. Light caregiving may provide exactly that stimulation: problem-solving, communicating, coordinating care, and staying attuned to another person’s needs.
That protective effect appears to have a breaking point. When caregiving becomes all-consuming, dominating a person’s days, disrupting sleep, and cutting them off from social connections and paid work, the toll may outweigh any cognitive benefits. Researchers tie this to the “stress process” framework, the idea that chronic, high-level stress wears down health over time. As the authors put it: “While caring may help preserve cognitive function, excessive caring demands appear to accelerate cognitive decline.”
Who Is Most at Risk, and What Families Should Know
The negative effects of intensive caregiving were not more pronounced for women or for people with less money. Women do disproportionately take on caregiving roles, the researchers noted, but the effect on cognitive test scores appeared similar regardless of gender or household wealth. People with lower wealth still started the study with lower cognitive scores overall, a gap present from the start, even if the caregiving effect itself didn’t differ by wealth.
People who had been caregiving for three or more years showed a slightly slower rate of memory decline, though the authors caution that this finding warrants careful interpretation. Longer-term caregivers may have built better support systems over time, or people with emerging cognitive difficulties may simply have stopped caregiving before reaching that mark.
With projections suggesting about one in five adults in England will be living with a serious illness by 2040, and similar aging pressures building across much of the developed world, the pool of family caregivers is expected to grow. Helping them keep responsibilities at a manageable level, rather than absorbing more and more hours without relief, may be one of the most important things families, doctors, and policymakers can do to protect cognitive health in an aging population.
Disclaimer: This article is based on an observational study and is intended for general informational purposes only. The research identifies associations between caregiving patterns and cognitive changes but does not prove that caregiving directly causes those changes in any individual. Consult a qualified health professional for personal medical advice.
Paper Notes
Limitations
Researchers acknowledge several important limitations. Care information was based on what participants reported doing in the past week, which is sensitive to short-term changes and may not accurately reflect longer-term patterns. The dataset also lacked information on participants’ caregiving history before they entered the survey, and the study did not include details about the specific health conditions of the people being cared for. Because findings relied on self-reported data, some participants may not have identified themselves as caregivers even when providing care. The animal-naming task may capture only part of what researchers consider executive function, rather than the full range of those mental abilities. People with dementia, or those providing very intensive care, may have been less likely to continue participating in the survey over time, which could have introduced bias into the results. The study also did not examine what happens to a person’s cognitive health after they stop caregiving, which the authors flag as an important area for future research.
Funding and Disclosures
The project was funded by the Joint Programming Initiative More Years Better Lives through the UK Economic and Social Research Council (grant ES/W001454/1), Equalise: The ESRC Centre for Lifecourse Health Equity (grant ES/Z504270/1), and the Wellcome Trust (grant 227639/Z/23/Z). No conflicts of interest were declared by the authors.
Publication Details
Authors: Baowen Xue, Anne McMunn, Rebecca Lacey, Nicola Brimblecombe, Martin Knapp, Magdalena Walbaum, and Yuntao Chen. Xue, McMunn, and Chen are affiliated with University College London; Lacey is affiliated with City St George’s, University of London; and Brimblecombe, Knapp, and Walbaum are affiliated with the Care Policy and Evaluation Centre at the London School of Economics and Political Science. | Journal: Age and Ageing | Paper Title: “Association between becoming a carer in later life and changes in the trajectory of cognitive function: results from the English longitudinal study of ageing” | DOI: https://doi.org/10.1093/ageing/afag132 | Published: 2026, Volume 55, article identifier afag132. Open-access article published under a Creative Commons Attribution License.







